Introduction
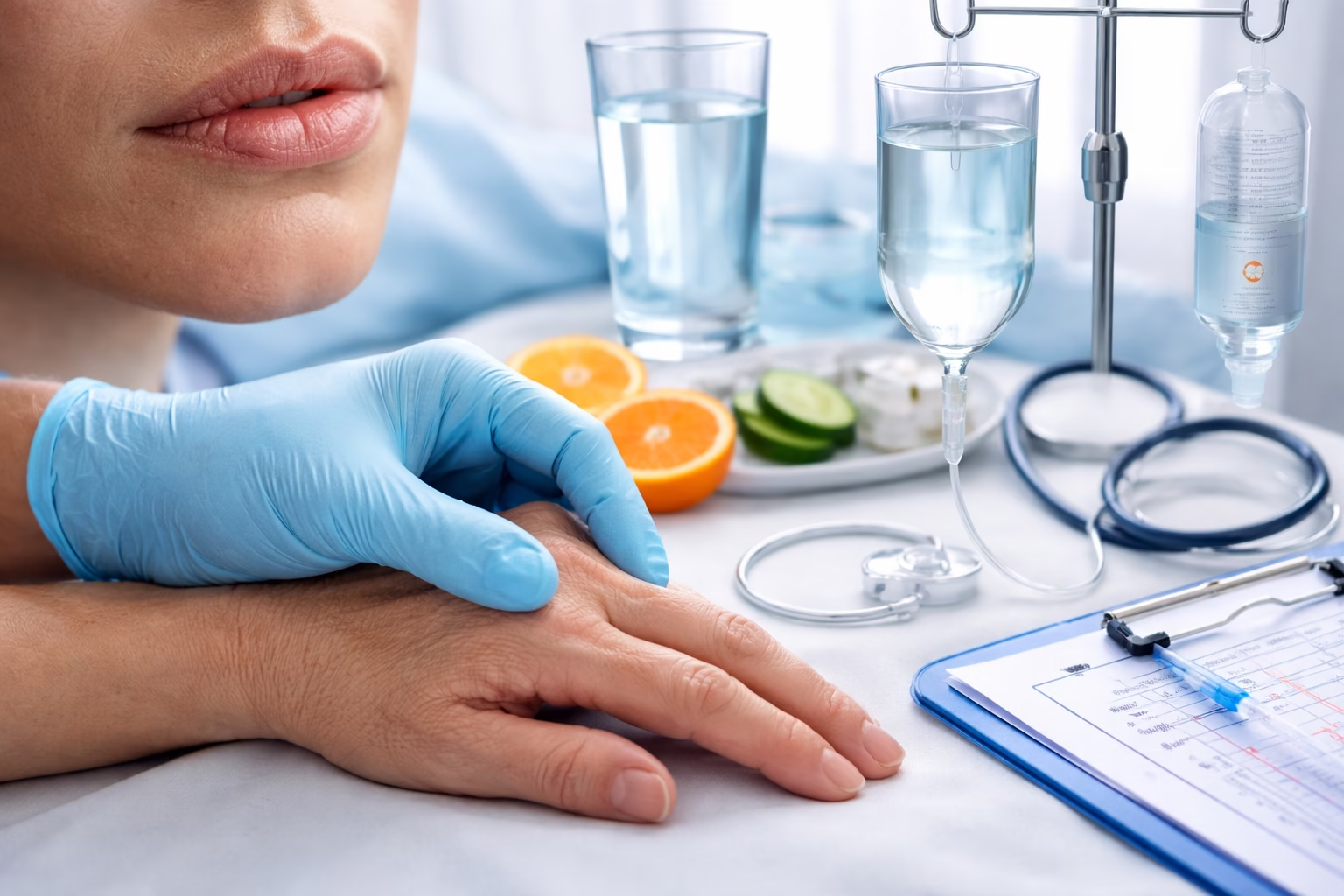
Every cell, tissue, and organ in our body relies on water to function optimally. When fluid losses exceed intake, or when the body can’t properly retain fluids, dehydration sets in. Clinically, dehydration ranges from a mild nuisance (headache, dry mouth) to a life‐threatening emergency (hypovolemic shock). Understanding how dehydration is recognized and treated not only helps healthcare providers intervene quickly but also empowers patients and caregivers to take preventive steps.
- Recognize dehydration severity using history, physical exam, vital signs, urine output, skin turgor, capillary refill, and labs like BUN/creatinine and electrolytes.
- Treat mild to moderate cases with standardized oral rehydration solutions, small frequent sips, and continue infant feeds; switch to IV if intolerant or severe.
- Use IV crystalloids for moderate to severe dehydration, calculate and replace fluid deficit, monitor intake/output and electrolytes, and adjust for age/comorbidities.
In this post, we’ll explore:
• The fundamental causes and risk factors behind dehydration
• How clinicians recognize its signs and severity
• Evidence‐based treatment strategies, from oral rehydration to IV fluids
• Prevention tips to stay ahead of fluid loss
Let’s dive into the science and the practical steps, that help keep dehydration at bay.
Section 1: What Is Dehydration?
