Ulcerative Colitis: Understanding the Symptoms, Causes, and Management
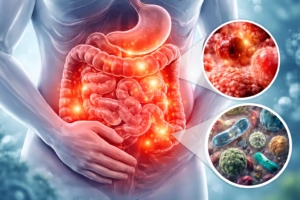
Ulcerative colitis (UC) is a chronic inflammatory bowel disease (IBD) that affects the large intestine, or colon. It can significantly impact daily life, but with appropriate medical care and lifestyle adjustments, many individuals are able to manage their symptoms effectively. Understanding what ulcerative colitis is, how it develops, and the available treatment options can empower patients and caregivers to make informed decisions about health and well-being.
This comprehensive guide explores the essential aspects of ulcerative colitis in clear, medically accurate terms.
Overview / Definition
Ulcerative colitis is a long-term inflammatory condition that affects the lining of the colon and rectum. It causes continuous inflammation and ulcers (small sores) in the innermost lining of the colon.
Unlike Crohn’s disease (another form of inflammatory bowel disease), ulcerative colitis:
- Affects only the colon and rectum
- Involves continuous inflammation (rather than patchy areas)
- Impacts primarily the inner lining of the bowel
The disease typically follows a pattern of flare-ups (periods of active symptoms) and remission (periods when symptoms improve or disappear).
Causes and Risk Factors
The exact cause of ulcerative colitis remains unknown. However, research suggests it develops due to a combination of genetic, immune, and environmental factors.
1. Immune System Dysfunction
In UC, the immune system appears to mistakenly attack the lining of the colon. This abnormal immune response leads to persistent inflammation.
2. Genetic Factors
- Individuals with a family history of ulcerative colitis or other inflammatory bowel diseases are at higher risk.
- Certain genetic variations have been linked to increased susceptibility.
3. Environmental Influences
While not fully understood, potential contributing factors may include:
- Viral or bacterial infections
- Urban living environments
- Diet and lifestyle patterns
- Use of certain medications (e.g., NSAIDs)
4. Age and Ethnicity
- Most commonly diagnosed between ages 15–30 or later between 50–70.
- Higher prevalence in individuals of Ashkenazi Jewish descent.
Importantly, ulcerative colitis is not caused by stress or diet alone, though these factors may influence symptom severity.
Symptoms and Clinical Presentation
Symptoms can vary depending on the severity of inflammation and how much of the colon is affected.
Common Symptoms
- Persistent diarrhea (often with blood or mucus)
- Abdominal pain or cramping
- Rectal bleeding
- Urgency to have bowel movements
- Incomplete bowel emptying
- Fatigue
- Unintended weight loss
Severe Symptoms
- Fever
- Severe abdominal tenderness
- Dehydration
- Rapid heart rate
Extraintestinal Symptoms
UC can also affect other parts of the body, including:
- Joint pain or swelling
- Skin rashes
- Eye inflammation
- Liver disorders
Symptoms may develop gradually or suddenly and typically fluctuate over time.
Diagnosis and Screening
There is no single test for ulcerative colitis. Diagnosis usually involves a combination of:
1. Medical History and Physical Examination
A physician will evaluate symptoms, duration, and family history.
2. Laboratory Tests
- Blood tests (to check for anemia or inflammation)
- Stool tests (to rule out infections)
3. Endoscopy (Colonoscopy)
This is the most definitive diagnostic test. A flexible camera is inserted into the colon to:
- Visualize inflammation
- Assess extent of disease
- Obtain biopsies for microscopic examination
4. Imaging Studies
In some cases, CT or MRI scans are used to evaluate complications.
Classification by Extent
UC is categorized based on how much of the colon is affected:
- Ulcerative proctitis (rectum only)
- Left-sided colitis
- Extensive colitis (most or all of the colon)
Early and accurate diagnosis is essential to reduce complications and guide treatment.
Treatment and Management Options
Although there is currently no cure for ulcerative colitis, treatment focuses on:
- Reducing inflammation
- Achieving and maintaining remission
- Preventing complications
1. Medications
Treatment plans depend on disease severity.
Aminosalicylates (5-ASA)
- Often first-line therapy for mild to moderate UC
- Reduce inflammation in the colon
Corticosteroids
- Used short-term for moderate to severe flares
- Not recommended for long-term maintenance due to side effects
Immunomodulators
- Suppress immune response
- Used in moderate to severe cases
Biologic Therapies
- Target specific inflammatory pathways
- Examples include anti-TNF agents and other targeted biologics
Small Molecule Drugs (e.g., JAK inhibitors)
- Oral agents for moderate to severe UC
2. Surgical Treatment
In cases where medical therapy is ineffective or complications arise, surgery may be necessary. Surgical removal of the colon (proctocolectomy) can:
- Eliminate the disease
- Remove cancer risk associated with affected colon tissue
Surgical options may include creation of an ileal pouch-anal anastomosis (IPAA).
Prevention and Lifestyle Considerations
There is no known way to prevent ulcerative colitis. However, lifestyle choices can help manage symptoms and maintain remission.
Dietary Considerations
No universal “UC diet” exists, but patients may benefit from:
- Keeping a food diary
- Limiting high-fiber foods during flares
- Avoiding trigger foods (e.g., high-fat or spicy items if they worsen symptoms)
- Eating smaller, more frequent meals
Stress Management
Stress does not cause UC but may worsen symptoms. Strategies include:
- Mindfulness meditation
- Exercise
- Counseling or support groups
Smoking
Interestingly, smoking is associated with a lower risk of UC, but the significant health risks of smoking far outweigh any potential benefit. Smoking is not recommended.
Regular Monitoring
Because long-standing UC increases the risk of colorectal cancer:
- Routine colonoscopic surveillance is recommended
- Follow-up intervals are determined by disease duration and severity
Potential Complications
If untreated or poorly managed, ulcerative colitis can lead to:
- Severe bleeding
- Colon perforation
- Toxic megacolon (a life-threatening dilation of the colon)
- Increased risk of colorectal cancer
- Nutritional deficiencies
Prompt medical care reduces these risks significantly.
Conclusion
Ulcerative colitis is a chronic inflammatory condition of the colon that requires comprehensive and ongoing management. While its exact cause remains unclear, advances in medical therapies have significantly improved outcomes. Early diagnosis, appropriate medication, routine monitoring, and supportive lifestyle adjustments are key to maintaining remission and preventing complications.
If you experience persistent digestive symptoms such as rectal bleeding, chronic diarrhea, or unexplained abdominal pain, it is important to seek medical evaluation.
Disclaimer: This article is intended for educational purposes only and does not substitute for professional medical advice, diagnosis, or treatment. Always consult a qualified healthcare provider for evaluation and management of any medical condition.