Understanding Child Fever and Leg Pain: Causes, Care, and When to Seek Help
Introduction
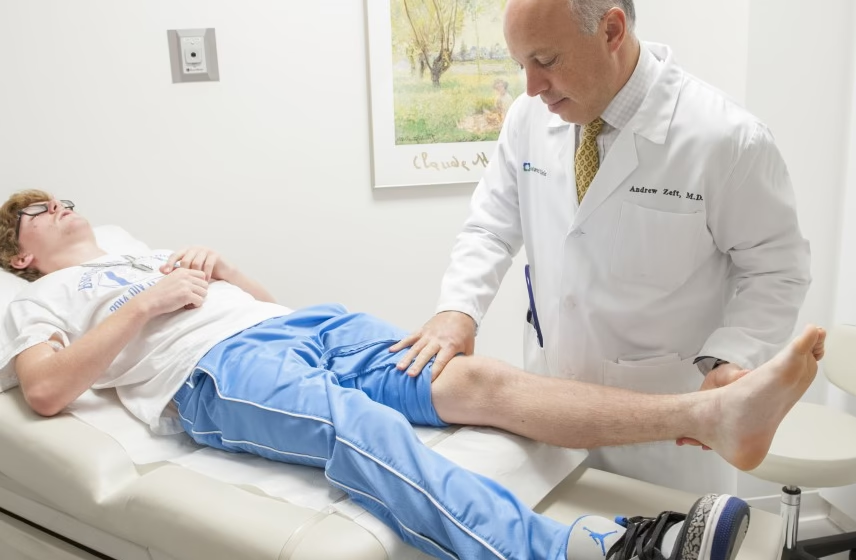
Few symptoms concern parents more than seeing a child with both fever and leg pain. Fever often signals that the body is responding to an infection or another inflammatory process, while leg pain may range from mild muscle aches to symptoms of a more serious bone, joint, or systemic illness. Although many cases are caused by common viral infections and improve with rest and fluids, fever plus leg pain should never be dismissed automatically, especially when the pain is severe, localized, associated with swelling, or causes a child to limp or refuse to bear weight. Pediatric guidance emphasizes that fever with localized musculoskeletal pain or refusal to walk should raise concern for conditions such as osteomyelitis or septic arthritis, which need prompt medical assessment.
- Immediate medical review for intense localized limb pain with swelling, warmth, severe pain, lethargy, dehydration, stiff neck, rash, or inability to use the limb.
- At home, ensure hydration, use age and weight based acetaminophen or ibuprofen for comfort, promote rest, gentle movement, and warm or cool compresses.
- Contact a clinician if fever persists beyond 72 to 96 hours, leg pain worsens, walking remains limited, or the child is immunocompromised or chronically ill.
- Prevention: keep vaccinations current, support bone health with nutrition and vitamin D, encourage regular activity, sleep hygiene, and proper supportive footwear.
This article explains the common causes in full, how to interpret symptom patterns, what parents can do at home for milder cases, and which warning signs mean a child should be seen urgently.
Common Causes of Fever and Leg Pain in Children
Viral Infections
Viral infections are among the most common reasons children develop fever and generalized aches. Illnesses such as influenza and other respiratory viruses can cause diffuse muscle soreness, including pain in the thighs, calves, or shins. In these situations, the leg pain is usually part of a broader “body aches” pattern rather than a single painful joint or one sharply localized area. Some viruses can also produce joint discomfort or temporary inflammation, which may make a child complain of knee, ankle, or leg pain during the illness. Because viral symptoms often improve gradually over several days, the leg pain in this setting is usually mild to moderate and improves as the fever resolves. However, viral illness does not completely rule out more serious causes, so the overall pattern still matters.
