Introduction
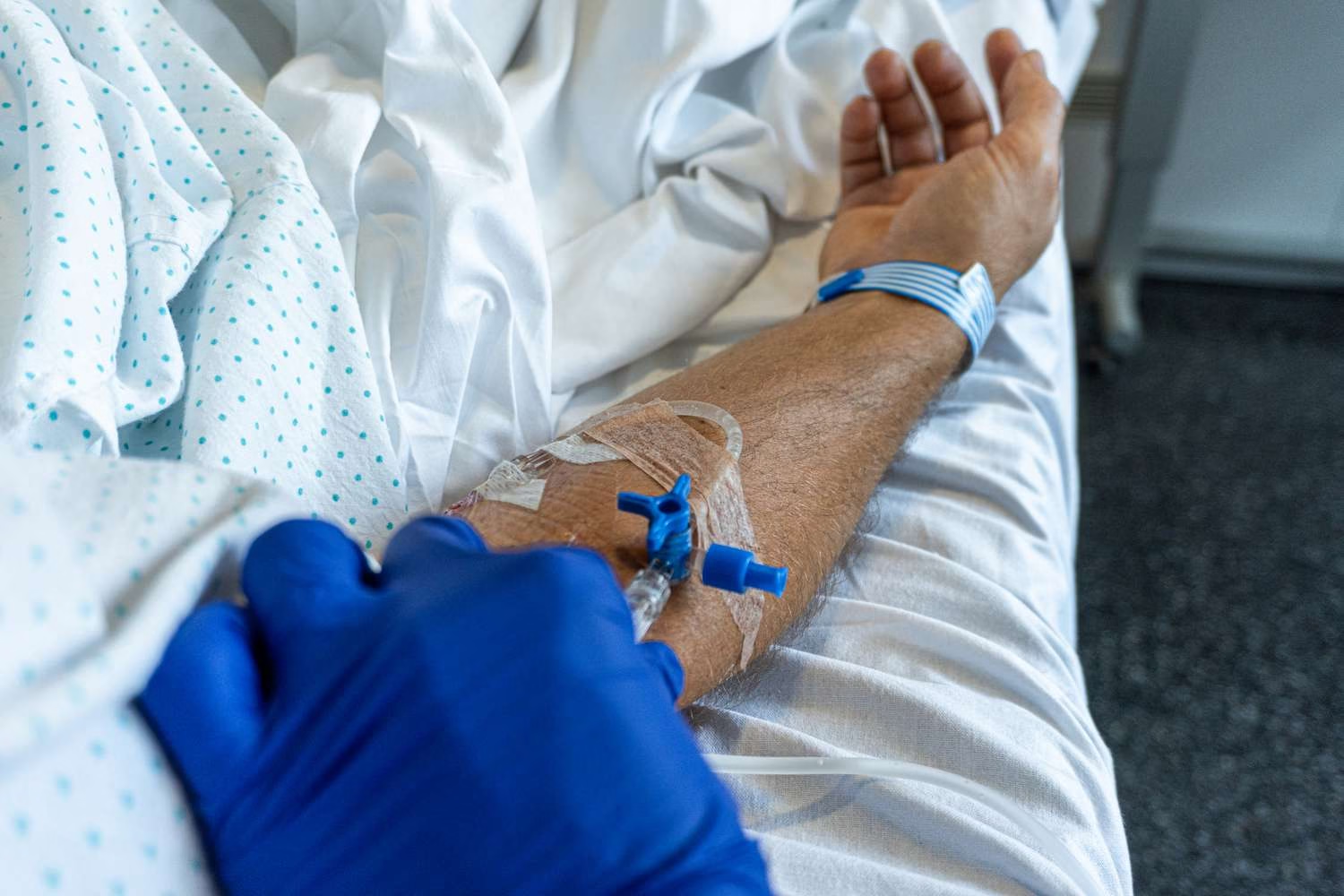
Dehydration is a physiological state in which fluid loss exceeds intake, leading to impaired cellular and organ function. While mild dehydration can often be corrected with oral fluids, more severe cases require rapid and controlled intervention. Intravenous (IV) fluid therapy represents a cornerstone of modern clinical practice, enabling direct delivery of fluids and electrolytes into the bloodstream.
This article provides a detailed and structured explanation of dehydration, the role of IV fluids, their mechanisms of action, and their clinical applications.
Understanding Dehydration
Causes of Dehydration
Excessive Fluid Loss
Significant fluid loss may occur through sweating during intense physical activity or fever. This loss is often accompanied by electrolyte depletion, which can disrupt physiological balance.
Gastrointestinal Losses
Vomiting and diarrhea are among the most common causes of acute dehydration. These conditions lead to rapid depletion of both fluids and essential electrolytes.
Inadequate Fluid Intake
Failure to consume sufficient fluids, particularly in hot climates or during illness, contributes to dehydration.
Medication Effects
Certain medications, including diuretics and laxatives, increase fluid excretion and may predispose individuals to dehydration.
Common Symptoms
Thirst and Dry Mouth
These are early indicators reflecting the body’s attempt to restore fluid balance.
Neurological Symptoms
Headache, dizziness, and lightheadedness occur as a result of reduced cerebral perfusion.
