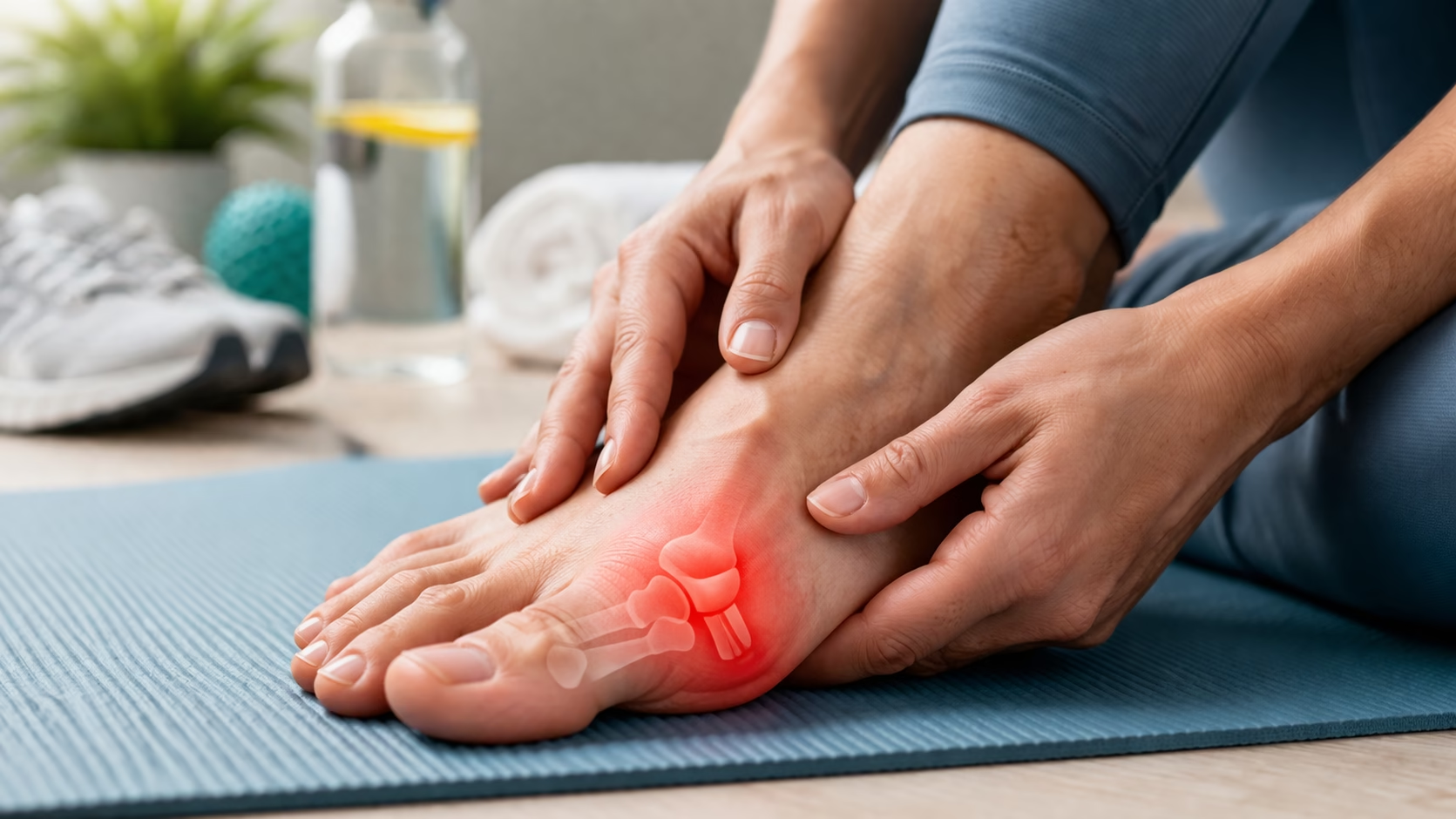
Arthritis affecting the big toe, medically referred to as hallux rigidus, is a progressive degenerative condition that can significantly impair mobility and daily functioning. Although it may initially present as mild stiffness or discomfort, the condition can gradually worsen, leading to persistent pain and restricted joint movement.
Early recognition and a structured treatment approach are essential to slow disease progression, relieve symptoms, and maintain functional independence. This article provides a comprehensive and detailed explanation of the causes, symptoms, and evidence-based treatment strategies for managing arthritis in the big toe.
Understanding Big Toe Arthritis
What Is Hallux Rigidus?
Hallux rigidus is a form of osteoarthritis that specifically affects the metatarsophalangeal (MTP) joint, which connects the big toe to the foot. This joint plays a crucial role in walking, balance, and weight distribution.
The condition develops when the cartilage that cushions the joint gradually deteriorates. As cartilage wears away, bones begin to rub against each other, leading to inflammation, pain, and the formation of bone spurs. Over time, this process reduces joint flexibility and results in stiffness, which is a defining feature of the condition.
Common Symptoms
Joint Stiffness
One of the earliest signs is reduced flexibility in the big toe. Patients may notice difficulty bending the toe upward or downward, particularly during walking.
Swelling and Bony Enlargement
Inflammation of the joint may cause visible swelling or the development of a firm bump on the top of the toe, often due to bone spur formation.
