Hypertensive Heart Disease with Congestive Heart Failure ICD-10: A Comprehensive Guide
Introduction
Long standing hypertension can gradually remodel the heart. Over time, persistently elevated arterial pressure increases afterload, forces the left ventricle to work harder, and contributes to structural and functional changes that may progress to symptomatic heart failure. In coding terms, when hypertension and heart failure are clinically linked, ICD-10-CM uses a combination code framework rather than treating them as entirely separate problems. For clinicians, coders, and billers, this distinction matters because it affects code selection, sequencing, claim accuracy, and the clinical picture reflected in the record.
- Assign I11.0 when hypertension is linked to heart failure and add an appropriate I50 code to specify heart failure type.
- Use I13 with N18 plus I50 when chronic kidney disease is related to hypertensive heart disease and heart failure.
- Document explicitly: "hypertensive heart disease with heart failure," specify systolic versus diastolic, acuity, comorbidities, diagnostic evidence, and treatments.
This topic is especially important because hypertensive heart disease sits at the intersection of cardiology, primary care, utilization review, and revenue cycle operations. Accurate coding supports risk adjustment, quality reporting, reimbursement, and continuity of care. Equally important, good documentation improves patient management by clearly stating whether heart failure is present, what type it is, whether kidney disease is also involved, and how severe the illness has become.
Section 1: Understanding Hypertensive Heart Disease
What Happens to the Heart?
Hypertensive heart disease develops because chronic high blood pressure exposes the myocardium to sustained mechanical stress. The left ventricle must generate more force to eject blood against elevated systemic resistance. Initially, the heart adapts by thickening its muscular wall, a process called left ventricular hypertrophy. Although this may temporarily preserve pumping function, the thickened ventricle becomes stiffer and less compliant. Over time, ventricular filling worsens, diastolic dysfunction develops, and some patients later progress to systolic dysfunction, chamber dilation, and overt heart failure symptoms.
This progression is clinically important because patients may not present with heart failure immediately. Many begin with asymptomatic hypertensive remodeling, then develop exercise intolerance, dyspnea, edema, or recurrent fluid overload as ventricular function deteriorates. Therefore, documentation should not stop at “hypertension” when the chart supports hypertensive cardiac involvement. Clear recognition of the disease process improves both care planning and code assignment.
Key Risk Factors
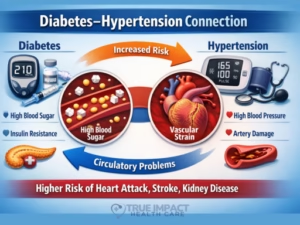
Several factors increase the likelihood that uncomplicated hypertension will progress to hypertensive heart disease and eventually congestive heart failure. Poorly controlled blood pressure over many years is the central driver, because duration and severity of pressure overload both matter. Older age increases vulnerability because myocardial stiffness, vascular disease, and comorbidity burden tend to rise with age. Obesity and metabolic syndrome worsen hemodynamic strain, insulin resistance, and inflammatory burden. Family history of cardiovascular disease may reflect inherited predisposition to hypertension, cardiomyopathy, or premature vascular disease. Sedentary behavior and a high sodium dietary pattern can further aggravate blood pressure control and volume retention.
From a documentation standpoint, these risk factors are not substitutes for diagnosis, but they do provide clinical context. When they are present alongside imaging, symptoms, and physician assessment, they help explain why hypertensive heart disease has developed and why long term preventive management remains essential.
Section 2: Congestive Heart Failure Overview
Recognizing CHF Symptoms
When hypertensive heart disease advances to congestive heart failure, patients typically develop symptoms related to elevated filling pressures, impaired forward flow, and fluid retention. Shortness of breath on exertion is often one of the earliest signs, because pulmonary venous pressure rises as the left side of the heart struggles to accommodate or eject blood effectively. Orthopnea, meaning shortness of breath while lying flat, occurs because recumbency shifts fluid back toward the chest and increases pulmonary congestion. Paroxysmal nocturnal dyspnea refers to episodes of waking from sleep gasping for air and is another classic manifestation of worsening congestion. Peripheral edema, especially in the ankles and legs, reflects systemic fluid accumulation. Fatigue and reduced exercise tolerance arise because inadequate cardiac performance limits oxygen delivery during activity.
