What Is the Difference Between Atrial Fibrillation (AFib) and Congestive Heart Failure?
Introduction
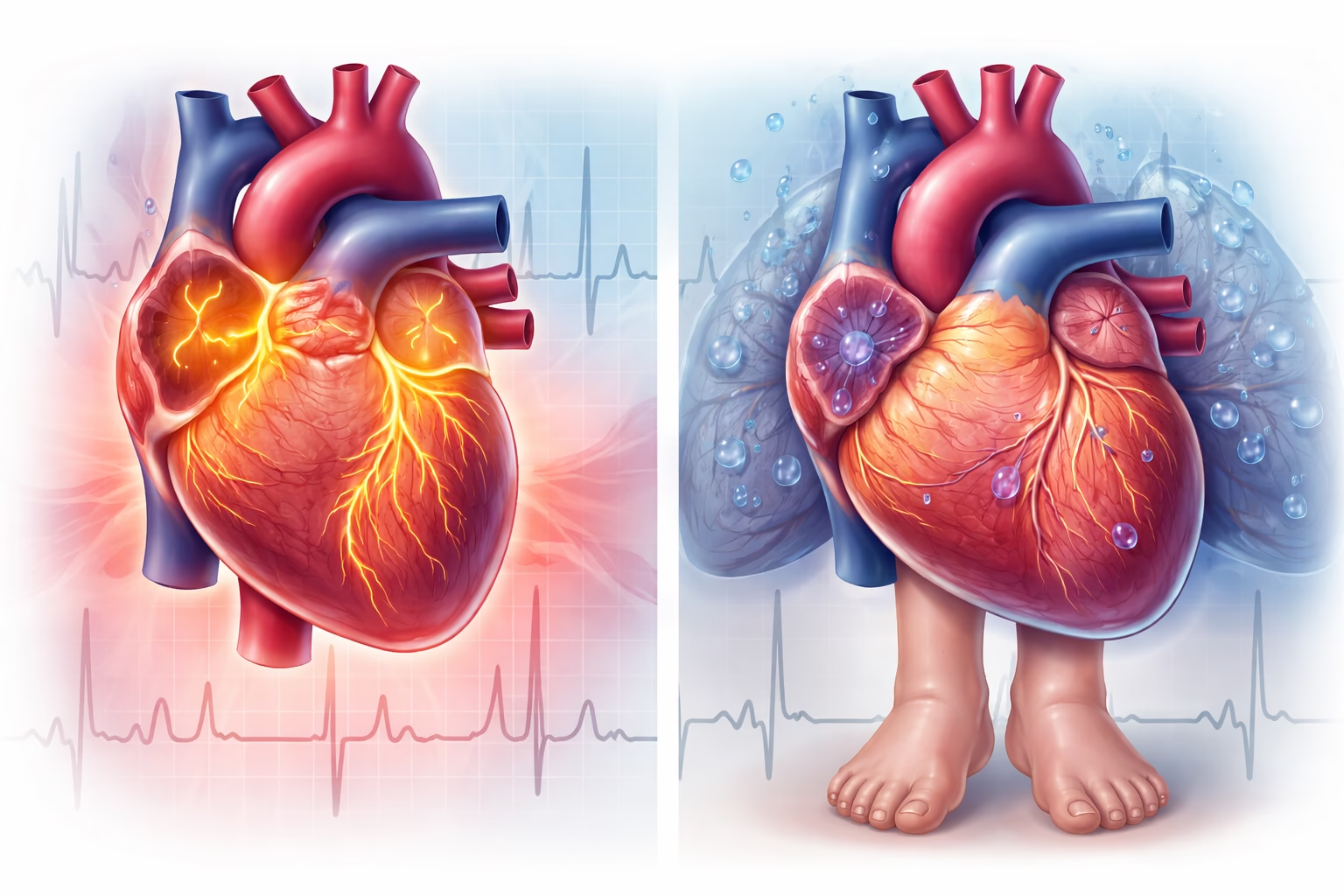
Cardiovascular diseases remain a leading cause of morbidity and mortality globally. Among the most frequently encountered conditions are atrial fibrillation (AFib) and congestive heart failure (CHF). Although both disorders impair the heart’s efficiency, they arise from distinct pathophysiological mechanisms and present with different clinical profiles. A clear understanding of these differences is essential for early detection, accurate diagnosis, and appropriate management.
