Shingles: Causes, Symptoms, Treatment, and Prevention
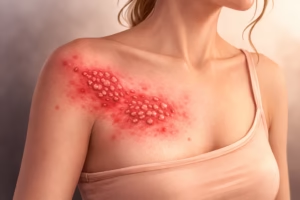
Shingles is a painful viral infection that affects millions of people worldwide each year. While many people associate it with a rash, shingles can be far more than a simple skin condition. It is linked to the same virus that causes chickenpox and can lead to significant discomfort, complications, and long-term nerve pain if not properly managed.
In this article, we’ll explore what shingles is, what causes it, how it presents, and the evidence-based strategies available for treatment and prevention.
Overview: What Is Shingles?
Shingles, medically known as herpes zoster, is a viral infection caused by the **varicella-zoster virus (VZV)**—the same virus responsible for chickenpox.
After a person recovers from chickenpox, the virus does not completely leave the body. Instead, it remains dormant (inactive) in nerve tissues near the spinal cord and brain. Years—or even decades—later, the virus can reactivate and cause shingles.
Key facts:
- Shingles typically presents as a painful rash on one side of the body or face.
- It most commonly affects older adults, particularly those over 50.
- It can occur in anyone who has previously had chickenpox.
- Early treatment reduces the risk of complications.
Causes and Risk Factors
The direct cause of shingles is the reactivation of latent varicella-zoster virus within nerve cells. However, several factors increase the likelihood of this reactivation.
Primary Risk Factors
- Age over 50 years (risk increases significantly with advancing age)
- Weakened immune system due to:
- HIV/AIDS
- Cancer
- Chemotherapy or radiation therapy
- Organ transplantation
- Long-term steroid use
- Chronic medical conditions
- Physical or emotional stress
- Recent illness or trauma
Even healthy individuals can develop shingles, although it is more common in those with reduced immune defenses.
Symptoms and Clinical Presentation
Shingles typically develops in distinct stages. Not everyone will experience all symptoms in the same way.
Early (Prodromal) Symptoms
Before the rash appears, individuals may experience:
- Burning, tingling, or itching in a localized area
- Sharp, stabbing, or shooting pain
- Sensitivity to touch
- Mild fever
- Headache
- Fatigue
This early pain is often mistaken for other conditions (such as heart, kidney, or dental problems), depending on its location.
Rash Development
Within a few days:
- A red rash appears in a localized area.
- The rash usually follows a dermatome—an area of skin supplied by a single nerve.
- Small fluid-filled blisters develop.
- Blisters eventually break open, crust over, and heal within 2–4 weeks.
The rash almost always affects one side of the body and does not cross the midline.
Complications
Some individuals may develop complications, including:
- Postherpetic neuralgia (PHN)
Persistent nerve pain lasting months or even years after the rash resolves. - Ophthalmic shingles (herpes zoster ophthalmicus)
Involvement of the eye, which can threaten vision. - Bacterial skin infections
- Neurological complications (rare)
Postherpetic neuralgia is the most common complication, particularly in older adults.
Diagnosis
Shingles is typically diagnosed based on:
- Characteristic rash appearance
- Distribution pattern along a dermatome
- Medical history of prior chickenpox
In unclear cases, laboratory tests may be used, including:
- Polymerase chain reaction (PCR) testing of blister fluid
- Direct fluorescent antibody testing
- Viral culture (less commonly used)
Prompt diagnosis is important, as antiviral treatment is most effective when started within 72 hours of rash onset.
Treatment and Management Options
While shingles usually resolves on its own, treatment aims to:
- Reduce the severity and duration of symptoms
- Decrease complications
- Prevent or reduce postherpetic neuralgia
Antiviral Medications
These are most effective when started early:
- Acyclovir
- Valacyclovir
- Famciclovir
Antivirals can shorten the disease course and reduce nerve damage.
Pain Management
Pain can range from mild to severe and may require:
- Over-the-counter pain relievers (e.g., acetaminophen, NSAIDs)
- Prescription medications
- Neuropathic pain agents (e.g., gabapentin)
- Topical treatments (e.g., lidocaine patches)
Supportive Care
- Cool compresses
- Loose clothing
- Keeping the rash clean and dry
Hospitalization is rarely required but may be necessary in severe cases or for individuals with significant immune suppression.
Prevention and Lifestyle Considerations
Vaccination
Vaccination is the most effective way to prevent shingles and its complications.
- The recombinant zoster vaccine (RZV) is recommended for:
- Adults aged 50 years and older
- Certain immunocompromised adults
Clinical trials show the vaccine significantly reduces:
- The risk of developing shingles
- The likelihood of postherpetic neuralgia
Even individuals who have previously had shingles can benefit from vaccination.
Reducing Risk
While shingles cannot always be prevented, maintaining a strong immune system may help:
- Eat a balanced, nutrient-rich diet
- Engage in regular physical activity
- Get adequate sleep
- Manage stress effectively
- Manage chronic health conditions appropriately
Is Shingles Contagious?
Shingles itself is not spread from person to person in the form of shingles. However:
- The virus can spread from active blisters to someone who has never had chickenpox or the vaccine
- In such cases, they may develop chickenpox, not shingles
Covering the rash and practicing good hygiene reduces transmission risk.
Conclusion
Shingles is a reactivation of the varicella-zoster virus that typically causes a painful, localized rash and can lead to long-term nerve pain if not treated promptly. Older adults and individuals with weakened immune systems are at highest risk. Early antiviral treatment and appropriate pain management significantly improve outcomes. Most importantly, vaccination provides strong protection against both shingles and its complications.
If you suspect you may have shingles or are experiencing unexplained localized pain and rash, seek evaluation from a qualified healthcare professional promptly.
Disclaimer:
This article is intended for educational purposes only and does not replace professional medical advice, diagnosis, or treatment. Always consult a qualified healthcare provider for guidance regarding your health or medical condition.