These symptoms should be described precisely in the clinical record. General phrases such as “CHF exacerbation” are less useful than documentation that specifies exertional dyspnea, orthopnea, nocturnal symptoms, recent weight gain, edema severity, and functional decline. Detailed symptom language supports both clinical decision making and more accurate coding.
Pathophysiology in a Nutshell
The pathophysiology of congestive heart failure in this setting begins with elevated left ventricular filling pressures. As the left ventricle becomes stiff or weak, pressure backs up into the left atrium and pulmonary veins, leading to pulmonary congestion and breathlessness. If the burden persists, right sided pressures may also rise, which contributes to systemic venous congestion, edema, abdominal fullness, and jugular venous distension. At the same time, the body activates neurohormonal systems, particularly the renin angiotensin aldosterone system and the sympathetic nervous system, in an attempt to preserve blood pressure and organ perfusion. Although initially compensatory, this neurohormonal activation eventually worsens vasoconstriction, sodium retention, remodeling, and disease progression.
This is why treatment targets not only symptoms, but also the underlying neurohormonal cascade and structural remodeling. It is also why records should distinguish between acute decompensation, chronic stable disease, and acute on chronic presentations. Each reflects a different stage of pathophysiology and often supports a different heart failure code.
Section 3: ICD-10 Classification and Specific Codes
Primary ICD-10 Code
For hypertensive heart disease with heart failure, the key ICD-10-CM combination code is I11.0, Hypertensive heart disease with heart failure. Current ICD-10-CM guidance states that when hypertension is present with heart conditions classified to the heart failure category, the case is assigned to category I11 unless the provider documents that the heart condition is unrelated to hypertension. In other words, the coding system presumes a relationship between hypertension and heart failure in this context unless the clinician explicitly separates them.
That rule is highly important in daily coding practice. It means coders should not default to coding essential hypertension and heart failure separately when the record supports hypertensive heart disease. However, if the provider clearly states that the heart failure is unrelated to hypertension, then separate coding may be appropriate according to the encounter circumstances.
Additional Codes to Consider
Although I11.0 identifies hypertensive heart disease with heart failure, it does not fully describe the type of heart failure. Official guidance requires an additional code from category I50 to identify the specific heart failure condition. CMS materials list the commonly paired heart failure codes for I11.0, including I50.1 left ventricular failure, I50.21 acute systolic heart failure, I50.22 chronic systolic heart failure, I50.23 acute on chronic systolic heart failure, I50.31 acute diastolic heart failure, I50.32 chronic diastolic heart failure, I50.33 acute on chronic diastolic heart failure, I50.41 acute combined systolic and diastolic heart failure, I50.42 chronic combined systolic and diastolic heart failure, I50.43 acute on chronic combined systolic and diastolic heart failure, and other specific heart failure codes when supported by the documentation.
This is why documentation must go beyond the older phrase “congestive heart failure” whenever possible. “CHF” alone may not tell the coder whether the patient has systolic, diastolic, combined, right sided, end stage, or left ventricular failure, nor whether the episode is acute, chronic, or acute on chronic. A vague diagnosis increases the likelihood of unspecified coding and weakens claim precision.
Important Coding Nuance About Kidney Disease
One of the most common pitfalls is using I11.0 when the patient also has chronic kidney disease related to hypertension. If hypertension, heart disease, and chronic kidney disease are all present together, ICD-10-CM directs the coder to category I13, hypertensive heart and chronic kidney disease, not I11 alone. If heart failure is present in that setting, an additional I50 code is still required to identify the type of heart failure, and an N18 code is used to identify the CKD stage.
Therefore, a chart that documents hypertension, chronic diastolic heart failure, and stage 3 chronic kidney disease may not be coded correctly with I11.0 plus N18.3 alone. Instead, the coder must evaluate whether the I13 combination category applies. This is a major reason why clinicians should document kidney involvement explicitly.
