Myelofibrosis: Understanding a Rare Bone Marrow Disorder
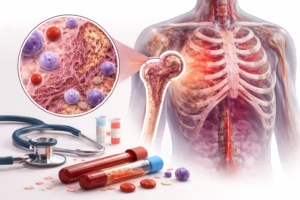
Myelofibrosis is a rare but serious blood cancer that affects the bone marrow’s ability to produce healthy blood cells. Although it progresses slowly in many individuals, it can significantly impact quality of life and overall health if not properly managed. Increasing awareness and understanding of this condition is essential for early detection, appropriate treatment, and improved outcomes.
In this article, we’ll explore what myelofibrosis is, its causes and symptoms, how it is diagnosed, available treatment options, and important lifestyle considerations.
Overview / Definition
Myelofibrosis (MF) is a type of chronic blood cancer classified as a myeloproliferative neoplasm (MPN). In this condition, abnormal changes occur in the bone marrow—the soft, spongy tissue inside bones responsible for producing blood cells.
Over time, scar tissue (fibrosis) replaces healthy bone marrow. This scarring:
- Reduces the production of normal red blood cells, white blood cells, and platelets
- Causes abnormal blood cell formation
- Often leads to enlargement of the spleen (splenomegaly)
Myelofibrosis can occur in two forms:
- Primary myelofibrosis: Develops on its own without a preceding blood disorder
- Secondary myelofibrosis: Develops as a complication of other myeloproliferative disorders such as:
- Polycythemia vera
- Essential thrombocythemia
Although considered a chronic condition, myelofibrosis can, in some cases, progress to acute leukemia.
Causes and Risk Factors
The exact cause of myelofibrosis is not fully understood. However, research has identified genetic mutations in blood-forming stem cells that contribute to the condition.
Common Genetic Mutations
Several acquired (not inherited) mutations are frequently involved:
- JAK2 mutation (most common)
- CALR mutation
- MPL mutation
These mutations lead to abnormal signaling in bone marrow cells, resulting in uncontrolled production and eventual scarring.
Risk Factors
While myelofibrosis can occur at any age, it is more common in:
- Adults over age 50
- Individuals with previous myeloproliferative disorders
- People previously exposed to high levels of radiation
- Those exposed to certain industrial chemicals (e.g., benzene)
It’s important to note that most cases occur without a clearly identifiable environmental trigger.
Symptoms and Clinical Presentation
Myelofibrosis often develops gradually. Some individuals are asymptomatic in early stages and are diagnosed during routine blood tests.
Common Symptoms
As the disease progresses, symptoms may include:
- Fatigue and weakness (due to anemia)
- Shortness of breath
- Pale skin
- Easy bruising or bleeding
- Frequent infections
- Night sweats
- Fever
- Unintentional weight loss
- Bone or joint pain
Enlarged Spleen (Splenomegaly)
One hallmark feature is an enlarged spleen, which may cause:
- Pain or fullness in the upper left abdomen
- Early satiety (feeling full quickly when eating)
Because the bone marrow becomes fibrotic, blood cell production may shift to the spleen and liver—a process called extramedullary hematopoiesis.
Diagnosis and Screening
There is no routine screening test for myelofibrosis in the general population. Diagnosis usually occurs after abnormal blood test results or evaluation of symptoms.
Diagnostic Tests May Include:
- Complete blood count (CBC):
- Low red blood cells (anemia)
- Abnormal white blood cells
- Platelet abnormalities
- Peripheral blood smear to examine cell shape and appearance
- Bone marrow biopsy, which confirms fibrosis and abnormal cell growth
- Genetic testing for JAK2, CALR, or MPL mutations
- Imaging studies to assess spleen enlargement
Severity is often assessed using prognostic scoring systems that evaluate:
- Age
- Blood counts
- Symptoms
- Genetic findings
Treatment and Management Options
Treatment depends on:
- Severity of symptoms
- Risk classification
- Age and overall health
- Genetic profile
Some individuals with mild disease may be closely monitored without immediate treatment (a “watchful waiting” approach).
Medications
Common therapies include:
- JAK inhibitors (e.g., ruxolitinib, fedratinib)
- Help reduce spleen size
- Improve symptoms
- Anemia treatments, such as:
- Blood transfusions
- Androgen therapy
- Erythropoiesis-stimulating agents
- Hydroxyurea to control elevated blood counts
- Corticosteroids (in selected cases)
Stem Cell Transplant
An allogeneic stem cell transplant is currently the only potentially curative treatment. However, it carries significant risks and is usually reserved for:
- Younger patients
- High-risk disease
- Those with suitable donor matches
Supportive Care
Supportive management plays a crucial role and includes:
- Symptom control
- Management of infections
- Pain relief
- Nutritional support
Prevention and Lifestyle Considerations
There is currently no known way to prevent myelofibrosis, particularly because most genetic mutations occur spontaneously.
However, individuals diagnosed with the condition can take steps to support overall health:
- Maintain a balanced, nutrient-rich diet
- Engage in moderate physical activity as tolerated
- Avoid tobacco use
- Keep vaccinations up to date (after consulting healthcare providers)
- Attend regular follow-up appointments
Emotional and psychological support—through counseling or support groups—can also help individuals cope with chronic illness.
Conclusion
Myelofibrosis is a rare but complex blood cancer characterized by scarring of the bone marrow and impaired blood cell production. While some individuals experience minimal symptoms, others may develop significant complications, including anemia and spleen enlargement.
Advances in genetic research and targeted therapies—particularly JAK inhibitors—have substantially improved symptom management and quality of life. In select cases, stem cell transplantation offers the possibility of cure.
Early diagnosis, individualized treatment, and ongoing medical monitoring are critical to optimizing outcomes.
Disclaimer:
This article is intended for educational purposes only and should not be considered medical advice. If you have symptoms or concerns about myelofibrosis or any blood disorder, please consult a qualified healthcare professional for personalized evaluation and treatment.