Introduction
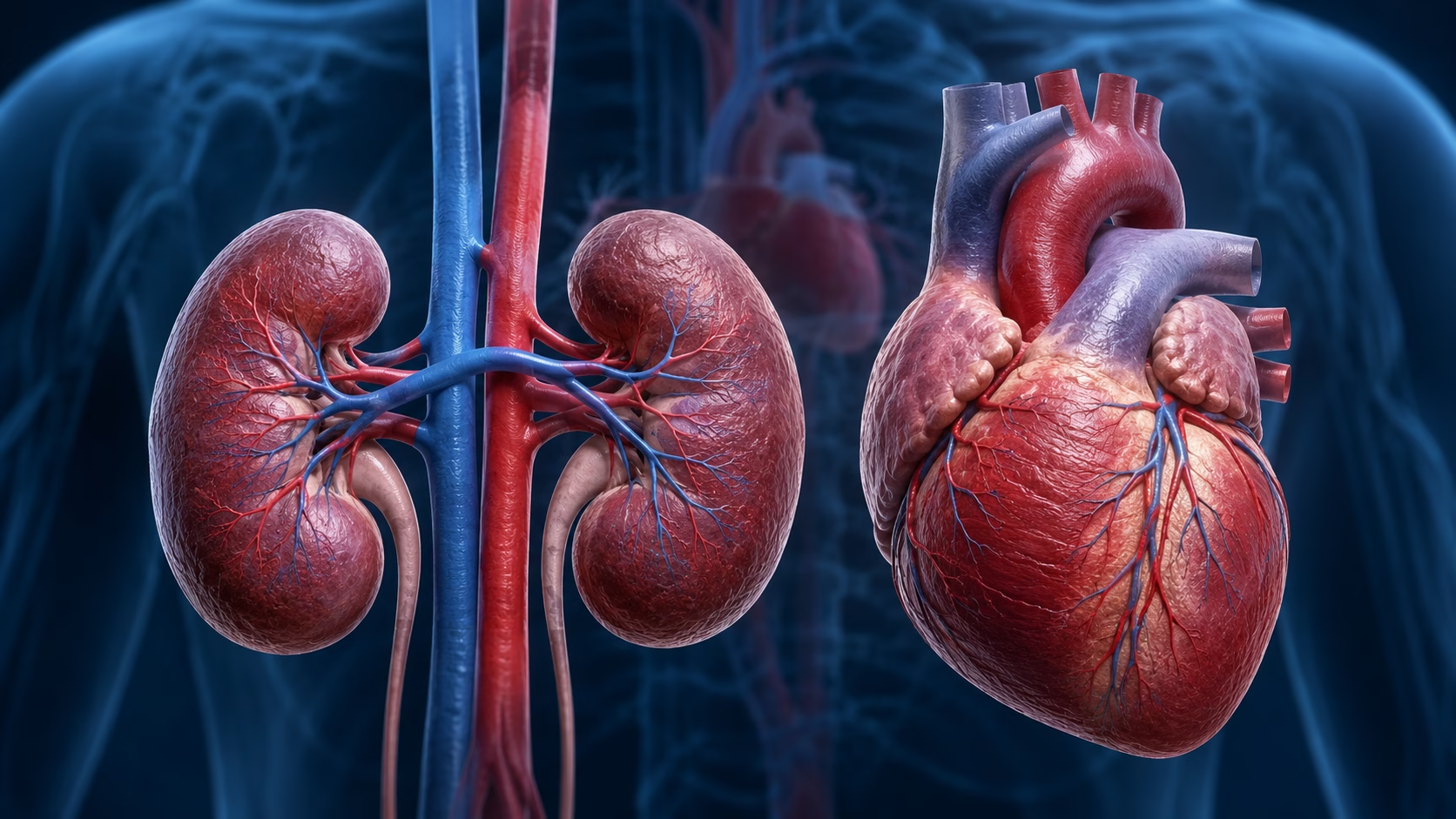
Renal failure and congestive heart failure are two major chronic conditions that frequently coexist and significantly influence one another. Together, they create a complex clinical relationship in which dysfunction in one organ system contributes to deterioration in the other. This interaction, commonly referred to as the cardiorenal connection or cardiorenal syndrome, represents a major challenge in modern healthcare because it increases complications, hospitalizations, and mortality rates.
- Acute and chronic renal failure impair filtration, cause electrolyte imbalance, fluid retention, and increase cardiovascular risk.
