Skin Cancer: Causes, Symptoms, Diagnosis, and Prevention
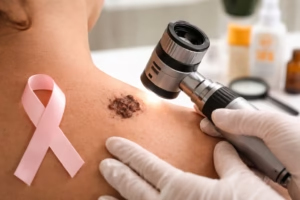
Skin cancer is the most common type of cancer worldwide, affecting millions of people each year. While hearing the word “cancer” can be frightening, the good news is that most skin cancers are highly treatable, especially when detected early. Increased awareness, early diagnosis, and preventive strategies play a critical role in reducing both the risk and impact of this condition.
This article provides an evidence-based overview of skin cancer, including its causes, warning signs, diagnostic approaches, treatment options, and prevention strategies.
Overview / Definition
Skin cancer occurs when abnormal skin cells begin to grow uncontrollably. Most skin cancers develop in areas exposed to the sun, such as the face, neck, scalp, and arms. However, they can occur anywhere on the body.
There are three primary types of skin cancer:
1. Basal Cell Carcinoma (BCC)
- The most common form
- Typically slow-growing
- Rarely spreads (metastasizes)
- Often appears as a pearly or flesh-colored bump
2. Squamous Cell Carcinoma (SCC)
- The second most common type
- May grow more quickly than BCC
- Has a higher risk of spreading if untreated
- Often presents as a scaly red patch or sore that doesn’t heal
3. Melanoma
- Less common but more dangerous
- Develops from pigment-producing cells (melanocytes)
- More likely to spread to other parts of the body
- Often appears as a new mole or changes in an existing mole
Early detection is essential—particularly in melanoma, which can become life-threatening if not treated promptly.
Causes and Risk Factors
The primary cause of most skin cancers is exposure to ultraviolet (UV) radiation, either from sunlight or artificial sources like tanning beds. UV radiation damages the DNA in skin cells, leading to mutations that can result in cancer.
Major Risk Factors Include:
- Excessive sun exposure, especially without protection
- Frequent sunburns, particularly during childhood
- Indoor tanning bed use
- Fair skin, light hair, or light-colored eyes
- A high number of moles or atypical moles
- Family history of skin cancer
- Weakened immune system (e.g., organ transplant recipients)
- Older age, though melanoma can occur in younger adults
While UV exposure is the leading risk factor, skin cancer can happen in people of all skin tones. Although individuals with darker skin have lower overall risk, diagnosis may occur later, sometimes leading to worse outcomes.
Symptoms or Clinical Presentation
Skin cancer symptoms vary depending on the type, but early recognition significantly improves treatment success.
Common Warning Signs:
- A new growth or sore that does not heal
- A spot or mole that changes in size, shape, or color
- A lesion that bleeds, crusts, or itches persistently
- A scaly red patch or wart-like growth
The ABCDE Rule for Melanoma
The ABCDE guideline helps identify suspicious moles:
- A – Asymmetry: One half doesn’t match the other
- B – Border: Edges are irregular or poorly defined
- C – Color: Varies in shades of brown, black, red, or white
- D – Diameter: Larger than 6 mm (about the size of a pencil eraser)
- E – Evolving: Changes in size, shape, or color
If any of these characteristics are observed, medical evaluation is recommended.
Diagnosis and Screening
Clinical Examination
A healthcare professional begins with a thorough skin examination. Suspicious lesions are evaluated visually and may be examined using dermoscopy, a specialized magnifying tool.
Skin Biopsy
If cancer is suspected, a biopsy is performed:
- A small sample (or the entire lesion) is removed
- The tissue is examined under a microscope
- Determines type and depth of cancer
Staging (for Melanoma and Advanced SCC)
If melanoma is diagnosed, additional imaging or lymph node evaluation may be necessary to determine whether the cancer has spread.
Screening Recommendations
- Routine self-examinations are encouraged monthly
- Periodic professional skin exams are recommended for high-risk individuals
- There is no universal population-wide screening guideline, but early evaluation of suspicious lesions is critical
Treatment and Management Options
Treatment depends on the type, size, location, and stage of the cancer.
1. Surgical Removal
The most common and often curative treatment.
- Excisional surgery: The cancer and a margin of normal skin are removed
- Mohs micrographic surgery: Removes cancer layer by layer while preserving healthy tissue (often used on the face)
2. Cryotherapy
Freezing precancerous lesions or small cancers using liquid nitrogen.
3. Radiation Therapy
Used for patients who cannot undergo surgery or for advanced cases.
4. Topical Medications
Certain superficial skin cancers may be treated with prescription creams (e.g., imiquimod, 5-fluorouracil).
5. Systemic Treatments (Primarily for Melanoma or Advanced SCC)
- Immunotherapy: Helps the immune system target cancer cells
- Targeted therapy: Attacks specific genetic mutations
- Chemotherapy: Less commonly used today but may be appropriate in certain cases
Prognosis is generally excellent for early-stage basal and squamous cell carcinomas. Melanoma survival rates are also high when caught early.
Prevention and Lifestyle Considerations
Preventive strategies significantly reduce the risk of skin cancer.
Sun Protection Measures:
- Use broad-spectrum sunscreen (SPF 30 or higher) daily
- Reapply sunscreen every 2 hours and after swimming or sweating
- Wear protective clothing, hats, and sunglasses
- Seek shade between 10 a.m. and 4 p.m., when UV exposure is strongest
- Avoid tanning beds
Additional Recommendations:
- Perform regular self-skin checks
- Schedule periodic skin exams if you have risk factors
- Educate children and adolescents about sun safety
Consistent preventive habits can substantially reduce cumulative UV damage over time.
Conclusion
Skin cancer is common but often preventable and highly treatable when detected early. Understanding the different types, recognizing warning signs, and practicing sun protection are crucial steps in reducing risk. Regular self-examinations and prompt medical evaluation of suspicious changes can make a significant difference in outcomes.
While this article provides general educational information, it is not a substitute for professional medical advice. If you have concerns about your skin or notice unusual changes, consult a qualified healthcare professional for proper evaluation and guidance.