Introduction
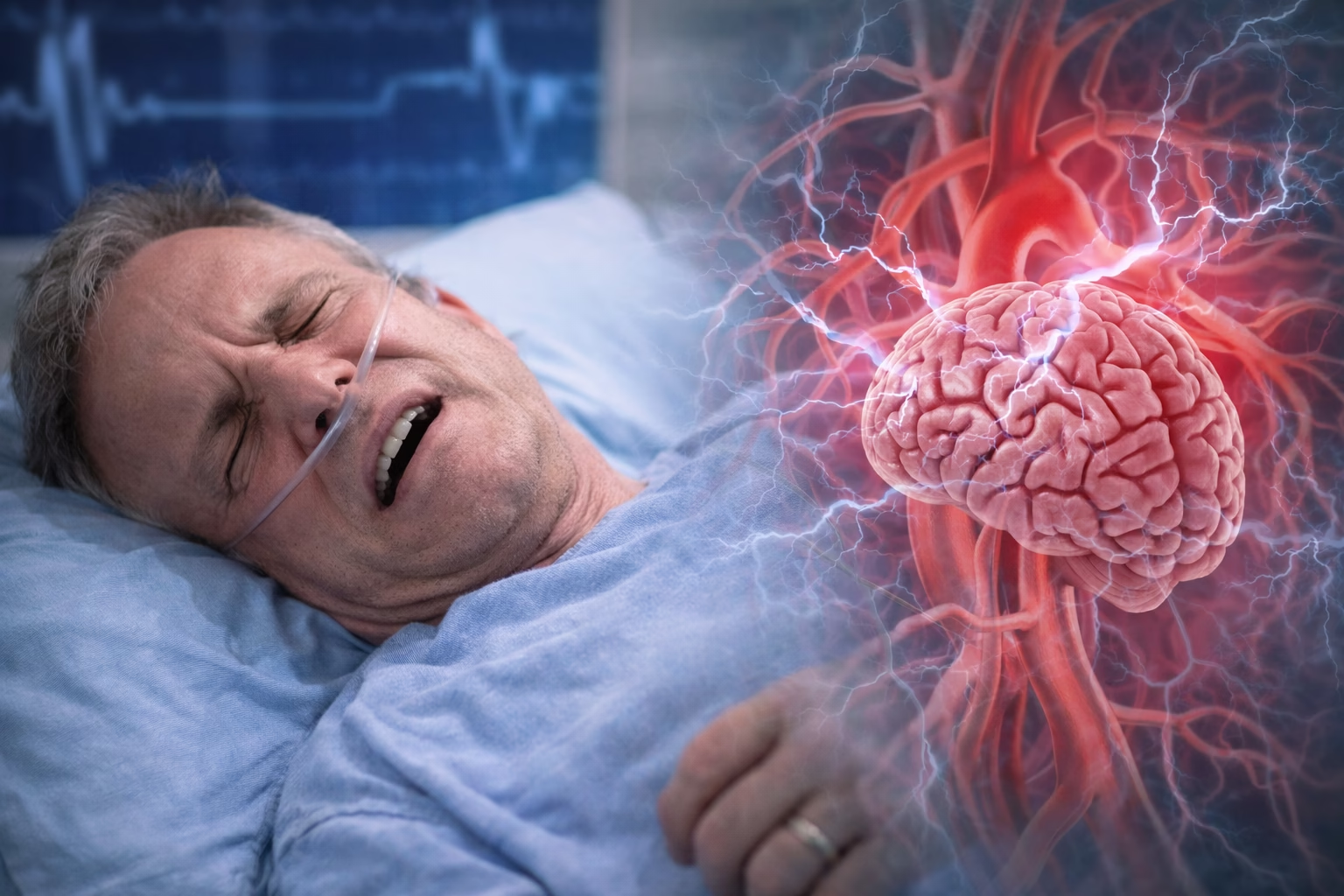
Hypertension, or high blood pressure, is most commonly discussed in relation to the heart, blood vessels, kidneys, and risk of stroke. However, its effects are not limited to the cardiovascular system. In severe cases, especially when blood pressure rises rapidly or remains dangerously uncontrolled, hypertension can also affect the brain and trigger neurological emergencies, including seizures. A hypertensive crisis is generally defined as blood pressure of 180/120 mm Hg or higher, and when this occurs with symptoms such as confusion, severe headache, visual changes, or seizures, urgent medical evaluation is required.
