Peyronie’s Disease: Causes, Symptoms, Diagnosis, and Treatment Options
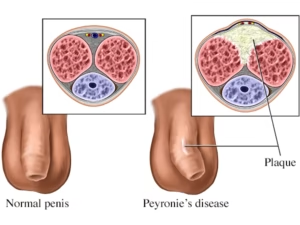
Peyronie’s disease is a condition that affects the structure of the penis, often leading to abnormal curvature, discomfort, and emotional distress. Although it is not life-threatening, it can significantly impact sexual health, confidence, and relationships. Despite being more common than many people realize, Peyronie’s disease is frequently underdiagnosed due to embarrassment or lack of awareness.
In this article, we’ll explore what Peyronie’s disease is, why it happens, how it’s diagnosed, and what treatment options are available—all in clear, accessible language grounded in medical evidence.
Overview / Definition
Peyronie’s disease is a connective tissue disorder characterized by the development of fibrous scar tissue known as plaques within the penis. These plaques form in the tunica albuginea, the fibrous sheath surrounding the erectile tissue.
When scar tissue develops, it can:
- Cause the penis to bend or curve during erection
- Lead to shortening or narrowing of the penis
- Produce pain, especially during erections
- Interfere with sexual intercourse
The curvature may be mild or severe and can curve upward, downward, or to either side. In some cases, Peyronie’s disease can also contribute to erectile dysfunction (ED).
The condition most commonly affects men between 40 and 70 years old, but it can occur at any adult age.
Causes and Risk Factors
The exact cause of Peyronie’s disease is not fully understood, but it is believed to result from abnormal wound healing after minor penile injury.
Potential Causes
- Repetitive microtrauma to the penis during sexual activity or physical activity
- Acute injury causing internal bleeding in penile tissue
- Abnormal healing response, leading to excess collagen and scar tissue formation
In many cases, the patient may not recall a specific injury.
Risk Factors
Several factors increase the likelihood of developing Peyronie’s disease:
- Age (risk increases with age due to reduced tissue elasticity)
- Genetic predisposition
- Family history of Peyronie’s disease
- Connective tissue disorders, such as:
- Dupuytren’s contracture (thickening of tissue in the hands)
- Diabetes
- Smoking
- Prior prostate surgery
These risk factors do not guarantee the condition will develop but may increase susceptibility.
Symptoms and Clinical Presentation
Peyronie’s disease typically develops gradually, though symptoms may sometimes appear suddenly.
Common Symptoms
- Noticeable curvature of the penis during erection
- Palpable lump or hardened plaque under the skin
- Penile pain, particularly during erections
- Shortening of penile length
- Narrowing or indentation (“hourglass” deformity)
- Erectile dysfunction
Phases of Peyronie’s Disease
The condition often progresses in two phases:
- Acute (Active) Phase
- Lasts 6–18 months
- Pain during erections is common
- Curvature may worsen over time
- Plaque is forming
- Chronic (Stable) Phase
- Pain typically improves or resolves
- Curvature stabilizes
- Scar tissue stops progressing
Early evaluation during the active phase may help guide treatment decisions.
Diagnosis and Evaluation
Diagnosis of Peyronie’s disease is primarily clinical and based on history and physical examination.
Medical History
A healthcare provider may ask about:
- Onset and duration of symptoms
- Degree and direction of curvature
- Pain severity
- Impact on sexual function
- History of injury
Physical Examination
The provider will typically:
- Palpate (feel) for plaques in the penis
- Assess curvature (sometimes with self-provided erection photographs)
Imaging Studies
In some cases, imaging may be used:
- Penile ultrasound:
- Identifies plaque location and calcification
- Evaluates penile blood flow
Ultrasound is particularly useful if surgical intervention is being considered.
Treatment and Management Options
Treatment depends on symptom severity, curvature degree, pain, and sexual function impact. Mild cases may not require intervention.
Observation (Watchful Waiting)
For men with:
- Mild curvature
- Minimal discomfort
- No functional impairment
Close monitoring may be appropriate, especially during the acute phase.
Non-Surgical Treatments
1. Oral Medications
While several oral agents have been studied, their effectiveness is limited. Commonly discussed options include:
- Vitamin E (limited evidence)
- Potassium para-aminobenzoate (POTABA)
- Pentoxifylline (may help in early stages)
Evidence for oral therapies is generally modest.
2. Intralesional Injections
This is a more evidence-supported approach.
- Collagenase Clostridium histolyticum (CCH)
- FDA-approved for Peyronie’s disease
- Breaks down collagen within plaques
- Combined with penile modeling exercises
Other injectable agents include:
- Verapamil
- Interferon-alpha
These treatments may reduce curvature in selected patients.
3. Penile Traction Therapy
Mechanical stretching devices may:
- Improve curvature
- Preserve or restore length
- Be used alone or alongside injections
Consistency and proper use are important for effectiveness.
Surgical Treatment
Surgery is typically reserved for men with:
- Stable disease (no progression for at least 3–6 months)
- Significant curvature affecting intercourse
- Severe deformity
Common surgical approaches include:
- Penile Plication
- Shortens the longer side of the penis
- Straightens curvature
- Less complex, but may reduce length
- Plaque Incision or Excision with Grafting
- Removes or cuts plaque
- Grafts tissue to restore shape
- Preserves length better than plication
- Penile Prosthesis Implant
- Recommended for men with severe erectile dysfunction and Peyronie’s disease
- Corrects curvature and restores rigidity
Surgical outcomes are generally favorable in properly selected patients.
Prevention and Lifestyle Considerations
There is no guaranteed way to prevent Peyronie’s disease. However, certain measures may reduce risk or improve overall penile health:
- Avoid traumatic sexual practices
- Use adequate lubrication during intercourse
- Manage chronic conditions such as:
- Diabetes
- High blood pressure
- Stop smoking
- Maintain a healthy weight
Early medical evaluation for new curvature or pain is also important.
Psychological and Emotional Impact
Peyronie’s disease can significantly affect emotional well-being.
Common concerns include:
- Anxiety
- Depression
- Reduced self-esteem
- Relationship stress
Open communication with partners and healthcare providers is essential. Counseling or sex therapy may be beneficial alongside medical treatment.
Conclusion
Peyronie’s disease is a connective tissue disorder that causes penile curvature due to scar tissue formation. While it can be distressing and physically uncomfortable, effective treatment options are available. Early recognition, proper evaluation, and individualized management can significantly improve outcomes.
If you notice new penile curvature, pain, or difficulty with sexual function, seeking medical evaluation is an important first step.
Disclaimer
This article is for educational purposes only and does not constitute medical advice. If you have concerns about Peyronie’s disease or related symptoms, consult a qualified healthcare professional for personalized evaluation and treatment guidance.