Section 4: Diagnosis and Documentation Best Practices
History and Physical Examination
Accurate coding begins with strong clinical documentation. The history should include blood pressure trends, duration of hypertension, medication adherence, prior admissions for fluid overload, and current symptom burden. The physical examination should describe signs of congestion such as elevated jugular venous pressure, pulmonary crackles, hepatomegaly, peripheral edema, tachypnea, and blood pressure findings. These details help establish whether the patient has stable chronic disease, acute decompensation, or poorly controlled hypertensive heart disease requiring intensive management.
For coders, the value of this information lies in specificity. The clearer the physician’s assessment, the easier it becomes to justify the relationship between hypertension and heart failure, support the acuity designation, and identify whether further coding for renal disease, arrhythmia, or other complications is necessary.
Diagnostic Tests
Diagnostic testing provides objective support for the diagnosis. Echocardiography is central because it can show left ventricular hypertrophy, chamber enlargement, impaired relaxation, reduced or preserved ejection fraction, and other structural findings relevant to heart failure classification. BNP or NT-proBNP levels support the diagnosis of heart failure in the appropriate clinical context. Chest radiography may show cardiomegaly or pulmonary vascular congestion. Electrocardiography can reveal hypertrophy, ischemic changes, conduction abnormalities, or arrhythmias. Together, these tests help distinguish hypertensive heart disease with heart failure from other causes of dyspnea and edema.
However, test results alone do not establish the final code. The provider’s diagnostic statement still drives code assignment. That means coders should not infer hypertensive heart disease or a heart failure subtype solely from imaging unless the clinician documents it. Documentation integrity depends on clinical confirmation, not just suggestive data.
Documentation Checklist
A strong record should explicitly state “hypertensive heart disease with heart failure” or equivalent wording when that relationship is intended. It should then specify the type of heart failure, such as systolic, diastolic, combined, left ventricular, right sided, or another supported subtype. It should also state whether the episode is acute, chronic, or acute on chronic. Relevant comorbidities, such as diabetes, chronic kidney disease, obesity, dyslipidemia, atrial fibrillation, ischemic heart disease, or electrolyte abnormalities, should be documented when they affect management. Finally, the chart should capture current therapy and clinical response, for example use of diuretics, beta blockers, ACE inhibitors, ARBs, ARNIs, mineralocorticoid receptor antagonists, or other heart failure directed treatment.
This level of detail protects both clinical and coding accuracy. It reduces the risk of using unspecified codes, improves case severity capture, and clarifies whether the correct code family is I11 or I13.
Section 5: Treatment and Management Strategies
Pharmacologic Therapies
Management focuses on both blood pressure control and evidence based heart failure treatment. ACE inhibitors or ARBs reduce afterload and help limit remodeling. In current heart failure guidance, ARNI therapy may be preferred in selected patients with reduced ejection fraction. Beta blockers improve survival, reduce sympathetic overactivation, and help with rate control. Diuretics relieve symptomatic fluid overload and are especially useful in patients with edema or pulmonary congestion. Mineralocorticoid receptor antagonists provide additional neurohormonal blockade. The 2022 AHA, ACC, and HFSA guideline also highlights SGLT2 inhibitors as foundational therapy in many patients with heart failure, particularly those with reduced ejection fraction, with broader roles extending into mildly reduced and preserved ejection fraction populations.
In practical terms, medication documentation should capture both what the patient is taking and why. For example, a note stating “chronic HFrEF due to hypertensive heart disease, stable on carvedilol, sacubitril valsartan, spironolactone, furosemide, and empagliflozin” is clinically rich and coding friendly. It signals disease type, etiology, chronicity, and treatment intensity in one sentence.
Lifestyle Modification
Lifestyle measures remain indispensable. Sodium restriction helps reduce fluid retention and blood pressure burden. Daily weight monitoring can identify early fluid accumulation before symptoms worsen. Regular moderate physical activity, when medically tolerated, improves functional capacity and overall cardiovascular health. Weight reduction can improve blood pressure control, metabolic profile, and hemodynamic stress. Smoking cessation is critical because smoking accelerates vascular disease and worsens overall cardiac risk. Sleep hygiene and stress reduction also matter, especially when poor sleep or untreated sleep apnea contributes to blood pressure instability and heart failure symptoms.