- Seizures usually occur when blood pressure is severely elevated, abrupt, or causes acute brain dysfunction rather than from routine mild hypertension.
- Main mechanisms include hypertensive encephalopathy, posterior reversible encephalopathy syndrome, ischemic or hemorrhagic stroke, and eclampsia causing cerebral edema.
- Higher risk with long standing uncontrolled hypertension, abrupt antihypertensive withdrawal, chronic kidney disease, diabetes, and pregnancy related hypertension.
- Prevent with medication adherence, lifestyle measures, routine blood pressure monitoring, and prompt emergency care when neurological symptoms or seizures appear.
The key clinical point is that hypertension does not usually cause seizures in the same way that epilepsy does. Rather, seizures may occur when extreme or poorly controlled blood pressure leads to acute brain dysfunction, swelling, stroke, or pregnancy related hypertensive complications such as eclampsia. Therefore, the answer is yes, hypertension can cause seizures, but this usually happens in the setting of a serious medical emergency rather than routine mildly elevated blood pressure.
Understanding Hypertension
Hypertension refers to persistently elevated blood pressure. In general medical practice, blood pressure at or above 130/80 mm Hg is considered high. What makes hypertension especially dangerous is that it can remain silent for years. Many people feel normal and have no obvious warning signs while damage is gradually occurring inside blood vessels and vital organs.
Over time, this chronic pressure injures the lining of arteries and makes them stiffer, narrower, and more vulnerable to blockage or rupture. That is why uncontrolled hypertension is strongly linked to heart disease, heart failure, kidney damage, visual problems, and both ischemic and hemorrhagic stroke. When the blood vessels supplying the brain are affected, neurological complications become possible, including the kinds of conditions that can provoke seizures.
It is also important to distinguish between long term hypertension and a hypertensive crisis. Chronic hypertension causes cumulative damage over time, whereas a hypertensive crisis can produce sudden organ injury. In the brain, this rapid rise may overwhelm the normal mechanisms that regulate cerebral blood flow. When that happens, fluid can leak into brain tissue, causing swelling and acute neurological symptoms.
What Are Seizures?
A seizure is a sudden, abnormal burst of electrical activity in the brain. The clinical presentation depends on which brain regions are involved and how widely the abnormal electrical activity spreads.
A focal seizure begins in one area of the brain. It may cause localized twitching, unusual sensations, strange smells or tastes, visual changes, or brief confusion. In some cases, the person remains aware. In others, awareness becomes impaired.
A generalized seizure involves both sides of the brain more broadly and may lead to convulsions, loss of consciousness, body stiffening, rhythmic jerking, or staring spells. Some generalized seizures are dramatic and obvious, while others are brief and subtle.
Seizures have many causes. Epilepsy is one, but not the only one. They may also result from head trauma, infections, metabolic disturbances, medication withdrawal, toxic exposures, stroke, or acute brain swelling. In the case of severe hypertension, the seizure usually reflects a secondary disturbance in the brain rather than a primary seizure disorder.
Can High Blood Pressure Cause Seizures?
Yes, but usually only when the blood pressure is severely elevated, rises abruptly, or produces complications such as hypertensive encephalopathy, posterior reversible encephalopathy syndrome, stroke, or eclampsia. Mild or moderately elevated blood pressure alone does not typically trigger seizures. The seizure risk emerges when brain tissue is injured or irritated by the consequences of extreme blood pressure dysregulation.
This distinction matters. A person with long standing hypertension may never experience a seizure. By contrast, someone with a sudden hypertensive emergency can develop neurological symptoms rapidly. In practical terms, the seizure is a sign that the hypertension has moved beyond a routine chronic condition and has become a medical emergency requiring immediate treatment.
How High Blood Pressure Can Lead to Seizures
Hypertensive Encephalopathy
Hypertensive encephalopathy is one of the clearest mechanisms linking hypertension to seizures. It is a hypertensive emergency in which severely elevated blood pressure overwhelms the brain’s autoregulatory system, disrupts the blood brain barrier, and leads to brain edema, meaning swelling caused by excess fluid. This swelling interferes with normal brain function and may produce headache, nausea, vomiting, confusion, visual disturbances, altered mental status, and seizures.