Dehydration occurs when water and key electrolytes (sodium, potassium, chloride) are lost faster than they’re replaced. Clinically, we categorize dehydration by fluid deficit and electrolyte imbalance:
- Isotonic dehydration: Equal loss of water and sodium
- Hypertonic dehydration: Greater water loss vs. sodium (often seen in fever or diabetes insipidus)
- Hypotonic dehydration: Greater sodium loss vs. water (e.g., prolonged vomiting, diuretics)
Risk Factors
• Infants and young children (higher metabolic rate, limited communication)
• Elderly patients (diminished thirst perception, medication side effects)
• Athletes exercising in high heat
• Patients with gastrointestinal losses (vomiting, diarrhea)
• Chronic illnesses (renal disease, uncontrolled diabetes)
Section 2: Recognizing Dehydration Clinically
Early recognition is key. Clinicians use a combination of patient history, physical exam, and laboratory tests to gauge severity.
2.1 Key Signs and Symptoms
Mild to Moderate Dehydration
• Thirst, dry or sticky mouth
• Reduced urine output; darker urine color
• Fatigue, lightheadedness
• Slight drop in blood pressure when standing (orthostatic hypotension)
Severe Dehydration
• Extreme thirst, confusion, irritability
• Rapid heartbeat (tachycardia) and low blood pressure (hypotension)
• Skin tenting (poor skin turgor)
• Sunken eyes and fontanelle (in infants)
• Oliguria or anuria (very low to no urine output)
2.2 Objective Measurements
• Vital signs: heart rate, blood pressure, respiratory rate
• Mucous membranes: dry, cracked lips; sunken eyes
• Capillary refill time: delayed (>2 seconds)
• Laboratory values:
– Elevated blood urea nitrogen (BUN)/creatinine ratio (>20:1)
– Increased hematocrit (hemoconcentration)
– Electrolyte disturbances (e.g., hypernatremia in hypertonic dehydration)
Section 3: Clinical Treatment Strategies
Treatment hinges on dehydration severity, underlying cause, and patient age/comorbidities.
3.1 Oral Rehydration Therapy (ORT)
First‐line for mild to moderate dehydration, especially in children and adults who can drink:
• Use standardized oral rehydration solutions (ORS) containing glucose and electrolytes
• Encourage small, frequent sips (e.g., 5–10 mL every few minutes)
• Monitor for vomiting; if persistent, switch to IV fluids
• Continue feeding in infants—do not withhold breastmilk or formula
3.2 Intravenous (IV) Fluid Replacement
Reserved for moderate to severe dehydration or patients unable to tolerate ORT:
Crystalloid Solutions
• Normal saline (0.9% NaCl): expands extracellular fluid volume
• Lactated Ringer’s: contains sodium, potassium, calcium, and lactate (acts as a buffer)
Replacement Strategy
- Calculate fluid deficit:
Fluid deficit (%) × body weight (kg) × 1,000 (mL) - Replace half of the deficit in the first 8 hours; the remainder over the next 16 hours
- Add maintenance fluids and ongoing losses
3.3 Monitoring and Adjustments
• Track intake/output hourly
• Reassess vital signs every 1–2 hours initially
• Reevaluate labs (electrolytes, BUN/creatinine) after 6–8 hours of therapy
• Adjust fluid type and rate based on ongoing assessment
Section 4: Special Considerations
4.1 Pediatric Patients
• Use weight‐based dosing for ORS and IV fluids
• Watch for rapid changes in status—infants can deteriorate quickly
• Encourage breastfeeding; avoid untested homemade solutions
4.2 Elderly Patients
• Consider comorbidities (heart failure, renal impairment) when prescribing fluids
• Monitor for fluid overload (edema, pulmonary crackles)
• Review medications that may exacerbate dehydration (diuretics, laxatives)
4.3 Chronic Illnesses
• Diabetes mellitus: monitor glucose levels to avoid hyperglycemia with ORS
• Renal disease: adjust electrolyte content, avoid potassium overload
• Heart failure: restrict sodium, carefully balance fluid removal versus repletion
Section 5: Prevention Strategies
Preventive measures help reduce hospital admissions and improve quality of life:
• Maintain regular fluid intake: aim for 1.5–2 liters/day for adults (adjust for climate, activity)
• Choose water, herbal teas, or ORS during illness or heavy exercise
• Educate high‐risk groups on early signs of dehydration
• Monitor urine color (pale straw‐yellow is ideal)
• Limit excessive caffeine/alcohol, which can be diuretic
Conclusion
Recognizing and treating dehydration promptly is vital to prevent complications ranging from acute kidney injury to shock. Clinicians rely on a combination of history, physical exam, and labs to determine severity—and then tailor treatment from oral rehydration solutions to intravenous fluids. By staying vigilant, educating patients, and applying evidence‐based protocols, healthcare providers can effectively restore fluid balance and protect vulnerable populations.
Remember: prevention is often the best medicine. Encouraging regular hydration habits and awareness of early warning signs can keep dehydration from ever becoming a clinical emergency. Stay hydrated, stay healthy!