How to Treat Green Nail Syndrome: A Comprehensive Guide
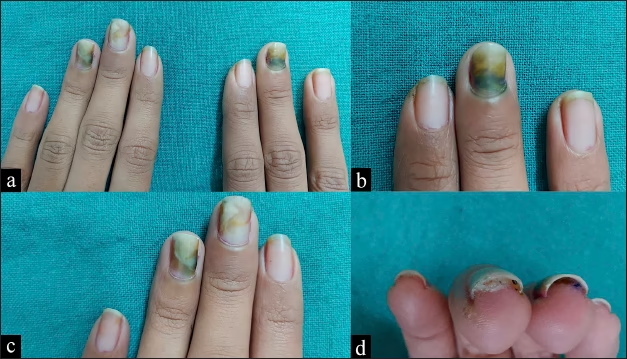
Green Nail Syndrome (GNS) is a relatively common nail condition characterized by a distinctive green discoloration caused by bacterial infection. Although it is typically not life-threatening, it can be persistent, cosmetically concerning, and occasionally uncomfortable.
The condition is most often associated with prolonged exposure to moisture and minor nail damage, which create an environment conducive to bacterial growth. A clear understanding of its causes, symptoms, and treatment options is essential for effective management and prevention. This article provides a detailed and structured explanation of Green Nail Syndrome, including practical home care strategies and medical treatments.
What Is Green Nail Syndrome?
Green Nail Syndrome, also known as chloronychia, occurs when the bacterium Pseudomonas aeruginosa colonizes the nail plate or the space beneath it. This organism thrives in moist environments and produces a pigment called pyocyanin, which gives the nail its characteristic green or blue-green appearance.
The infection often develops when there is a separation between the nail and the nail bed, a condition known as onycholysis. This separation creates a sheltered space where moisture and bacteria can accumulate, facilitating infection.
Key Risk Factors
Frequent Exposure to Moisture
Repeated contact with water, such as during dishwashing or swimming, creates a persistently damp environment that promotes bacterial growth.
Nail Trauma or Separation
Damage to the nail or lifting of the nail plate allows bacteria to enter and colonize the underlying space.
Poor Nail Hygiene
Inadequate cleaning or prolonged use of artificial nails can trap moisture and bacteria, increasing infection risk.
Pre-Existing Fungal Infections
Conditions such as athlete’s foot weaken the nail structure and create an environment that supports secondary bacterial infections.
Recognizing Symptoms and Diagnosis
Common Symptoms
Nail Discoloration
The most prominent sign is a green, blue-green, or dark green discoloration beneath the nail.
Nail Separation
The nail may lift away from the nail bed, creating a visible gap.
Mild Discomfort
Some individuals may experience tenderness around the nail edges.
Odor
In certain cases, a mild unpleasant smell may be present due to bacterial activity.
Diagnosis
Diagnosis is typically based on clinical examination. Healthcare professionals may visually inspect the nail and assess associated symptoms.
In uncertain cases, laboratory testing may be conducted. Nail samples can be analyzed through bacterial cultures to confirm the presence of Pseudomonas aeruginosa. Additionally, fungal infections may be ruled out using specialized tests.
Home Remedies for Mild Cases
Vinegar Soaks
A diluted vinegar solution creates an acidic environment that inhibits bacterial growth. Regular soaking of the affected nail can help control infection in early stages.
Tea Tree Oil Application
Tea tree oil possesses natural antimicrobial properties. When diluted appropriately, it can be applied to the affected area to reduce bacterial load.
Use of Alcohol or Hydrogen Peroxide
Cleaning the nail with antiseptic agents such as isopropyl alcohol or hydrogen peroxide helps disinfect the area and limit bacterial proliferation.
Maintaining Dry and Trimmed Nails
Keeping the nail short and dry is critical. Removing loose portions of the nail reduces spaces where bacteria can thrive, while proper drying minimizes moisture retention.
Over-the-Counter and Topical Treatments
Antiseptic Solutions
Topical antiseptics, including iodine-based solutions, help reduce bacterial contamination when applied regularly.
Antibiotic Ointments
Products such as mupirocin or bacitracin can be applied under the nail edge to directly target bacterial growth.
Nail Strengthening Products
Strengthening lacquers support nail integrity and help the nail reattach to the nail bed, reducing the likelihood of recurrent infection.
Prescription and Professional Treatments
Topical Prescription Antibiotics
Medications such as gentamicin or ciprofloxacin solutions are applied directly to the affected area and are effective in treating persistent infections.
Oral Antibiotics
In severe or widespread cases, oral antibiotics may be prescribed to eliminate deeper infections.
Nail Debridement
Healthcare professionals may remove damaged or infected portions of the nail to improve treatment effectiveness and promote healing.
Advanced Therapies
Emerging treatments, including laser and photodynamic therapy, aim to eliminate bacteria through targeted energy delivery. These approaches may be considered in resistant cases.
Preventing Future Episodes
Proper Nail Hygiene
Regular cleaning and thorough drying of nails are essential in preventing recurrence.
Use of Protective Gloves
Wearing waterproof gloves during activities involving water or chemicals reduces exposure to moisture.
Nail Care Practices
Limiting prolonged use of nail polish and ensuring proper sterilization of nail tools helps maintain nail health.
Footwear and Moisture Control
Allowing shoes to dry properly and using moisture-wicking socks reduces damp conditions that favor bacterial growth.
Prompt Treatment of Fungal Infections
Addressing fungal infections early prevents secondary bacterial colonization.
Conclusion
Green Nail Syndrome is a manageable condition when identified early and treated appropriately. Initial management often involves simple home remedies and improved hygiene practices, while more persistent cases may require medical intervention.
Moreover, preventive strategies play a crucial role in reducing recurrence. By maintaining proper nail care, minimizing moisture exposure, and seeking timely professional guidance when needed, individuals can restore nail health and prevent future infections.