This article provides a detailed and structured explanation of AFib and CHF, expanding on their causes, symptoms, complications, and management strategies.
Understanding Atrial Fibrillation (AFib)
What Is AFib?
Atrial fibrillation is a form of cardiac arrhythmia characterized by irregular and often rapid electrical activity in the atria, which are the upper chambers of the heart. Under normal physiological conditions, electrical impulses originate from the sinoatrial node and propagate in an orderly fashion, resulting in coordinated contraction.
However, in AFib, this orderly conduction is disrupted. Instead of contracting effectively, the atria quiver or fibrillate. Consequently, blood is not efficiently transferred into the ventricles, leading to impaired cardiac output and potential blood stagnation within the atrial chambers.
Causes and Risk Factors
Hypertension
Chronic high blood pressure increases the workload of the heart. Over time, this leads to structural remodeling of the atria, including enlargement and fibrosis, which predispose individuals to abnormal electrical signaling.
Coronary Artery Disease
Reduced blood supply to heart tissue due to narrowed arteries can damage cardiac cells. This damage may interfere with normal electrical conduction pathways, increasing the likelihood of arrhythmias.
Valve Disorders
Abnormalities in heart valves, such as stenosis or regurgitation, alter blood flow dynamics. These changes can enlarge the atria and create conditions favorable for AFib development.
Thyroid Disorders
Excess thyroid hormone, particularly in hyperthyroidism, accelerates metabolic activity and heart rate. This heightened stimulation can trigger irregular heart rhythms.
Alcohol and Caffeine
Excessive intake of stimulants, especially alcohol, is associated with episodes of AFib. This phenomenon is sometimes referred to as “holiday heart syndrome.”
Age and Genetics
The prevalence of AFib increases significantly with age. Moreover, genetic predisposition can influence susceptibility, particularly in individuals with a family history of arrhythmias.
Common Symptoms
Palpitations
Patients often report a sensation of fluttering or pounding in the chest. This reflects the irregular electrical activity of the atria.
Dizziness and Lightheadedness
Irregular cardiac output may reduce cerebral perfusion, leading to transient dizziness.
Shortness of Breath
Inadequate cardiac efficiency during exertion results in reduced oxygen delivery to tissues, causing breathlessness.
Fatigue
Chronic inefficiency of blood circulation leads to reduced energy levels and persistent tiredness.
Chest Discomfort
Although less common, some individuals may experience mild chest pain or discomfort due to irregular cardiac activity.
Potential Complications
Stroke
One of the most serious complications of AFib arises from blood clot formation within the atria. These clots can travel to the brain, resulting in ischemic stroke.
Heart Failure
Persistent AFib can weaken the heart over time, eventually contributing to heart failure.
Reduced Quality of Life
Chronic symptoms such as fatigue and palpitations can significantly impair daily functioning and overall well-being.
Understanding Congestive Heart Failure (CHF)
What Is Congestive Heart Failure?
Congestive heart failure is a chronic condition in which the heart is unable to pump sufficient blood to meet the body’s metabolic demands. Unlike AFib, which is primarily an electrical disorder, CHF is a mechanical problem involving weakened or stiffened heart muscle.
The term “congestive” refers to the accumulation of fluid in various parts of the body, including the lungs, lower limbs, and abdominal cavity, due to impaired circulation.
Causes and Risk Factors
Coronary Artery Disease
Reduced blood flow to the heart muscle weakens its contractile function over time.
Long-Standing Hypertension
Sustained high blood pressure forces the heart to pump against increased resistance, eventually leading to muscle thickening and weakening.
Previous Heart Attack
Damage from myocardial infarction results in scar tissue, which cannot contract effectively.
Cardiomyopathy
Diseases of the heart muscle, whether genetic or acquired, directly impair pumping ability.
Diabetes
Chronic hyperglycemia contributes to vascular damage and metabolic dysfunction, increasing the risk of heart failure.
Obesity and Sedentary Lifestyle
Excess body weight and physical inactivity place additional strain on the cardiovascular system, promoting disease progression.
