GERD: Understanding Gastroesophageal Reflux Disease

Gastroesophageal reflux disease (GERD) is a common digestive condition that affects millions of people worldwide. While occasional heartburn is something many individuals experience, GERD refers to chronic, persistent acid reflux that can significantly impact quality of life and lead to complications if left untreated.
Understanding GERD—its causes, symptoms, diagnosis, and management—can help individuals recognize when to seek medical care and take informed steps toward better digestive health.
Overview / Definition
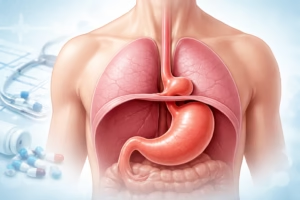
Gastroesophageal reflux disease (GERD) is a chronic digestive disorder in which stomach acid—or sometimes stomach contents—flows backward into the esophagus (the tube connecting the mouth to the stomach).
Normally, a ring of muscle called the lower esophageal sphincter (LES) acts as a valve, opening to allow food into the stomach and closing to prevent backflow. In GERD, this valve becomes weakened or relaxes inappropriately, leading to frequent acid reflux.
Occasional reflux is common and not necessarily a disease. GERD is diagnosed when reflux:
- Occurs at least twice per week, or
- Causes troublesome symptoms or complications
Causes and Risk Factors
GERD develops due to a combination of anatomical, physiological, and lifestyle-related factors.
Common Causes
- Weak or dysfunctional lower esophageal sphincter (LES)
- Hiatal hernia, where part of the stomach pushes upward through the diaphragm
- Delayed stomach emptying
Risk Factors
Certain factors increase the likelihood of developing GERD:
- Obesity or overweight
- Pregnancy
- Smoking
- Excessive alcohol consumption
- Diet high in fatty, fried, or spicy foods
- Frequent consumption of caffeine or carbonated beverages
- Large or late-night meals
- Certain medications (e.g., NSAIDs, calcium channel blockers)
Understanding these risk factors can help guide preventive strategies and symptom control.
Symptoms / Clinical Presentation
GERD symptoms can vary in severity and frequency. The most common symptoms include:
Typical Symptoms
- Heartburn (burning sensation in the chest)
- Acid regurgitation (sour or bitter-tasting fluid in the throat or mouth)
Other Possible Symptoms
- Chest pain (sometimes mistaken for heart-related pain)
- Difficulty swallowing (dysphagia)
- Chronic cough
- Hoarseness or sore throat
- Sensation of a lump in the throat
- Worsening symptoms after meals or when lying down
Alarm Symptoms (Require Prompt Medical Attention)
- Unintentional weight loss
- Persistent vomiting
- Difficulty or pain with swallowing
- Gastrointestinal bleeding (vomiting blood or black stools)
These may indicate complications or alternative diagnoses and should be evaluated by a healthcare professional promptly.
Diagnosis / Screening
GERD is often diagnosed based on symptoms and medical history. If symptoms are classic and uncomplicated, healthcare providers may recommend an initial trial of medication.
Diagnostic Tools
If symptoms persist or complications are suspected, further tests may include:
- Upper endoscopy (EGD): Visual examination of the esophagus and stomach
- Ambulatory pH monitoring: Measures acid exposure in the esophagus
- Esophageal manometry: Assesses esophageal muscle function
- Imaging studies: Sometimes used to identify hiatal hernia or other structural issues
Screening for complications like Barrett’s esophagus may be recommended for individuals with longstanding GERD and additional risk factors.
Treatment / Management Options
GERD management typically involves a combination of lifestyle changes and medications. In some cases, surgical interventions may be considered.
1. Lifestyle Modifications
Often the first step in management:
- Eating smaller, more frequent meals
- Avoiding trigger foods (e.g., spicy, fatty, acidic foods)
- Not lying down within 2–3 hours after eating
- Elevating the head of the bed by 6–8 inches
- Weight loss (if overweight)
- Smoking cessation
- Limiting alcohol intake
2. Medications
Medications help reduce acid production or neutralize acid:
- Antacids: Provide quick, short-term relief
- H2 receptor blockers (e.g., famotidine): Reduce acid production
- Proton pump inhibitors (PPIs) (e.g., omeprazole): More potent acid suppression and commonly used for moderate to severe GERD
Long-term use of certain medications should be monitored by a healthcare provider due to potential side effects.
3. Surgical and Procedural Options
For individuals who do not respond to medical therapy or prefer alternatives:
- Fundoplication: Reinforces the lower esophageal sphincter
- LINX device: Magnetic ring placed around the LES
- Endoscopic procedures aimed at strengthening the valve
Surgical options are typically reserved for selected patients after careful evaluation.
Prevention and Lifestyle Considerations
While not all cases can be prevented, certain strategies can significantly reduce the risk or severity of GERD:
- Maintain a healthy body weight
- Eat balanced meals with moderate portion sizes
- Identify and avoid personal trigger foods
- Practice mindful eating (eat slowly, chew thoroughly)
- Avoid tight clothing that increases abdominal pressure
- Manage stress levels
Long-term, consistent lifestyle adjustments can help reduce symptom recurrence and improve overall well-being.
Possible Complications
When left untreated, chronic GERD may lead to:
- Esophagitis (inflammation of the esophagus)
- Esophageal strictures (narrowing due to scar tissue)
- Barrett’s esophagus, a precancerous condition
- Increased risk of esophageal adenocarcinoma (rare but serious)
Timely evaluation and appropriate management significantly reduce the risk of these complications.
Conclusion
Gastroesophageal reflux disease (GERD) is a common but manageable condition characterized by chronic acid reflux. While occasional heartburn is normal, frequent or severe symptoms may indicate underlying disease requiring medical attention.
Effective management typically includes a combination of lifestyle modifications, medications, and, in select cases, procedural interventions. Recognizing symptoms early and seeking appropriate care can help prevent complications and improve quality of life.
Disclaimer: This article is for educational purposes only and does not substitute professional medical advice. If you experience persistent symptoms of acid reflux or have concerning signs such as difficulty swallowing or unexplained weight loss, consult a qualified healthcare professional for proper evaluation and guidance.