Under normal conditions, cerebral blood vessels constrict or dilate to maintain stable brain perfusion. In hypertensive encephalopathy, the pressure rises beyond what these vessels can safely manage. The result is leakage of fluid into surrounding tissues and widespread neurological dysfunction. The seizure in this context is therefore a manifestation of acute brain irritation from edema and loss of normal electrical stability.
Posterior Reversible Encephalopathy Syndrome, PRES
Posterior Reversible Encephalopathy Syndrome, often called PRES, is closely related to severe hypertension and is one of the most important seizure associated neurological syndromes in this setting. PRES is characterized by acute or subacute onset of seizures, headache, encephalopathy, and visual disturbances, often in the setting of uncontrolled or rapidly rising blood pressure. MRI commonly shows vasogenic edema, classically in the parieto occipital regions of the brain, although other regions may also be involved.
The term “reversible” reflects the fact that many patients improve when the underlying cause is recognized and treated promptly. However, reversibility is not guaranteed, and delayed care can lead to lasting neurological injury. Seizures are particularly common in PRES because the swollen brain tissue becomes electrically unstable. Thus, severe hypertension can lead to seizures by producing a radiologically and clinically recognizable syndrome of brain edema.
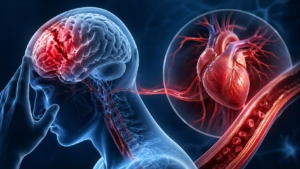
Stroke and Mini Strokes
Hypertension is a major risk factor for both ischemic stroke, in which a vessel becomes blocked, and hemorrhagic stroke, in which a vessel ruptures and bleeds into brain tissue. High blood pressure damages arteries throughout the body and makes the vessels in the brain more likely to clog or burst. Because strokes injure brain tissue directly, they can provoke seizures either immediately or later in the recovery period.
In hemorrhagic stroke, seizures may occur because blood itself is irritating to the brain and because increased pressure from bleeding disrupts surrounding tissue. In ischemic stroke, damaged neurons may become electrically unstable, especially if the cortical areas are involved. Therefore, hypertension may lead to seizures indirectly by first causing the stroke that then triggers seizure activity.
Eclampsia in Pregnancy
Pregnancy introduces a special and clinically urgent scenario. Some pregnant women develop pre eclampsia, a condition marked by high blood pressure and other signs of organ stress. When seizures occur in this setting, the condition is called eclampsia. Eclampsia is a life threatening emergency for both the mother and the baby. It is also one of the clearest examples of hypertension causing seizures.
The mechanisms overlap with hypertensive encephalopathy and PRES, including endothelial dysfunction, cerebral edema, and impaired autoregulation of blood flow in the brain. Because of the high stakes, any pregnant patient with high blood pressure, headache, visual symptoms, confusion, or seizure activity requires urgent medical evaluation.
Who Is at Higher Risk?
Not every person with hypertension will experience seizures. The risk becomes more significant when other clinical factors increase the chance of acute brain injury.
People with long standing, poorly controlled hypertension are at higher risk because chronic vascular damage makes the brain more vulnerable to sudden pressure surges. Those who abruptly stop antihypertensive medication may also be at risk because blood pressure can rebound sharply, sometimes precipitating a hypertensive emergency.
Individuals with chronic kidney disease are more vulnerable because the kidneys play a major role in blood pressure regulation, and kidney dysfunction can intensify blood pressure instability. People with diabetes and other vascular disorders face added risk because their blood vessels are already under strain. Pregnant patients with pregnancy related hypertension are a special high risk group because of the possibility of eclampsia.
In essence, seizure risk rises when hypertension is severe, unstable, or combined with other conditions that impair vascular health or brain perfusion.
Recognizing Warning Signs
Early recognition is extremely important because seizures related to hypertension often occur alongside other signs of acute brain dysfunction.
A sudden, severe headache, particularly one described as thunderclap in onset, may suggest hemorrhage, hypertensive encephalopathy, or another neurological emergency. Visual disturbances, such as blurred vision, double vision, or sudden loss of vision, are especially concerning because they can occur in PRES or severe hypertensive crises. Confusion, agitation, drowsiness, or altered mental state suggest that the brain is already being affected by the blood pressure elevation. Nausea and vomiting may appear when intracranial pressure rises or when the brain becomes swollen. Finally, uncontrolled jerking, convulsions, or loss of responsiveness indicate active seizure activity and require immediate emergency care.
