Introduction
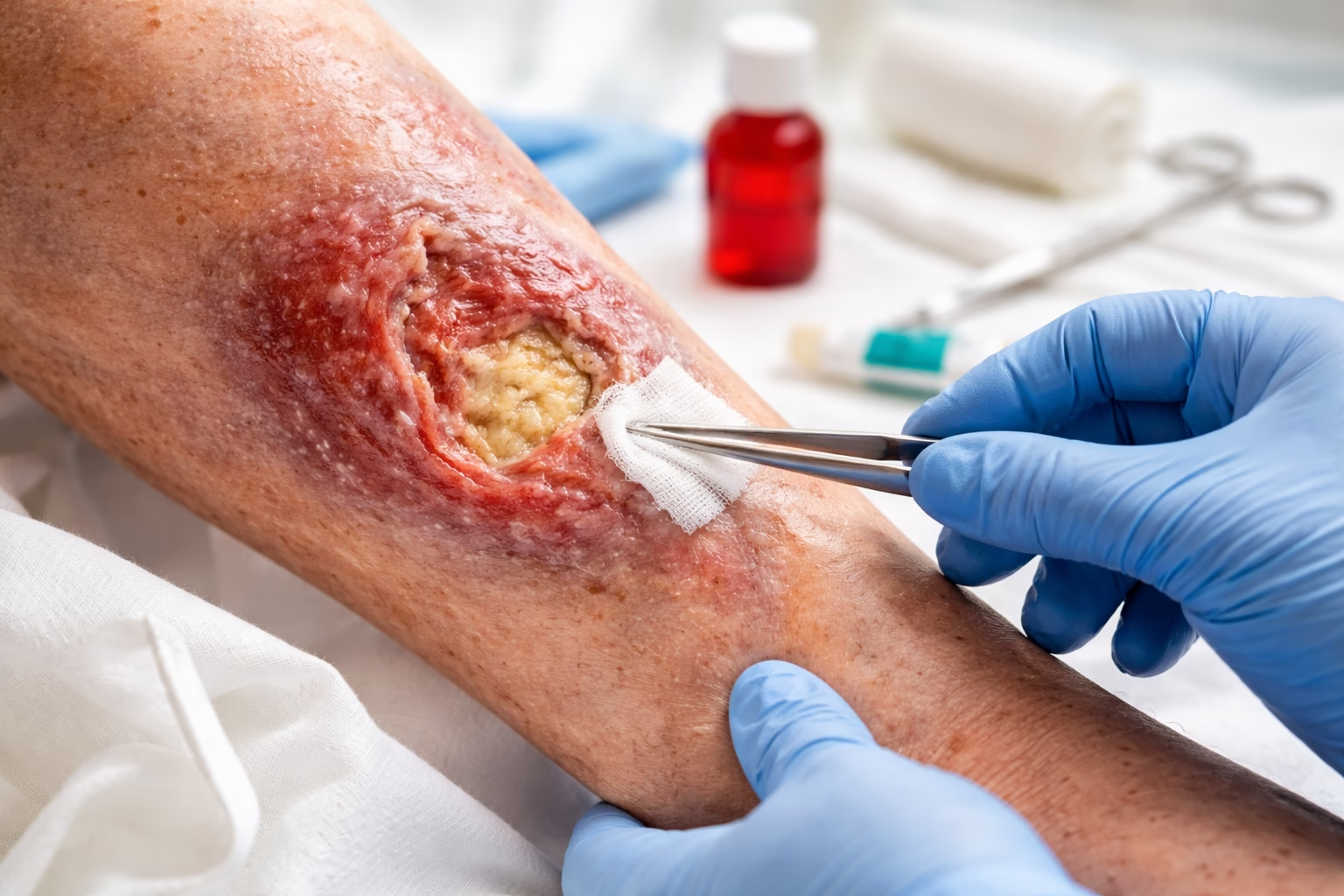
Chronic or non-healing wounds can be a source of frustration, discomfort, and even serious health risks. Whether you’re dealing with a diabetic ulcer, a pressure sore, or a surgical incision that simply refuses to close, slow-healing wounds require a targeted approach.
- Identify and address underlying barriers to healing such as poor circulation, infection, diabetes, pressure, nutritional deficits, and medication effects.
- If a wound shows no notable improvement within two weeks obtain a healthcare evaluation for size measurement, infection testing, and blood flow assessment.
- Prepare the wound using TIME: debride necrotic tissue, control infection, maintain moist balance, and manage wound edges to encourage healing.
- When conventional care stalls consider specialist therapies like negative pressure, hyperbaric oxygen, growth factors, or bioengineered skin substitutes.
- Optimize healing with adequate protein and vitamins, glucose control, pressure offloading, smoking cessation, and exercise; seek urgent care for spreading infection or exposed bone.