Common Symptoms
Persistent Coughing or Wheezing
Fluid accumulation in the lungs interferes with normal respiratory function, particularly when lying down.
Shortness of Breath
Dyspnea may occur both during physical activity and at rest, reflecting impaired oxygen exchange.
Edema
Swelling in the feet, ankles, legs, or abdomen results from fluid retention due to poor circulation.
Irregular Heartbeat
The heart may attempt to compensate for reduced efficiency by increasing its rate or becoming irregular.
Reduced Exercise Tolerance
Patients often find it difficult to perform routine physical activities due to fatigue and breathlessness.
Nocturia
Increased urination at night occurs as fluid redistributes when lying down.
Potential Complications
Kidney Damage
Reduced blood flow to the kidneys impairs their ability to filter waste effectively.
Liver Congestion
Fluid buildup can affect liver function, leading to congestion and potential damage.
Arrhythmias
CHF increases the risk of abnormal heart rhythms, including AFib.
Sudden Cardiac Death
In severe cases, electrical instability may lead to life-threatening arrhythmias.
Key Differences Between AFib and CHF
Underlying Mechanism
AFib is fundamentally an electrical disorder affecting the rhythm of the heart, whereas CHF is a mechanical disorder involving the heart’s inability to pump effectively.
Symptom Profile
AFib primarily presents with palpitations, dizziness, and irregular pulse. In contrast, CHF is characterized by fluid retention, shortness of breath, and persistent coughing.
Diagnostic Evaluation
AFib is diagnosed through electrical monitoring techniques such as electrocardiograms and ambulatory monitors. Conversely, CHF is evaluated using imaging modalities like echocardiography and laboratory tests assessing cardiac biomarkers.
Treatment Approaches
Management of AFib focuses on controlling heart rate and rhythm, as well as preventing clot formation through anticoagulation. In contrast, CHF treatment emphasizes improving cardiac function, reducing fluid overload, and slowing disease progression through medications and lifestyle changes.
Prognosis
AFib can often be effectively managed over the long term with appropriate therapy. However, CHF is generally progressive, requiring continuous monitoring and adjustment of treatment strategies.
When AFib and CHF Coexist
Pathophysiological Interaction
AFib and CHF frequently coexist, creating a complex clinical scenario. AFib reduces the efficiency of atrial contraction, thereby decreasing cardiac output and exacerbating heart failure symptoms. Conversely, fluid overload and structural changes in CHF can stretch cardiac tissue, increasing susceptibility to arrhythmias.
Management Strategies
Effective management requires an integrated approach. Rate and rhythm control in AFib are essential to maintain adequate cardiac output. Simultaneously, fluid management through diuretics is critical in CHF to reduce congestion. Coordination between cardiology specialists is often necessary to optimize patient outcomes.
Prevention and Lifestyle Strategies
Heart-Healthy Diet
A balanced diet rich in fruits, vegetables, whole grains, and lean proteins supports cardiovascular health. Limiting sodium intake is particularly important to control blood pressure and prevent fluid retention.
Regular Physical Activity
Engaging in consistent moderate exercise improves cardiac efficiency, enhances circulation, and supports overall health.
Weight Management
Maintaining a healthy body weight reduces strain on the heart and lowers the risk of both AFib and CHF.
Blood Pressure and Cholesterol Control
Regular monitoring and adherence to prescribed medications help prevent vascular damage and disease progression.
Avoiding Tobacco and Excess Alcohol
Smoking cessation and moderation of alcohol intake significantly reduce cardiovascular risk.
Regular Medical Checkups
Routine health evaluations enable early detection of abnormalities, allowing for timely intervention and improved outcomes.
Conclusion
Atrial fibrillation and congestive heart failure represent two distinct yet interconnected cardiovascular conditions. AFib arises from disordered electrical activity in the atria, whereas CHF reflects a progressive decline in the heart’s pumping capacity. Despite these differences, both conditions can coexist and mutually exacerbate each other.
Therefore, early recognition, accurate diagnosis, and comprehensive management remain essential. Adopting preventive lifestyle measures, adhering to medical therapy, and maintaining regular follow-up with healthcare professionals are critical strategies for improving long-term outcomes and quality of life.