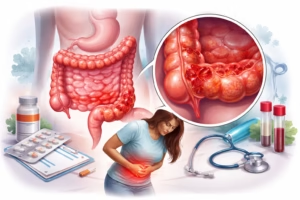
Inflammatory Bowel Disease (IBD): Understanding a Chronic Digestive Condition
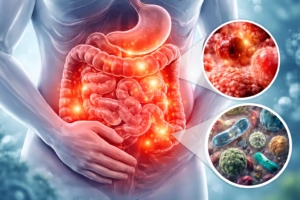
Inflammatory Bowel Disease (IBD) is a term used to describe chronic inflammatory conditions of the gastrointestinal (GI) tract. It primarily includes Crohn’s disease and ulcerative colitis, both of which can significantly impact a person’s quality of life if not properly managed. Although IBD is a lifelong condition, advances in medical research and treatment have made it increasingly manageable.
In this article, we’ll explore what IBD is, its causes, symptoms, diagnostic process, treatment options, and lifestyle considerations—all in clear, evidence-based language to help you better understand this complex condition.
Overview / Definition
Inflammatory Bowel Disease (IBD) refers to a group of disorders characterized by chronic inflammation of the digestive tract.
The two main types are:
- Crohn’s Disease: Can affect any part of the gastrointestinal tract (from mouth to anus), but most commonly affects the end of the small intestine (ileum) and the beginning of the colon. It can involve all layers of the bowel wall.
- Ulcerative Colitis: Primarily affects the colon and rectum, involving inflammation and ulcers in the innermost lining of the colon.
IBD vs. IBS: What’s the Difference?
IBD is often confused with Irritable Bowel Syndrome (IBS), but they are different conditions:
- IBD involves structural inflammation and can lead to serious complications.
- IBS is a functional disorder without visible inflammation or tissue damage.
Causes and Risk Factors
The exact cause of IBD is not fully understood, but it is believed to involve a combination of genetic, environmental, and immune system factors.
Key Contributing Factors:
- Immune System Dysfunction: An abnormal immune response may cause the body to attack its own intestinal tissue.
- Genetics: Having a close relative with IBD increases risk.
- Environmental Factors:
- Smoking (particularly associated with Crohn’s disease)
- Urban living
- Westernized diets high in processed foods
- Age: Most cases are diagnosed between ages 15 and 35, though it can occur at any age.
- Ethnicity: Higher prevalence in individuals of Northern European descent and Ashkenazi Jewish heritage.
Importantly, IBD is not caused by stress or diet alone, although these factors may influence symptoms.
Symptoms and Clinical Presentation
Symptoms can vary depending on the type and severity of IBD. They often follow a pattern of flare-ups (active inflammation) and remission (periods of fewer or no symptoms).
Common Symptoms:
- Persistent diarrhea
- Abdominal pain and cramping
- Rectal bleeding
- Urgency to have a bowel movement
- Fatigue
- Weight loss
- Reduced appetite
Additional Symptoms (May Include):
- Fever
- Anemia (due to blood loss or nutrient malabsorption)
- Joint pain
- Skin rashes
- Eye inflammation
- Delayed growth in children
Severe cases may lead to complications such as bowel obstruction, fistulas (abnormal connections between organs), or colon cancer.
Diagnosis and Screening
Diagnosing IBD typically involves a combination of clinical evaluation, laboratory tests, imaging, and endoscopy.
Common Diagnostic Tools:
- Blood tests: To detect anemia or markers of inflammation (e.g., C-reactive protein).
- Stool tests: To rule out infections and assess inflammatory markers (such as fecal calprotectin).
- Colonoscopy: The gold standard for diagnosis; allows direct visualization and biopsy of the colon.
- Imaging studies:
- CT scan
- MRI
- Small bowel imaging (for Crohn’s disease)
Early diagnosis is important to begin appropriate treatment and prevent complications.
Treatment and Management Options
While there is currently no cure for IBD, treatment aims to:
- Reduce inflammation
- Achieve and maintain remission
- Prevent complications
- Improve quality of life
Medication Options:
- Aminosalicylates (5-ASAs): Often used for mild to moderate ulcerative colitis.
- Corticosteroids: Used short-term to control flares.
- Immunomodulators: Suppress the immune response (e.g., azathioprine).
- Biologic therapies: Target specific immune system pathways (e.g., anti-TNF agents like infliximab).
- Small molecule inhibitors: Such as JAK inhibitors for moderate to severe cases.
Surgical Options:
- Ulcerative colitis: Removal of the colon (colectomy) can be curative.
- Crohn’s disease: Surgery may address complications (e.g., strictures, fistulas), but disease recurrence is possible.
Treatment plans are individualized based on disease severity, location, response to prior therapies, and overall health.
Prevention and Lifestyle Considerations
There is no known way to prevent IBD completely. However, certain lifestyle strategies may help manage symptoms and reduce flare-ups.
Helpful Strategies:
- Smoking cessation, especially in Crohn’s disease
- Balanced nutrition:
- Avoid trigger foods during flares (e.g., high-fiber foods if strictures are present)
- Consider low-residue diets when advised
- Regular medical follow-up
- Stress management techniques:
- Mindfulness
- Regular exercise
- Cognitive behavioral therapy
- Vaccinations: Particularly important for individuals on immunosuppressive medications
Patients with longstanding ulcerative colitis or extensive Crohn’s colitis may require routine colon cancer screening due to increased risk.
When to Seek Medical Care
Immediate medical evaluation is warranted for:
- Severe abdominal pain
- High fever
- Persistent vomiting
- Significant rectal bleeding
- Signs of dehydration
Prompt assessment can prevent serious complications.
Conclusion
Inflammatory Bowel Disease (IBD) is a chronic inflammatory condition of the digestive tract that includes Crohn’s disease and ulcerative colitis. Although it can be life-altering, early diagnosis and modern treatment strategies allow many individuals to achieve long-term remission and lead fulfilling lives.
Understanding the symptoms, risk factors, and management options empowers patients and caregivers to seek appropriate medical care and participate actively in treatment decisions.
Disclaimer
This article is for educational purposes only and does not constitute medical advice. If you are experiencing symptoms or have concerns about Inflammatory Bowel Disease, please consult a qualified healthcare professional for personalized evaluation and treatment guidance.