Growth Pains
Growth pains are common in preschool and school aged children and typically cause aching in both legs, especially in the calves, shins, or behind the knees. They are more likely to happen in the evening or at night and usually do not cause swelling, redness, limping, or pain during daytime activity. Importantly, classic growing pains are not usually associated with high fever. If a child has leg pain plus a high temperature, pain in one leg, pain in the morning, limping, or pain bad enough to stop walking, that pattern is less consistent with ordinary growing pains and deserves medical review. The NHS specifically advises assessment when leg pain is in one leg, occurs with walking, is associated with a high temperature, or is accompanied by swelling, rash, tiredness, or weight loss.
Post Vaccination Reactions
After routine immunizations, some children develop a low grade fever and soreness in the leg if the vaccine was given in the thigh. This is usually a short lived inflammatory response to the injection itself and tends to improve within 24 to 48 hours. The pain is generally localized to the injection site, not deep in the bone or joint, and the child usually remains able to move the leg, even if they are somewhat uncomfortable. If the pain becomes severe, spreading, increasingly swollen, or lasts beyond the expected short recovery window, the child should be evaluated because that pattern suggests something other than a routine vaccine reaction.
Inflammatory and Autoimmune Conditions
Some inflammatory conditions can also produce fever and leg or joint pain. Rheumatic fever, for example, can cause high temperature along with painful, swollen joints, often affecting larger joints such as the knees, ankles, wrists, or elbows. Juvenile inflammatory disorders may also cause ongoing pain, stiffness, swelling, fatigue, or rash. These causes are less common than viral illness, but they become more important when symptoms persist, recur, or involve swollen joints, morning stiffness, or other systemic features rather than short lived muscle aches.
Serious Infections
The most important causes to exclude are serious bone or joint infections such as osteomyelitis and septic arthritis. Pediatric sources emphasize that these should be considered in any child with fever and limb pain, especially when the pain is localized, the limb is swollen or red, the child has reduced range of motion, or refuses to bear weight. Osteomyelitis is an infection of the bone and often causes focal pain and fever. Septic arthritis is an infection inside a joint and can cause intense pain, warmth, swelling, and marked difficulty moving the joint. These conditions can worsen quickly and usually require urgent treatment.
Recognizing Symptoms and Warning Signs
Fever Details
The fever pattern gives useful clues. A low grade fever may fit with a mild viral illness or a short term post vaccination reaction. A higher fever, especially above 39°C or 102.2°F, raises concern for more significant infection or inflammation. Duration matters as well. Fever that continues beyond several days without improvement should not be ignored. NHS child fever guidance advises medical review for persistent fever, including temperatures of 38°C or above lasting more than five days.
Leg Pain Characteristics
The nature of the leg pain is just as important as the fever. Muscle type pain often feels more diffuse and may involve both legs. Joint pain tends to be more localized, often in the knee or ankle, and may be associated with swelling or reduced movement. Pain that is mild and improves with rest is less concerning than pain that is intense, clearly localized, wakes the child repeatedly, or makes walking difficult. Refusal to bear weight is a particularly important warning sign because it may indicate septic arthritis, osteomyelitis, or another urgent condition.
Red Flags That Warrant Immediate Attention
Some symptom combinations require prompt medical evaluation rather than home observation. These include:
- intense, localized pain with swelling, warmth, or redness
- refusal to walk or inability to put weight on the leg
- severe pain not improving with pain relief
- swelling of a limb or joint
- lethargy, confusion, or unusual drowsiness
- dehydration signs such as dry mouth and reduced urination
- stiff neck, severe headache, or a rash, especially if the child seems seriously unwell
Child fever guidance from NHS sources highlights swelling of a limb or joint, inability to use or bear weight on a limb, severe pain, dehydration, and signs of serious illness as reasons to seek urgent help. Meningitis guidance also stresses not waiting for every symptom to appear before getting help if a child seems seriously ill.
At Home Care and Comfort Measures
Keep Your Child Hydrated
Fever increases fluid loss, and children who feel unwell may drink less than usual. Offering water, oral rehydration fluids, clear soups, or other tolerated fluids helps reduce the risk of dehydration. Small, frequent sips are often easier than asking a child to drink a large amount at once. Hydration matters because dehydration can worsen fatigue, irritability, and headache, and it is also one of the warning features clinicians watch for in febrile children.