- Left and right heart failure produce pulmonary congestion or peripheral edema, causing dyspnea, fatigue, and exercise intolerance.
- Cardiorenal syndrome is bidirectional: reduced cardiac output worsens renal perfusion; renal dysfunction promotes fluid overload, further straining the heart.
- Diagnosis uses blood tests, biomarkers, echocardiography, renal ultrasound, urinalysis, chest radiographs, and blood pressure monitoring.
- Management combines medications, device therapies, dialysis when needed, lifestyle modification, multidisciplinary care, and careful fluid and electrolyte monitoring.
The heart and kidneys are closely interconnected through circulatory, hormonal, and fluid regulation mechanisms. When either organ loses functional efficiency, the resulting physiological imbalance places additional stress on the other. Understanding this relationship is essential for effective prevention, diagnosis, and treatment.
Understanding Renal Failure
Renal failure refers to the inability of the kidneys to adequately filter waste products, regulate electrolytes, and maintain fluid balance. The condition may develop suddenly or progress gradually over time depending on the underlying cause.
Acute kidney injury is characterized by a rapid decline in kidney function occurring over hours or days. This condition may result from severe dehydration, infections, reduced blood flow to the kidneys, or exposure to medications that damage kidney tissue. Because the onset is abrupt, prompt diagnosis and treatment are essential to prevent permanent injury.
Chronic kidney disease develops gradually over months or years and involves progressive loss of kidney function. The condition is classified into stages based on the glomerular filtration rate, which measures the kidneys’ ability to filter blood. Diabetes mellitus and hypertension are among the most common causes because they damage the delicate blood vessels within the kidneys over time. Inflammatory diseases affecting kidney structures may also contribute to chronic dysfunction.
As kidney function declines, several physiological disturbances occur. Sodium and fluid retention lead to swelling in the extremities and increased circulatory volume. Electrolyte imbalances, particularly elevated potassium levels, can interfere with cardiac rhythm and muscle function. Accumulation of metabolic waste products contributes to symptoms such as fatigue, nausea, loss of appetite, and confusion. Furthermore, renal failure substantially increases cardiovascular risk because impaired kidney function affects blood pressure regulation and vascular health.
Understanding Congestive Heart Failure
Congestive heart failure occurs when the heart is unable to pump blood effectively enough to meet the body’s demands. This impaired pumping capacity results in fluid accumulation within tissues and organs.
Left sided heart failure primarily affects the lungs because blood backs up into the pulmonary circulation. Individuals commonly experience shortness of breath, chronic coughing, and difficulty breathing while lying down. Reduced oxygen delivery may also contribute to fatigue and exercise intolerance.
Right sided heart failure mainly affects systemic circulation. Fluid accumulates in the legs, ankles, and abdomen, leading to swelling and weight gain. In advanced cases, congestion may affect liver function and digestive processes.
Several conditions increase the risk of developing heart failure. Coronary artery disease restricts blood supply to heart tissue, weakening cardiac function. Chronic hypertension forces the heart to work harder over time, eventually leading to structural and functional changes. Heart valve disorders interfere with efficient blood flow, while diabetes and obesity contribute to both vascular and metabolic stress.
The symptoms of congestive heart failure often include shortness of breath, persistent coughing, swelling of the lower limbs, fatigue, and irregular heart rhythms. These symptoms may worsen gradually and significantly reduce quality of life if not properly managed.
The Cardiorenal Connection
The relationship between renal failure and congestive heart failure is bidirectional. Dysfunction in one organ can directly impair the function of the other, creating a cycle of progressive deterioration known as cardiorenal syndrome.
When the heart fails to pump effectively, blood flow to the kidneys decreases. Reduced renal perfusion limits the kidneys’ ability to filter waste and regulate fluids, resulting in worsening kidney function. In response, the kidneys activate hormonal systems designed to retain sodium and water in an attempt to restore blood pressure and circulation. However, this fluid retention increases the workload on the heart and further exacerbates heart failure.
Conversely, kidney failure contributes to fluid overload and elevated blood pressure, both of which place additional strain on the heart. Electrolyte disturbances associated with renal dysfunction can also impair cardiac rhythm and contractility.
This interaction creates a self perpetuating cycle in which both organs progressively deteriorate unless carefully managed. The coexistence of these conditions is associated with increased hospital readmissions, higher treatment complexity, and elevated mortality risk.
Recognizing Warning Signs
Because renal failure and congestive heart failure share several overlapping symptoms, careful monitoring is essential. Rapid weight gain may indicate fluid retention, while worsening shortness of breath suggests increasing congestion in the lungs. Reduced urine output or dark urine may signal declining kidney function. Persistent fatigue, nausea, or confusion may result from inadequate circulation or accumulation of metabolic waste products.