In this post, we’ll explore why some wounds stall in the healing process and provide practical, evidence-based steps to help get them back on track.
Understanding Why Wounds Don’t Heal
Before diving into treatment strategies, it’s essential to identify the underlying factors that impede healing:
-
Poor circulation: Reduced blood flow means less oxygen and fewer nutrients reach the wound.
-
Infection: Bacterial colonization delays tissue regeneration and can cause secondary complications.
-
Diabetes and metabolic disorders: High blood sugar damages small blood vessels and impairs immune function.
-
Pressure and friction: Constant rubbing or pressure—common in bedridden patients—can reopen or worsen wounds.
-
Nutritional deficiencies: Inadequate protein, vitamins (especially C and A), and minerals (zinc, iron) undermine tissue repair.
-
Medications and systemic diseases: Steroids, chemotherapy, or autoimmune conditions may slow down the body’s natural healing response.
Initial Assessment and Professional Evaluation
If a wound hasn’t shown noticeable improvement in two weeks, arrange for a healthcare evaluation. A clinician can:
-
Measure wound size, depth, and appearance
-
Test for infection (swabs or biopsies)
-
Assess blood flow with Doppler ultrasound or ankle-brachial index (ABI)
-
Review your medical history, medications, and lifestyle factors
Early assessment helps prevent complications and ensures the right treatment plan is started promptly.
Core Principles of Wound Bed Preparation (TIME Framework)
A systematic approach known as TIME can guide effective wound care.
T: Tissue Management
-
Debride necrotic (dead) tissue using sharp, mechanical, enzymatic, or autolytic methods
-
Remove slough to expose healthy granulation tissue
I: Infection and Inflammation Control
-
Use topical or systemic antibiotics if infection is confirmed
-
Consider antiseptic dressings (e.g., iodine or silver-impregnated) for colonized wounds
M: Moisture Balance
-
Maintain a moist (not wet) environment to promote cell migration
-
Choose dressings that match wound exudate levels:
-
Hydrocolloids for light exudate
-
Foams for moderate exudate
-
Alginates for heavy drainage
-
E: Edge of Wound Advancement
-
Evaluate and treat rolled or calloused wound edges (epibole)
-
Encourage epithelial migration with shear reduction and protective dressings
Advanced Therapies for Stubborn Wounds
When conventional care stalls, consider these evidence-based interventions under professional guidance:
Negative Pressure Wound Therapy (NPWT)
-
Applies controlled suction to draw out fluid
-
Reduces swelling
-
Stimulates granulation tissue formation
Hyperbaric Oxygen Therapy (HBOT)
-
Involves breathing 100% oxygen in a pressurized chamber
-
Enhances tissue oxygenation and supports healing
Growth Factors and Bio-Engineered Skin Substitutes
-
Topical recombinant growth factors (e.g., PDGF)
-
Cultured skin equivalents that help jump-start healing
Electrical and Ultrasound Stimulation
-
Low-level electrical currents
-
Therapeutic ultrasound to promote cell proliferation
Holistic Support: Nutrition, Lifestyle, and Prevention
A healing wound needs more than dressings—it requires a healthy internal environment.
Nutrition Tips
-
Protein: Aim for 1.2–1.5 g/kg body weight per day
-
Vitamin C: 75–90 mg daily
-
Vitamin A: 700–900 µg daily
-
Zinc: 8–11 mg daily
-
Iron: Especially important if anemia is present
Blood Sugar Control
-
Monitor glucose levels regularly if diabetic
-
Follow your healthcare provider’s medication and diet plan carefully
Pressure Relief and Offloading
-
Use specialized mattresses or cushions for pressure ulcers
-
Change position every two hours if bedridden
Smoking Cessation and Exercise
-
Smoking constricts blood vessels and delays healing
-
Gentle exercise boosts circulation and overall health
When to Seek Immediate Medical Attention
Not every non-healing wound can be managed at home. Contact your healthcare provider immediately if you notice:
-
Signs of spreading infection (red streaks, increasing pain, fever)
-
Sudden increase in wound size or depth
-
Exposed bone, tendon, or surgical hardware
-
Foul odor or excessive purulent discharge
Prompt action can prevent serious complications such as sepsis or limb-threatening infections.
Conclusion
Wounds that won’t heal demand a comprehensive, methodical approach: assess, clean, protect, and nourish both the wound and your body. By addressing underlying causes—whether poor circulation, infection, or nutritional gaps—and leveraging advanced therapies when necessary, you can give your body the tools it needs to close the gap on stubborn wounds.
Collaboration with a qualified healthcare professional is key to developing a personalized care plan. With diligence, appropriate treatment, and healthy lifestyle adjustments, many chronic wounds can make meaningful progress toward full recovery.