Pain with Movement
Activities such as walking, climbing stairs, or squatting can place pressure on the MTP joint, resulting in pain that may worsen with continued use.
Difficulty Wearing Shoes
Tight or narrow footwear can aggravate symptoms by compressing the inflamed joint, making it uncomfortable to wear certain types of shoes.
Why Early Treatment Matters
Early intervention is critical in managing hallux rigidus. Timely treatment helps preserve remaining cartilage, maintain joint mobility, and reduce inflammation. Furthermore, it can delay or prevent the need for surgical intervention by controlling symptoms in the early stages of the disease.
Lifestyle Modifications
Maintaining a Healthy Weight
Excess body weight increases the mechanical load on foot joints, particularly during weight-bearing activities. Even modest weight reduction can significantly decrease pressure on the big toe joint, thereby alleviating pain and slowing disease progression.
Activity Modification
High-impact activities, such as running on hard surfaces, place repetitive stress on the toe joint and may accelerate cartilage degeneration. Substituting these activities with low-impact exercises, such as swimming or cycling, reduces joint strain while maintaining overall fitness.
Use of Supportive Aids
Assistive devices such as walking poles or canes can help redistribute body weight and reduce pressure on the forefoot. Additionally, shoe inserts with metatarsal pads help shift weight away from the affected joint, providing relief during movement.
Footwear and Orthotics
Choosing Appropriate Footwear
Footwear plays a central role in managing symptoms. Shoes with firm, supportive soles help limit excessive motion at the big toe joint, thereby reducing irritation. A wide and deep toe box accommodates swelling and prevents compression of the joint. Low-heeled shoes minimize forward pressure on the forefoot, further reducing discomfort.
Orthotic Devices
Custom or over-the-counter orthotics can provide structural support to the foot. Rigid or semi-rigid insoles limit joint motion and prevent excessive bending, while metatarsal pads support the arch and redistribute weight toward less affected areas of the foot.
Practical Shopping Considerations
It is advisable to shop for shoes later in the day when feet are slightly swollen, ensuring a comfortable fit throughout daily activities. Regular measurement of foot size is also important, as changes can occur over time due to aging or structural alterations.
Physical Therapy and Home Exercises
Stretching and Range-of-Motion Exercises
Gentle stretching exercises help maintain joint flexibility and reduce stiffness. For example, manually extending the big toe upward for short intervals can improve range of motion and reduce discomfort.
Strengthening Exercises
Exercises such as picking up small objects with the toes or performing resistance-based movements enhance muscle strength around the joint. Strengthening the surrounding structures improves joint stability and reduces mechanical stress.
Professional Rehabilitation
A physical therapist can design individualized exercise programs tailored to the severity of the condition. They may also provide manual therapy and gait correction techniques to optimize movement patterns and reduce joint strain.
Medications and Injections
Over-the-Counter Pain Relievers
Nonsteroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen or naproxen are commonly used to reduce pain and inflammation. Topical formulations offer localized relief with fewer systemic effects.
Prescription Medications
In more severe cases, healthcare providers may prescribe stronger anti-inflammatory medications or short courses of corticosteroids to manage acute flare-ups.
Corticosteroid Injections
Injections directly into the joint can provide temporary relief by reducing inflammation. However, their use is typically limited to avoid potential damage to joint structures with repeated administration.
Alternative and Complementary Therapies
Acupuncture and Acupressure
These therapies may help alleviate pain by stimulating specific points in the body, potentially improving circulation and reducing inflammation.
Ultrasound and Shockwave Therapy
These modalities are designed to promote tissue healing and reduce inflammation. They are often available in specialized physical therapy or sports medicine settings.
Nutritional Supplements
Compounds such as glucosamine and chondroitin may provide modest symptom relief in some individuals. Omega-3 fatty acids, commonly found in fish oil, also possess anti-inflammatory properties. Consultation with a healthcare provider is recommended before initiating any supplement regimen.
Surgical Options
Cheilectomy
This procedure involves removing bone spurs and a portion of the joint surface. It is typically recommended in early-stage arthritis to improve joint movement and reduce pain.
Arthrodesis
Joint fusion eliminates movement at the affected joint, thereby relieving pain. Although it results in loss of flexibility, it often allows for a stable and functional gait.
Joint Replacement
Arthroplasty involves replacing the damaged joint surfaces with artificial components. This approach preserves some degree of motion, although long-term outcomes may vary.
When to Seek Medical Attention
Consultation with a specialist, such as a podiatrist or orthopedic surgeon, is recommended when symptoms persist or worsen.
Persistent Pain
Ongoing pain that interferes with daily activities indicates the need for professional evaluation.
Unresolved Swelling
Swelling that does not improve with conservative measures may suggest disease progression.
Impaired Mobility
Difficulty walking short distances or performing routine tasks warrants further assessment.
Neurological Symptoms
Numbness or tingling may indicate nerve involvement and should be evaluated promptly.
Conclusion
The management of arthritis in the big toe requires a comprehensive and individualized approach. Conservative strategies, including lifestyle modification, appropriate footwear, targeted exercises, and pharmacological interventions, form the foundation of treatment.
Moreover, early intervention is critical in slowing disease progression and preserving joint function. When necessary, surgical options provide effective solutions for advanced cases. By combining informed decision-making with professional guidance, individuals can effectively manage symptoms and maintain an active and functional lifestyle.