Control Fever Safely
For many children, weight based doses of acetaminophen or ibuprofen can reduce fever and ease associated aches. This can make the child more comfortable and help them drink, rest, and move more easily. However, fever medicine does not treat the underlying cause, so it should be viewed as symptom relief rather than a substitute for medical assessment when red flags are present. Parents should follow age and weight based instructions carefully and seek professional advice if unsure.
Promote Rest and Gentle Movement
Rest supports recovery, especially when the cause is viral. However, complete immobility is not always necessary for mild muscle aches. If the child is comfortable, gentle movement and light walking may prevent stiffness. The key is to follow the child’s tolerance. A child who is willing to move a little and improves with rest is different from a child who refuses to stand because of pain. Persistent inability to walk is not something to manage at home without guidance.
Warm or Cold Compresses
Warmth can help relax tight muscles, while a cool pack may reduce localized inflammation around a sore joint or injection site. Compresses should be gentle and not applied directly to bare skin for long periods. These measures may improve comfort, but if swelling, redness, and severe pain are present, parents should not assume that home treatment is enough because those features can occur with bone or joint infection.
Gentle Massage and Stretching
When the pain pattern fits benign muscle aching or growth pains, gentle massage of the calves or thighs can be soothing. Mild stretching may also help. However, massage should not be used on an acutely swollen, red, or intensely painful area, because that type of presentation may indicate infection or significant inflammation and should be medically assessed instead.
When to Seek Medical Attention
Parents should contact a clinician if the fever persists beyond roughly 72 to 96 hours, if the leg pain is getting worse rather than better, or if walking remains limited after a short period of home care. Medical review is especially important when the child has a weakened immune system, chronic illness, or sudden severe pain after injury. Official pediatric and NHS guidance also supports urgent assessment when a child has fever plus localized limb pain, joint swelling, severe pain, refusal to bear weight, or signs of serious illness.
A clinician may perform a physical examination and, depending on the findings, order blood tests or imaging such as X rays, ultrasound, or other studies. This is particularly important when trying to rule out osteomyelitis, septic arthritis, or inflammatory joint disease.
Preventive Tips and Healthy Habits
Keep Vaccinations Up to Date
Vaccination reduces the risk of several infections that can cause fever and more serious complications in children. Although mild post vaccine soreness can happen, the long term preventive benefit is substantial.
Support Bone and Muscle Health With Nutrition
A balanced diet that includes adequate protein, calcium, and vitamin D supports growing bones and muscles. Good nutrition does not prevent every cause of leg pain, but it helps maintain musculoskeletal health and recovery capacity.
Encourage Regular Activity and Stretching
Children benefit from regular movement, which supports muscle strength, coordination, and flexibility. Gentle stretching can also help reduce routine muscle tightness.
Maintain Good Sleep Habits
Sleep is important for immune function, recovery, and growth. A child who is sleep deprived may feel worse during illness and recover more slowly.
Use Proper Footwear
Supportive shoes can reduce strain on growing legs and feet, particularly in active children. While footwear will not prevent infectious causes of pain, it can reduce some mechanical discomfort and overuse related aches.
Conclusion
Child fever with leg pain is often caused by common and self limited illnesses, especially viral infections, but it can also signal more serious conditions that should not be missed. The most important distinction is between mild, generalized aches that improve with rest and fluids, and more concerning patterns such as localized pain, swelling, high fever, limping, or refusal to bear weight. Serious bone and joint infections remain key diagnoses to exclude in a child with fever and limb pain.
Parents can usually help with hydration, fever relief, rest, and comfort measures in mild cases. However, if symptoms intensify, fever lasts several days, the child cannot walk, or red flag features appear, medical evaluation should be sought promptly. Early assessment improves the chance of timely treatment and better outcomes.