These measures are not minor adjuncts. In hypertensive heart disease, long term outcome improvement depends heavily on sustained blood pressure control and self management. Patient education should therefore be documented as part of the treatment plan, not treated as an afterthought.
Advanced Interventions
Some patients will need advanced therapies beyond medication. Cardiac resynchronization therapy may benefit selected patients with systolic heart failure and electrical dyssynchrony. Implantable cardioverter defibrillators may be indicated in patients at elevated risk for malignant ventricular arrhythmias. In refractory end stage disease, referral for advanced heart failure evaluation, including ventricular assist devices or heart transplantation, may become appropriate.
For coders and documentation specialists, these interventions also signal disease severity. Their presence often indicates advanced heart failure and should prompt careful review of whether the chart supports more specific heart failure and comorbidity coding.
Section 6: Prevention and Patient Education
Early Detection
Prevention begins with identifying hypertension before structural heart disease develops. Routine blood pressure screening in primary care remains fundamental. Home blood pressure monitoring with validated devices can improve longitudinal assessment and medication titration. Regular follow up is necessary because many patients remain undertreated or nonadherent for long periods before symptoms emerge. Early intervention can delay or prevent ventricular hypertrophy, diastolic dysfunction, and overt heart failure.
This preventive framework matters even in an ICD-10 discussion because coding should reflect the disease stage accurately. A patient with uncomplicated hypertension should not be coded as hypertensive heart disease unless the record supports cardiac involvement. Good preventive care and good coding both depend on careful distinction between stages of illness.
Empowering Patients
Patients should be taught to recognize red flag symptoms. These include sudden weight gain over a short period, worsening shortness of breath, increasing ankle or abdominal swelling, reduced exercise tolerance, and worsening orthopnea or nocturnal breathlessness. Written diet guidance, fluid instructions when appropriate, medication counseling, and symptom tracking tools can improve adherence and reduce readmissions. Mobile applications, blood pressure logs, and structured heart failure management programs may further support self monitoring.
Education also improves the quality of documentation indirectly. Patients who can describe symptom changes more accurately often provide clinicians with clearer histories, which in turn allows better classification of acuity and severity in the record.
Coding Pearls and Common Pitfalls
A few coding rules deserve special emphasis. First, I11.0 is the correct combination code when hypertension and heart failure are linked and there is no hypertensive chronic kidney disease combination code required. Second, an additional I50 code should be assigned to specify the type of heart failure. Third, if the provider states the heart condition is unrelated to hypertension, then separate coding may be appropriate instead of category I11. Fourth, if chronic kidney disease is also present and related, the correct family is often I13, with an added N18 code for CKD stage and an added I50 code for heart failure type.
A frequent error is relying on I50.9 heart failure, unspecified when the chart actually supports a more precise diagnosis. Another is using I11.0 without documenting the type of heart failure. A third common error is failing to move to the I13 category when heart disease and chronic kidney disease coexist with hypertension. These mistakes can affect reimbursement, severity capture, and audit defensibility.
Conclusion
Hypertensive heart disease with congestive heart failure is more than a billing label. It represents a clinically meaningful pathway in which chronic hypertension causes structural cardiac change and eventually symptomatic failure. In ICD-10-CM, the principal combination code is I11.0 when hypertension and heart failure are linked, but that code is only part of the picture. Accurate records should also identify the specific heart failure subtype, its acuity, and any relevant renal or other comorbid involvement.
The practical takeaway is straightforward. Clinicians should document the causal relationship, heart failure type, acuity, and comorbid burden clearly. Coders should verify whether the correct family is I11 or I13 and add the required I50 code for heart failure specificity. When documentation and coding are aligned, the result is better clinical communication, cleaner claims, and a more accurate representation of disease severity.
Brief Compliance Note
Because ICD-10-CM guidance is updated periodically, coding teams should continue to verify annual CMS and NCHS updates before applying rules in live claims workflows. This article is educational and should not replace official payer policy, local coding guidance, or clinician judgment for a specific patient encounter.