Plaque Psoriasis: Understanding Symptoms, Causes, and Treatment Options
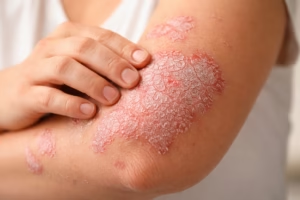
Plaque psoriasis is a common, chronic autoimmune skin condition that affects millions of people worldwide. It is more than just a cosmetic issue, it’s a medical condition that can significantly impact physical comfort, emotional well-being, and overall quality of life. Fortunately, with proper diagnosis and management, many people can effectively control symptoms and reduce flare-ups.
In this article, we’ll explore what plaque psoriasis is, its causes, symptoms, diagnosis methods, treatment options, and lifestyle considerations.
Overview: What Is Plaque Psoriasis?
Plaque psoriasis is the most common form of psoriasis, accounting for approximately 80–90% of all cases. It is a chronic inflammatory condition in which the immune system mistakenly accelerates the skin cell life cycle.
Normally, skin cells are replaced every 28–30 days. In plaque psoriasis, this process speeds up dramatically, sometimes to just 3–4 days. As a result, skin cells accumulate on the surface, forming thick, raised patches known as plaques.
These plaques are typically:
- Red or inflamed
- Covered with silvery-white scales
- Well-defined and raised
- Often itchy, painful, or tender
Plaque psoriasis is not contagious and cannot be spread through physical contact.
Causes and Risk Factors
The exact cause of plaque psoriasis is not fully understood, but it involves a complex interaction between genetic and immune system factors.
1. Immune System Dysfunction
In psoriasis, T-cells (a type of white blood cell) mistakenly attack healthy skin cells. This triggers inflammation and rapid skin cell production.
2. Genetic Factors
- Up to one-third of people with psoriasis have a family history of the condition.
- Specific genetic markers are associated with increased risk.
3. Environmental Triggers
Common triggers that may cause flare-ups include:
- Stress
- Infections (such as strep throat)
- Skin injuries (cuts, burns, sunburn)
- Certain medications (e.g., lithium, beta-blockers)
- Cold or dry weather
- Smoking and heavy alcohol use
Having risk factors does not guarantee development of psoriasis, but they may increase susceptibility.
Symptoms and Clinical Presentation
Plaque psoriasis can appear anywhere on the body, but most commonly affects:
- Elbows
- Knees
- Scalp
- Lower back
Common Symptoms
- Thick, red patches of skin
- Silvery or white scaling
- Itching or burning sensation
- Cracked, dry skin that may bleed
- Thickened or ridged nails (nail psoriasis)
Severity Levels
Psoriasis may be classified as:
- Mild: Covers less than 3% of body surface area
- Moderate: Covers 3–10%
- Severe: Covers more than 10% or significantly impacts quality of life
In some individuals, plaque psoriasis is associated with psoriatic arthritis, which causes joint pain, stiffness, and swelling.
Diagnosis and Evaluation
Plaque psoriasis is typically diagnosed through:
1. Clinical Examination
A healthcare provider examines the skin, scalp, and nails for characteristic plaques.
2. Medical History
Questions may include:
- Family history of psoriasis
- Onset and duration of symptoms
- Presence of joint pain
3. Skin Biopsy (Rarely Needed)
In uncertain cases, a small sample of skin may be examined under a microscope to confirm the diagnosis.
There is currently no routine screening test for psoriasis. Early diagnosis is important to prevent complications and improve quality of life.
Treatment and Management Options
While there is no cure for plaque psoriasis, many effective treatments can control symptoms and reduce flare-ups. Treatment depends on severity, location, and individual response.
1. Topical Treatments (Mild to Moderate Cases)
Applied directly to the skin:
- Corticosteroids (reduce inflammation)
- Vitamin D analogues (slow skin cell growth)
- Retinoids
- Coal tar
- Salicylic acid (helps remove scales)
2. Phototherapy
Controlled exposure to ultraviolet (UV) light under medical supervision can slow excessive skin cell production.
3. Systemic Medications (Moderate to Severe Cases)
Oral or injectable treatments that affect the entire body:
- Methotrexate
- Cyclosporine
- Oral retinoids
- Biologic therapies (target specific immune pathways, such as TNF-alpha or interleukin inhibitors)
Biologic medications have significantly improved outcomes for many patients with moderate to severe disease.
4. Management of Psoriatic Arthritis
If joint symptoms are present, additional medications may be prescribed to control inflammation and prevent joint damage.
Prevention and Lifestyle Considerations
Although psoriasis cannot be completely prevented, certain lifestyle strategies may help reduce flare-ups and improve symptom control.
Helpful Self-Care Measures
- Moisturize daily to prevent dryness
- Manage stress through relaxation techniques (e.g., meditation, yoga)
- Avoid skin injuries
- Limit alcohol consumption
- Quit smoking
- Maintain a healthy weight
When to Seek Medical Care
Consult a healthcare professional if:
- Skin lesions are worsening or spreading
- Joint pain develops
- Symptoms interfere with daily life
- Current treatments are not effective
Early and consistent management improves long-term outcomes.
Living With Plaque Psoriasis
Plaque psoriasis is a lifelong condition characterized by periods of remission and flare-ups. Beyond physical symptoms, it can impact emotional and psychological health. Support from healthcare providers, patient support groups, and mental health professionals can be beneficial.
Modern therapies offer substantial relief, and many individuals achieve significant skin clearance and improved quality of life with appropriate treatment.
Conclusion
Plaque psoriasis is a chronic autoimmune condition that causes red, scaly skin plaques due to accelerated skin cell turnover. While the condition cannot be cured, it can be effectively managed with topical treatments, phototherapy, systemic medications, and healthy lifestyle choices. Early diagnosis and individualized treatment are key to minimizing symptoms and preventing complications such as psoriatic arthritis.
If you suspect you may have plaque psoriasis or are experiencing worsening symptoms, consult a qualified healthcare professional for proper evaluation and treatment guidance.
Disclaimer: This article is intended for educational purposes only and should not be considered medical advice. Always seek the advice of a licensed healthcare provider for diagnosis and treatment of any medical condition.