Psoriasis: Understanding the Causes, Symptoms, and Treatment Options
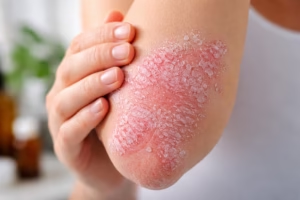
Psoriasis is more than just a skin condition, it is a chronic, immune-mediated disease that can affect a person’s physical health, emotional well-being, and quality of life. Characterized by red, scaly patches on the skin, psoriasis is common, affecting millions of people worldwide. Although it is a long-term condition, advances in medical research have made effective treatment and symptom control more achievable than ever.
In this article, we will explore what psoriasis is, what causes it, how it is diagnosed, and the various treatment and lifestyle strategies available to manage it.
Overview: What Is Psoriasis?
Psoriasis is a chronic inflammatory autoimmune condition that primarily affects the skin. It occurs when the immune system mistakenly speeds up the life cycle of skin cells. Instead of maturing and shedding over a normal 28–30 day period, new skin cells rise to the surface in just a few days. This rapid buildup leads to thick, scaly plaques.
Common Types of Psoriasis
There are several types of psoriasis, including:
- Plaque psoriasis (most common): Raised, red patches covered with silvery-white scales
- Guttate psoriasis: Small, drop-shaped spots, often triggered by infections
- Inverse psoriasis: Smooth, red patches in skin folds (e.g., underarms, groin)
- Pustular psoriasis: White pustules surrounded by red skin
- Erythrodermic psoriasis: A rare but severe form causing widespread redness and scaling
In some individuals, psoriasis is also associated with psoriatic arthritis, which causes joint pain, stiffness, and swelling.
Causes and Risk Factors
Psoriasis is considered an immune-mediated disease influenced by genetic and environmental factors.
Immune System Involvement
In people with psoriasis:
- The immune system becomes overactive.
- T cells (a type of white blood cell) mistakenly attack healthy skin cells.
- This triggers inflammation and rapid skin cell production.
Genetic Factors
- Psoriasis tends to run in families.
- Having a close relative with psoriasis increases your risk.
- Multiple genes are believed to contribute, though no single gene causes the condition.
Common Triggers
While psoriasis is not contagious, certain factors can trigger or worsen flare-ups:
- Emotional stress
- Skin injuries (cuts, burns, insect bites)
- Infections (e.g., strep throat)
- Cold, dry weather
- Smoking
- Heavy alcohol consumption
- Certain medications (e.g., lithium, beta-blockers)
Identifying and managing individual triggers is an important component of disease control.
Symptoms and Clinical Presentation
Symptoms vary depending on the type and severity of psoriasis.
Typical Skin Symptoms
- Red, inflamed patches of skin
- Thickened plaques with silvery scales
- Dry, cracked skin that may bleed
- Itching, burning, or soreness
- Nail changes (pitting, discoloration, or separation from nail bed)
Psoriatic Arthritis Symptoms
Up to 30% of people with psoriasis develop psoriatic arthritis. Symptoms may include:
- Joint pain and stiffness
- Swelling in fingers and toes
- Reduced range of motion
- Morning stiffness lasting more than 30 minutes
Because psoriasis is a systemic inflammatory condition, it is also associated with an increased risk of:
- Cardiovascular disease
- Obesity
- Type 2 diabetes
- Depression and anxiety
Diagnosis and Screening
Psoriasis is typically diagnosed through a clinical examination by a healthcare professional.
Diagnostic Process
- Review of medical and family history
- Visual inspection of skin, scalp, and nails
- Examination of joints if arthritis is suspected
In unclear cases, a skin biopsy may be performed to confirm the diagnosis and rule out other conditions.
If psoriatic arthritis is suspected, additional tests such as imaging (X-rays or MRI) and blood tests may be used to assess joint involvement and exclude other types of arthritis.
Treatment and Management Options
While there is currently no cure for psoriasis, many treatments are effective in reducing symptoms and preventing flare-ups. Treatment choice depends on:
- Severity of disease
- Areas of skin involved
- Presence of psoriatic arthritis
- Patient preferences and overall health
1. Topical Treatments (Mild to Moderate Psoriasis)
- Corticosteroids (reduce inflammation)
- Vitamin D analogs
- Retinoids
- Calcineurin inhibitors (for sensitive areas)
- Coal tar or salicylic acid preparations
2. Phototherapy
- Controlled exposure to ultraviolet (UV) light under medical supervision
- Slows rapid skin cell growth
- Often used for moderate psoriasis
3. Systemic Medications (Moderate to Severe Psoriasis)
Oral or injectable medications that work throughout the body:
- Methotrexate
- Cyclosporine
- Oral retinoids
4. Biologic Therapies
Biologics are targeted medications that block specific parts of the immune system. They are often used for moderate to severe psoriasis and psoriatic arthritis. Examples include:
- TNF-alpha inhibitors
- IL-17 inhibitors
- IL-23 inhibitors
- IL-12/23 inhibitors
These treatments have significantly improved long-term disease management but require medical monitoring.
Prevention and Lifestyle Considerations
Although psoriasis cannot be completely prevented, certain strategies can help reduce flare-ups and improve overall health.
Skin Care Tips
- Moisturize daily to reduce dryness and scaling
- Avoid harsh soaps and hot showers
- Use gentle, fragrance-free products
Lifestyle Modifications
- Manage stress through relaxation techniques or counseling
- Maintain a healthy weight
- Engage in regular physical activity
- Avoid smoking
- Limit alcohol intake
Infection Prevention
Prompt treatment of infections, particularly strep throat, may help reduce the risk of certain psoriasis flares.
A comprehensive care approach often includes collaboration between dermatologists, rheumatologists, and primary care providers.
Conclusion
Psoriasis is a chronic, immune-mediated condition that affects more than just the skin. It can vary from mild to severe and may involve the joints and other aspects of overall health. While there is no cure, modern therapies—including topical treatments, phototherapy, systemic medications, and biologics—offer effective ways to manage symptoms and improve quality of life.
Understanding triggers, maintaining healthy lifestyle habits, and working closely with healthcare professionals are key components of successful long-term management.
Disclaimer:
This article is intended for educational purposes only and does not replace professional medical advice. If you have symptoms of psoriasis or concerns about your skin or joint health, consult a qualified healthcare professional for proper evaluation and individualized treatment recommendations.