These symptoms become even more alarming if a blood pressure reading is 180/120 mm Hg or higher. In that situation, the concern is not merely that the blood pressure is elevated, but that organ damage may already be occurring.
Diagnosis and Testing
When clinicians suspect that hypertension may be contributing to seizures, the diagnostic approach aims to answer two questions. First, is the person having a seizure or another neurological event. Second, what hypertensive or vascular complication is causing it.
Continuous or repeated blood pressure monitoring helps determine whether the person is in hypertensive crisis and whether the elevation is sustained. Brain imaging, usually CT or MRI, is used to look for bleeding, swelling, stroke, or characteristic changes of PRES. MRI is particularly useful for identifying vasogenic edema typical of PRES, while CT may be used rapidly in emergency settings to exclude hemorrhage.
An electroencephalogram, EEG, may be ordered to detect ongoing abnormal electrical activity in the brain, especially if the diagnosis is uncertain or if nonconvulsive seizures are suspected. Blood tests are also important because metabolic abnormalities such as sodium disturbances, kidney failure, infection, or toxic exposures can cause or worsen seizures and may coexist with hypertension. Therefore, the workup is not limited to blood pressure alone. It aims to identify the full medical picture so treatment can be targeted correctly.
Treatment and Prevention Strategies
Medication Adherence
One of the most important preventive measures is taking antihypertensive medication exactly as prescribed. Blood pressure medicines help reduce long term vascular damage and lower the risk of hypertensive emergencies. Abrupt discontinuation can be dangerous because it may cause rebound hypertension, which in some patients can become severe enough to injure the brain. Therefore, medication changes should always be guided by a clinician.
Lifestyle Modification
Lifestyle remains a cornerstone of blood pressure control. Dietary patterns such as the DASH diet, which emphasizes fruits, vegetables, whole grains, and lean proteins, can help lower blood pressure. Regular exercise improves vascular health and supports weight control. Reducing sodium intake, limiting alcohol, and avoiding tobacco are also important because each of these factors influences blood pressure and vascular integrity. Although lifestyle measures do not replace medication when it is needed, they strengthen overall blood pressure control and reduce risk over time.
Regular Monitoring
Routine blood pressure monitoring at home can help identify dangerous trends before a crisis develops. Keeping a written or digital log gives clinicians better information for adjusting treatment. Regular follow up visits are important because hypertension management often needs periodic refinement based on age, kidney function, symptoms, and response to therapy. Early detection of poor control is one of the best ways to prevent brain complications.
Emergency Preparedness
People living with severe hypertension, pregnancy related hypertension, or prior hypertensive neurological complications should know the signs of emergency. If a seizure occurs, basic first aid matters. The person should be protected from injury, placed on their side if possible, and observed carefully. Emergency services should be called if the seizure lasts more than five minutes, if repeated seizures occur, if breathing is difficult, if consciousness does not return normally, or if the seizure occurs during pregnancy or with suspected stroke symptoms. These situations require immediate professional care because the underlying cause may be ongoing brain injury.
Conclusion
Hypertension can cause seizures, but it usually does so in the context of a serious medical emergency, not ordinary uncomplicated high blood pressure. The main pathways include hypertensive encephalopathy, PRES, stroke, and eclampsia. In each case, the underlying problem is that severe or rapidly rising blood pressure disrupts normal brain function, causes edema, or injures cerebral blood vessels.
This connection is clinically important because seizures may be one of the clearest signs that blood pressure has moved into dangerous territory. Recognizing warning symptoms early, maintaining blood pressure control, adhering to medication, and seeking urgent medical care when neurological symptoms appear can reduce the risk of permanent injury. In practical terms, protecting the brain is one more reason why hypertension should never be treated as a minor or purely cardiovascular issue.
Disclaimer
This article is for educational purposes only and does not replace professional medical advice, diagnosis, or treatment. Seizures, severe headache, confusion, visual changes, or blood pressure readings in the hypertensive crisis range require urgent medical evaluation.