Eczema: Understanding a Common Chronic Skin Condition

Eczema is a common and often frustrating skin condition that affects people of all ages, from infants to older adults. While it is not contagious, eczema can significantly affect quality of life due to persistent itching, visible skin changes, and frequent flare-ups. This article provides a clear, medically accurate overview of eczema, including its causes, symptoms, diagnosis, and management, using accessible language for a general audience.
Overview / Definition
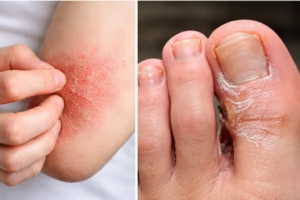
Eczema is a broad term used to describe a group of inflammatory skin conditions characterized by dry, itchy, and inflamed skin. The most common form is atopic dermatitis, which typically begins in childhood but can persist or appear in adulthood.
Eczema is considered a chronic condition with periods of flares and remissions, meaning symptoms can worsen or improve over time. Although there is no cure, many people successfully manage symptoms with appropriate care.
Common types of eczema include:
- Atopic dermatitis (most common)
- Contact dermatitis (allergic or irritant-related)
- Dyshidrotic eczema (affecting hands and feet)
- Nummular eczema (coin-shaped patches)
- Seborrheic dermatitis (often affects scalp and face)
- Stasis dermatitis (associated with poor circulation)
Causes or Risk Factors
Eczema does not have a single cause. Instead, it results from a combination of genetic, immune, and environmental factors.
Key contributing factors include:
- Genetic predisposition
- Family history of eczema, asthma, or allergic rhinitis
- Skin barrier dysfunction
- Reduced ability of the skin to retain moisture and protect against irritants
- Immune system overactivity
- Inflammatory responses that lead to redness and itching
- Environmental triggers
- Soaps, detergents, fragrances
- Pollen, dust mites, animal dander
- Temperature changes or low humidity
- Other risk factors
- Stress
- Certain infections
- Allergies or asthma
Symptoms or Clinical Presentation
Eczema symptoms can vary depending on age, skin tone, eczema type, and disease severity. Symptoms often fluctuate over time.
Common signs and symptoms include:
- Dry, sensitive skin
- Intense itching, which may worsen at night
- Red, inflamed patches
- Rough, scaly, or thickened skin
- Oozing or crusting during severe flare-ups
- Skin darkening or lightening after healing (post-inflammatory changes)
In infants, eczema often appears on the face and scalp, while in older children and adults it commonly affects elbow creases, behind the knees, hands, neck, and wrists.
Diagnosis or Screening
Eczema is primarily a clinical diagnosis, meaning it is diagnosed based on medical history and a physical examination.
Healthcare professionals may consider:
- Pattern and duration of skin symptoms
- Personal or family history of allergies or asthma
- Visual inspection of affected skin areas
In certain cases, additional tests may be performed to rule out other conditions or identify triggers, such as:
- Patch testing (for allergic contact dermatitis)
- Skin swabs if infection is suspected
- Blood tests in select situations
There is no single laboratory test that definitively diagnoses eczema.
Treatment or Management Options
While eczema cannot currently be cured, effective management focuses on reducing symptoms, preventing flare-ups, and maintaining skin health.
Treatment strategies may include:
Skin Care Foundation
- Regular use of fragrance-free moisturizers
- Gentle cleansing with non-irritating products
- Avoiding harsh soaps and frequent hot showers
Medications (as prescribed by healthcare professionals)
- Topical corticosteroids to reduce inflammation during flares
- Topical calcineurin inhibitors for sensitive areas or long-term use
- Topical PDE-4 inhibitors for mild to moderate eczema
- Antihistamines (sometimes used to relieve itching)
- Antibiotics or antivirals if secondary infection occurs
Advanced Therapies (for moderate to severe cases)
- Phototherapy (light therapy)
- Systemic medications or biologic therapies that target immune pathways
Treatment plans are typically individualized and adjusted over time based on response and severity.
Prevention or Lifestyle Considerations
Although eczema cannot always be prevented, certain measures may help reduce flare frequency and severity:
- Maintain consistent daily moisturizing routines
- Identify and avoid known triggers
- Wear soft, breathable fabrics like cotton
- Keep fingernails short to minimize skin injury from scratching
- Manage stress through healthy coping strategies
- Use humidifiers in dry environments, when appropriate
Early recognition and ongoing skin care are key elements of long-term management.
Conclusion
Eczema is a common, chronic inflammatory skin condition driven by a complex interaction of genetic, immune, and environmental factors. While symptoms such as itching, dryness, and inflammation can be challenging, evidence-based treatments and consistent skincare routines allow many individuals to achieve good symptom control. Understanding the nature of eczema empowers patients and caregivers to recognize triggers, seek appropriate care, and maintain healthier skin over time.
Medical Disclaimer
This article is intended for educational purposes only and does not replace professional medical evaluation or treatment. Readers are encouraged to consult a qualified healthcare professional or dermatologist for diagnosis, treatment options, and individualized medical guidance.