Fatigue and Muscle Cramps
Electrolyte imbalances impair muscle and nerve function, leading to weakness and cramping.
Urinary Changes
Dark-colored urine and reduced output indicate decreased kidney perfusion and fluid conservation.
Clinical Significance
Dehydration can progress to serious complications, including electrolyte disturbances, acute kidney injury, hypotension, and, in severe cases, hypovolemic shock. Therefore, timely recognition and intervention are essential.
Why Oral Rehydration May Be Insufficient
Oral rehydration is effective in mild to moderate dehydration. However, it may be inadequate under certain conditions.
Gastrointestinal Limitations
Persistent vomiting or severe diarrhea prevents adequate absorption of oral fluids.
Impaired Consciousness
Patients who are unable to swallow safely require alternative methods of hydration.
Need for Rapid Correction
In critical conditions such as heat stroke or severe volume depletion, immediate restoration of circulating volume is necessary.
In such scenarios, IV fluid therapy provides a direct and efficient means of rehydration.
What Are IV Fluids?
IV fluids are sterile solutions administered directly into the bloodstream through a venous catheter. They are formulated to restore fluid balance, correct electrolyte disturbances, and, in some cases, provide metabolic support.
Major Categories of IV Fluids
Crystalloids
Crystalloids contain small molecules that easily move across vascular membranes. They are widely used due to their effectiveness and accessibility.
Common examples include normal saline, lactated Ringer’s solution, and dextrose-containing solutions.
Colloids
Colloids contain larger molecules that remain within the vascular compartment for longer periods. They exert oncotic pressure, drawing fluid from surrounding tissues into the bloodstream.
Examples include albumin and synthetic starches.
Hypertonic Solutions
These solutions have a higher osmolarity than plasma and are used in specific clinical situations to shift fluid into the vascular compartment.
Mechanisms of Rehydration
IV fluids restore hydration through several physiological processes.
Intravascular Volume Expansion
Isotonic crystalloids rapidly increase plasma volume, improving blood pressure and tissue perfusion. This effect is particularly important in cases of hypovolemia and shock.
Osmotic Fluid Shifts
Hypotonic solutions facilitate movement of water into cells, correcting intracellular dehydration. Conversely, hypertonic solutions draw fluid from cells into the bloodstream, stabilizing circulation in critical states.
Electrolyte Restoration
IV fluids are formulated to replenish essential ions such as sodium, potassium, and calcium. These electrolytes are crucial for maintaining nerve conduction, muscle contraction, and cardiac function.
Common IV Solutions and Their Clinical Uses
Normal Saline (0.9% Sodium Chloride)
This isotonic solution is widely used for general fluid replacement. It is particularly effective in treating hypovolemia, shock, and dehydration.
Lactated Ringer’s Solution
This balanced solution contains multiple electrolytes and is commonly used in surgical settings, trauma care, and burn management.
Dextrose 5% in Water (D5W)
D5W provides free water and a small amount of energy. It is often used in cases where hydration is required without significant electrolyte disturbance.
Half-Normal Saline (0.45% Sodium Chloride)
This hypotonic solution is used to address intracellular dehydration, particularly in conditions involving cellular fluid deficits.
Hypertonic Saline (3%–5%)
Hypertonic saline is reserved for severe cases such as cerebral edema or profound hyponatremia and requires careful monitoring.
Colloids
Colloid solutions, such as albumin, are used in cases of significant plasma loss or low oncotic pressure. They help maintain intravascular volume more effectively than crystalloids in certain clinical scenarios.
The IV Fluid Administration Process
Clinical Assessment
Before initiating IV therapy, healthcare providers evaluate vital signs, body weight, and laboratory parameters, including electrolyte levels and kidney function.
Establishing IV Access
A catheter is inserted into a peripheral vein for short-term therapy or a central vein for long-term or high-volume administration.
Controlled Infusion
Fluids are delivered using infusion pumps that regulate flow rates precisely. Continuous monitoring ensures appropriate response and prevents complications.
Monitoring and Adjustment
Regular assessment of clinical status and laboratory values guides adjustments in fluid type and rate.
Transition to Oral Intake
Once the patient stabilizes, IV fluids are gradually discontinued, and oral hydration is resumed.
Safety Considerations and Potential Complications
Although IV fluid therapy is generally safe, certain risks must be carefully managed.
Fluid Overload
Excessive fluid administration can lead to edema and respiratory complications, particularly in patients with heart or kidney disease.
Electrolyte Imbalances
Incorrect fluid selection or dosing may result in abnormal electrolyte levels, affecting cardiac and neurological function.
Local Complications
Inflammation of the vein, known as phlebitis, may occur at the insertion site.
Infection Risk
Improper handling or prolonged catheter use increases the risk of infection.
Air Embolism
Although rare, the introduction of air into the bloodstream can have serious consequences and requires strict procedural control.
Conclusion
IV fluid therapy is an essential intervention for managing moderate to severe dehydration. By delivering fluids and electrolytes directly into the bloodstream, it enables rapid restoration of physiological balance and supports critical bodily functions.
Moreover, the selection of appropriate fluid types and careful monitoring are central to achieving optimal outcomes. When administered correctly, IV fluids not only correct dehydration but also prevent complications and facilitate recovery.