Blood pressure that remains elevated despite medication may also indicate worsening cardiorenal dysfunction. Recognizing these signs early allows for timely medical intervention and reduces the risk of severe complications.
Diagnostic Approaches
Accurate diagnosis requires a combination of laboratory testing, imaging studies, and clinical evaluation.
Blood tests provide essential information regarding kidney and heart function. Elevated serum creatinine and blood urea nitrogen levels indicate impaired kidney filtration, while abnormalities in sodium and potassium levels reflect electrolyte disturbances. Biomarkers such as B type natriuretic peptide help assess the severity of heart failure by indicating cardiac stress.
Imaging studies contribute to structural and functional evaluation. Echocardiography assesses heart pumping efficiency and identifies abnormalities in cardiac structure. Renal ultrasound helps detect structural changes in the kidneys, including obstruction or chronic damage.
Additional assessments such as urinalysis may reveal protein or blood in the urine, suggesting kidney injury. Chest radiographs can identify pulmonary congestion associated with heart failure, while blood pressure monitoring provides information about circulatory stability.
Treatment Strategies
Management of cardiorenal syndrome requires a multidisciplinary approach involving cardiologists, nephrologists, dietitians, and primary care providers. The goal is to balance treatment of both organ systems while minimizing adverse effects.
Medications form the foundation of treatment. ACE inhibitors and angiotensin receptor blockers help protect both heart and kidney function by reducing blood pressure and limiting harmful hormonal activation. Beta blockers reduce cardiac workload and improve heart efficiency. Diuretics are commonly used to remove excess fluid, although careful monitoring is required because excessive fluid removal may worsen kidney function. Mineralocorticoid receptor antagonists may also help control fluid retention and reduce cardiovascular stress.
In some individuals, device based therapies are necessary. Implantable cardioverter defibrillators reduce the risk of sudden cardiac death, while cardiac resynchronization therapy improves coordination of heart contractions.
Advanced chronic kidney disease may require renal replacement therapy such as hemodialysis or peritoneal dialysis. In selected cases, evaluation for kidney transplantation may be appropriate.
Regular monitoring of body weight, electrolyte levels, kidney function, and blood pressure is essential to ensure that treatment remains effective and balanced. Medication adjustments are often necessary because interventions that benefit one organ may negatively affect the other.
Lifestyle Modifications and Prevention
Lifestyle changes play a critical role in slowing disease progression and improving overall health outcomes.
Dietary management is particularly important. Restricting sodium intake helps reduce fluid retention and blood pressure. Protein intake may need to be moderated in advanced kidney disease to reduce metabolic burden. A diet emphasizing fruits, vegetables, and whole grains supports cardiovascular and metabolic health.
Regular physical activity improves circulation, strengthens the cardiovascular system, and enhances functional capacity. Low impact activities such as walking, swimming, and cycling are generally recommended because they provide cardiovascular benefits while minimizing strain.
Smoking cessation and moderation of alcohol intake reduce vascular damage and improve long term outcomes. Maintaining a healthy body weight decreases stress on both the heart and kidneys. Stress management techniques such as meditation and yoga may further support cardiovascular stability and emotional well being.
Routine medical evaluations and laboratory monitoring remain essential for early detection of disease progression and timely intervention.
Prognosis and Support Systems
The prognosis of individuals with combined renal failure and congestive heart failure depends on the severity of organ dysfunction, the effectiveness of treatment, and adherence to management strategies. Early diagnosis and coordinated care significantly improve outcomes and quality of life.
Support systems also play a vital role in long term management. Family members, patient support groups, and counseling services help individuals cope with the emotional and practical challenges associated with chronic illness. Access to education and community resources further enhances self management and treatment adherence.
Conclusion
Renal failure and congestive heart failure are deeply interconnected conditions that frequently coexist and reinforce one another through complex physiological mechanisms. This cardiorenal relationship complicates treatment and increases the risk of serious complications.
Understanding the interaction between the heart and kidneys allows for earlier recognition of symptoms, more effective treatment strategies, and improved long term outcomes. Through a combination of medical management, lifestyle modification, and multidisciplinary care, individuals living with these conditions can better manage symptoms and slow disease progression.
Prompt medical evaluation, adherence to treatment plans, and ongoing collaboration with healthcare professionals remain essential for protecting both heart and kidney health.