Bacterial Vaginosis (BV) is one of the most common vaginal conditions affecting women of reproductive age. It occurs when the natural balance of bacteria in the vagina becomes disrupted, allowing certain harmful bacteria to multiply excessively. Under normal circumstances, the vaginal microbiome is dominated by beneficial bacteria known as Lactobacillus, which help maintain an acidic environment that protects against infections. When this balance is disturbed, the vaginal environment becomes more favorable for harmful microorganisms, resulting in bacterial vaginosis.
- Multiple or new sexual partners increase risk by shifting vaginal bacterial composition and destabilizing the microbiome.
- Vaginal douching disrupts beneficial bacteria and alters pH, markedly increasing BV risk; avoid internal cleansing.
- Unprotected sex can raise vaginal pH via semen, reducing acidity and promoting harmful bacterial growth; consistent condom use is recommended.
- Smoking and scented hygiene products can impair immune defenses and alter vaginal pH, increasing susceptibility to BV.
- Prevent with gentle external hygiene, breathable clothing, healthy lifestyle, condom use, and seek medical evaluation for persistent symptoms or odor.
Although BV is not always classified strictly as a sexually transmitted infection, it is closely associated with sexual activity and several behavioral, biological, and lifestyle factors. Understanding the underlying risk factors and adopting effective preventive measures can significantly reduce the likelihood of developing this condition.
Understanding the Vaginal Microbiome

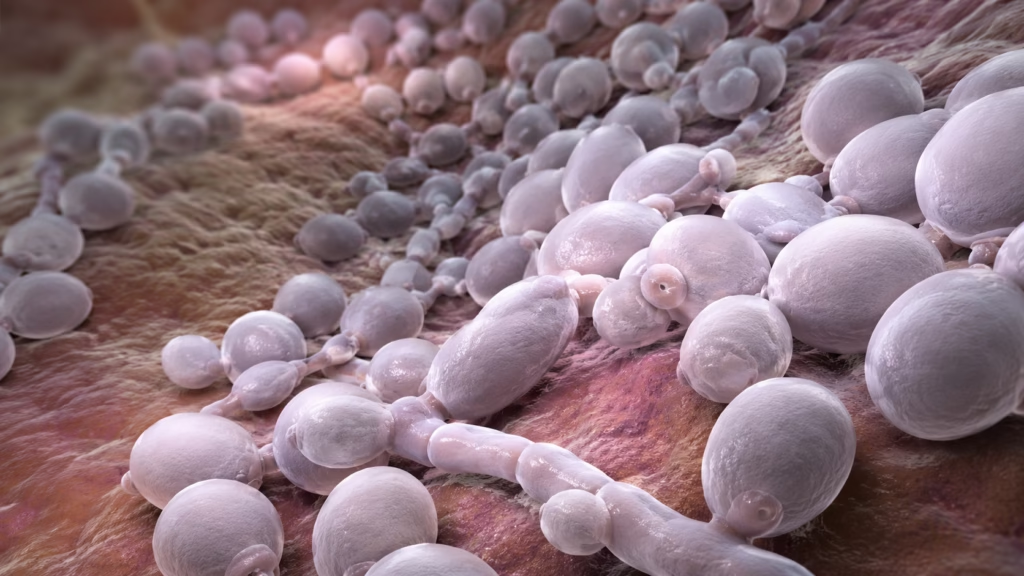
The vagina contains a complex ecosystem of microorganisms collectively known as the vaginal microbiota. Healthy vaginal flora is primarily composed of Lactobacillus species that produce lactic acid and hydrogen peroxide. These substances help maintain a low pH environment, typically between 3.8 and 4.5, which inhibits the growth of pathogenic organisms.
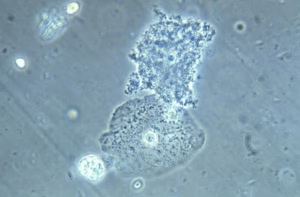
Bacterial vaginosis develops when the protective lactobacilli decrease and are replaced by anaerobic bacteria such as Gardnerella vaginalis, Atopobium vaginae, and Mobiluncus species. This microbial imbalance alters the vaginal pH and produces characteristic symptoms such as unusual discharge and odor.
However, BV can also occur without noticeable symptoms, which makes awareness of risk factors particularly important.
Common Risk Factors for Bacterial Vaginosis
Several factors can disrupt the natural vaginal microbiome and increase susceptibility to bacterial vaginosis. These risk factors often involve lifestyle behaviors, hormonal changes, or alterations in vaginal hygiene practices.
Multiple or New Sexual Partners
Women who have multiple sexual partners or a new partner may experience shifts in vaginal bacterial composition. Exposure to different bacterial environments can interfere with the stability of the vaginal microbiota, increasing the risk of BV.
