Ringworm: Causes, Symptoms, Treatment, and Prevention
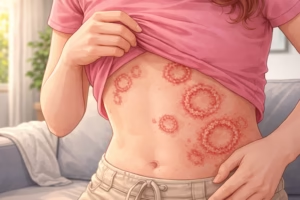
Ringworm is a common fungal infection that affects the skin, hair, or nails. Despite its name, it has nothing to do with worms. The term “ringworm” refers to the characteristic ring-shaped rash that often appears on the skin. Medically known as tinea or dermatophytosis, this infection is generally mild and treatable, but it can spread easily without proper care.
In this article, we’ll explore what ringworm is, what causes it, how it’s diagnosed and treated, and how you can reduce your risk.
Overview / Definition
Ringworm is a superficial fungal infection caused by a group of fungi called dermatophytes. These fungi thrive on keratin, a protein found in the skin, hair, and nails.
Depending on the area affected, ringworm is classified into different types:
- Tinea corporis – Body
- Tinea capitis – Scalp
- Tinea pedis – Athlete’s foot
- Tinea cruris – Jock itch
- Tinea unguium (onychomycosis) – Nails
- Tinea faciei – Face
Although it can affect anyone, ringworm is especially common in children, athletes, and people with weakened immune systems.
Causes and Risk Factors
What Causes Ringworm?
Ringworm is caused by dermatophyte fungi, most commonly from the genera:
- Trichophyton
- Microsporum
- Epidermophyton
These fungi spread through direct or indirect contact.
How It Spreads
You can get ringworm through:
- Skin-to-skin contact with an infected person
- Contact with infected animals (especially cats, dogs, and livestock)
- Contaminated objects (towels, clothing, combs, gym equipment)
- Soil (less common, but possible)
Risk Factors
Certain conditions increase susceptibility:
- Warm, humid environments
- Sweating excessively
- Wearing tight or non-breathable clothing
- Participation in contact sports (e.g., wrestling)
- Weakened immune system
- Diabetes
- Poor hygiene or crowded living conditions
Symptoms or Clinical Presentation
Symptoms vary depending on the area affected, but common signs include:
Skin (Tinea Corporis)
- Red, circular rash with raised borders
- Clear or scaly center
- Itching
- Gradually expanding ring-shaped lesion
Scalp (Tinea Capitis)
- Scaly patches
- Hair breakage or hair loss
- Black dots where hair has broken off
- Occasionally swollen lymph nodes
Feet (Tinea Pedis)
- Cracked or peeling skin between toes
- Burning or itching sensation
- Blisters in some cases
Nails (Tinea Unguium)
- Thickened nails
- Yellow or white discoloration
- Brittle, crumbly texture
Symptoms may start mildly and gradually worsen without treatment.
Diagnosis or Screening
Healthcare providers typically diagnose ringworm based on:
1. Clinical Examination
The rash’s characteristic appearance often allows for a clinical diagnosis.
2. Laboratory Testing (if needed)
If the presentation is atypical, a provider may perform:
- KOH (potassium hydroxide) preparation: A skin scraping is examined under a microscope.
- Fungal culture: Identifies the specific organism (takes longer).
- Wood’s lamp examination: Some fungal species fluoresce under ultraviolet light.
Accurate diagnosis is important because other conditions—such as eczema, psoriasis, or bacterial infections—can resemble ringworm.
Treatment or Management Options
Ringworm is generally treatable with antifungal medications.
Topical Antifungal Medications
Most mild skin infections respond to over-the-counter or prescription creams, such as:
- Clotrimazole
- Miconazole
- Terbinafine
- Ketoconazole
Treatment duration: Usually 2–4 weeks, even if symptoms improve earlier.
Oral Antifungal Medications
Oral medications may be necessary for:
- Scalp infections
- Nail infections
- Severe or widespread cases
- Infections that don’t respond to topical therapy
Common oral antifungals include:
- Terbinafine
- Griseofulvin
- Itraconazole
- Fluconazole
These medications require medical supervision due to possible side effects and drug interactions.
Important Treatment Tips
- Complete the full course of treatment.
- Keep affected areas clean and dry.
- Wash clothing, towels, and bedding regularly.
- Avoid sharing personal items.
Prevention and Lifestyle Considerations
Preventing ringworm involves simple hygiene and environmental measures:
Personal Hygiene
- Wash hands regularly.
- Shower after sports or sweating.
- Dry skin thoroughly, especially between toes.
Clothing and Footwear
- Wear breathable fabrics (e.g., cotton).
- Change socks daily.
- Avoid tight-fitting, damp clothing.
Public Spaces
- Wear sandals in locker rooms and communal showers.
- Use personal towels and grooming tools only.
Pet Care
- Check pets for hair loss or skin lesions.
- Seek veterinary care if infection is suspected.
Environmental Cleaning
- Disinfect shared surfaces.
- Wash linens in hot water if infected.
Consistent hygiene can significantly reduce recurrence.
Conclusion
Ringworm is a common and highly treatable fungal infection that affects the skin, scalp, or nails. Despite its name, it is not caused by a worm but by dermatophyte fungi that thrive in warm, moist conditions. Early recognition and appropriate antifungal treatment usually lead to full recovery.
Maintaining good hygiene, avoiding shared personal items, and keeping the skin clean and dry are key strategies for both treatment and prevention.
Disclaimer
This article is intended for educational purposes only and does not substitute for professional medical advice, diagnosis, or treatment. If you suspect you have ringworm or another skin condition, consult a qualified healthcare professional for proper evaluation and care.