Although BV is not strictly classified as a sexually transmitted infection, sexual activity remains one of the strongest associations identified in clinical studies.
Unprotected Sexual Activity
Unprotected intercourse may contribute to microbial imbalance within the vaginal environment. Semen has an alkaline pH, which can temporarily raise the vaginal pH and reduce the protective acidic environment maintained by beneficial bacteria.
Repeated exposure to alkaline conditions can make it easier for harmful bacteria to proliferate.
Vaginal Douching
Douching is widely recognized as one of the most significant behavioral risk factors for bacterial vaginosis. This practice involves flushing the vagina with water or cleansing solutions in an attempt to improve hygiene.
However, the vagina is naturally self-cleaning. Douching disrupts the microbial ecosystem by removing beneficial bacteria and altering the vaginal pH, which creates favorable conditions for pathogenic organisms.
Smoking
Research has identified smoking as a contributing factor in the development of bacterial vaginosis. Tobacco use can influence immune responses and may reduce the presence of beneficial lactobacilli in the vaginal microbiota.
Furthermore, certain compounds in cigarette smoke can impair the body’s natural defense mechanisms, making infections more likely.
Hormonal Changes
Hormonal fluctuations associated with menstruation, pregnancy, or hormonal contraceptives may influence the balance of vaginal bacteria. Changes in estrogen levels affect glycogen production in vaginal cells, which in turn influences bacterial growth patterns.
Periods of hormonal transition can therefore increase susceptibility to microbial imbalance.
Use of Certain Hygiene Products
Scented soaps, vaginal deodorants, and perfumed hygiene products may irritate the vaginal lining and disrupt the natural bacterial environment. Chemicals present in these products can alter pH levels and reduce the protective barrier created by beneficial bacteria.
Symptoms Associated with Bacterial Vaginosis
Although some individuals experience no noticeable symptoms, bacterial vaginosis can present with several characteristic signs, including:
-
Thin gray or white vaginal discharge
-
A strong fish-like odor, particularly after sexual intercourse
-
Vaginal irritation or itching
-
Burning sensation during urination
Symptoms may vary in intensity, and in some cases the condition is detected only during routine medical examinations.
Prevention Strategies for Bacterial Vaginosis
Preventing bacterial vaginosis primarily involves maintaining a healthy vaginal microbiome and avoiding practices that disrupt the natural bacterial balance. The following strategies are widely recommended in clinical and public health guidelines.
Avoid Vaginal Douching
One of the most effective preventive measures is to avoid douching entirely. Since the vagina naturally regulates its microbial environment, external cleansing products are unnecessary and often harmful.
Maintaining normal hygiene practices without internal cleansing helps preserve the beneficial bacterial population.
Practice Safe Sexual Habits
Consistent use of barrier protection such as condoms can reduce exposure to external bacteria and minimize changes in vaginal pH associated with semen. Limiting the number of sexual partners may also reduce the risk of microbial imbalance.
Open communication with partners and awareness of sexual health are essential components of prevention.
Choose Gentle Hygiene Products
Using mild, unscented soaps for external cleansing can help avoid irritation and disruption of the vaginal environment. Products containing perfumes, dyes, or harsh chemicals should be avoided in the genital area.
Maintaining simple hygiene routines often supports the natural balance of vaginal bacteria.
Maintain a Healthy Lifestyle
General health habits such as balanced nutrition, adequate sleep, and smoking cessation support immune function and microbial stability. The immune system plays a significant role in regulating bacterial populations within the body, including those in the vaginal microbiome.
Lifestyle choices therefore contribute indirectly to reducing infection risk.
Wear Breathable Clothing
Tight or non-breathable clothing may create warm and moist environments that encourage bacterial growth. Wearing cotton underwear and avoiding prolonged moisture exposure can help maintain a healthier genital environment.
When to Seek Medical Advice
Although bacterial vaginosis is often mild, untreated BV can lead to complications in certain situations. These may include increased susceptibility to sexually transmitted infections, complications during pregnancy, or pelvic inflammatory disease.
Individuals who experience persistent symptoms such as unusual discharge, strong odor, or irritation should seek evaluation from a qualified healthcare professional. Early diagnosis allows appropriate treatment, usually with prescribed antibiotics.
Conclusion
Bacterial vaginosis is a common condition that arises from disruption of the natural vaginal microbiome. While the condition may not always produce severe symptoms, understanding its risk factors is essential for maintaining reproductive health. Behavioral practices such as douching, smoking, and unprotected sexual activity can significantly increase vulnerability to microbial imbalance.
Preventive strategies emphasize maintaining the natural protective environment of the vagina through gentle hygiene practices, healthy lifestyle choices, and responsible sexual behavior. By prioritizing awareness and prevention, individuals can reduce the likelihood of bacterial vaginosis and support long-term vaginal health.