Melanoma: Understanding the Most Serious Form of Skin Cancer
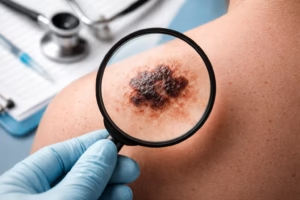
Melanoma is a potentially life-threatening form of skin cancer that develops in the cells responsible for producing pigment in the skin. While it is less common than other types of skin cancer, it is significantly more dangerous due to its ability to spread (metastasize) to other parts of the body if not detected early.
The good news is that melanoma is highly treatable when diagnosed in its early stages. Awareness of risk factors, warning signs, and preventive strategies plays a crucial role in improving outcomes. This article provides a clear and comprehensive overview of melanoma, including its causes, symptoms, diagnosis, treatment options, and prevention.
Overview: What Is Melanoma?
Melanoma is a type of cancer that originates in melanocytes, the cells responsible for producing melanin—the pigment that gives skin its color. While most melanomas develop on the skin, they can also appear:
- Under the nails
- In the eyes (ocular melanoma)
- On mucosal surfaces (such as inside the mouth, nose, or genital areas)
Unlike more common skin cancers such as basal cell carcinoma and squamous cell carcinoma, melanoma is more likely to invade nearby tissues and spread through the lymphatic system or bloodstream.
Types of Melanoma
The main types include:
- Superficial spreading melanoma (most common)
- Nodular melanoma
- Lentigo maligna melanoma
- Acral lentiginous melanoma (more common in people with darker skin)
Causes and Risk Factors
Melanoma begins when DNA damage occurs in melanocytes, often triggered by ultraviolet (UV) radiation. This damage can cause the cells to grow uncontrollably.
Key Risk Factors
- Excessive sun exposure, especially with a history of sunburns
- Use of tanning beds
- Fair skin, light hair, or light-colored eyes
- Large number of moles (especially atypical moles)
- Family history of melanoma
- Personal history of melanoma or other skin cancers
- Weakened immune system
- Increasing age (though melanoma can occur in younger individuals)
While UV exposure is the primary environmental risk factor, melanoma can occur even in sun-protected areas of the body.
Symptoms and Clinical Presentation
The most common sign of melanoma is a new mole or a change in an existing mole.
The ABCDE Rule for Identifying Melanoma
Healthcare professionals often recommend using the ABCDE rule:
- A – Asymmetry: One half of the mole does not match the other.
- B – Border: Edges are irregular, ragged, or blurred.
- C – Color: Uneven color with shades of black, brown, tan, red, white, or blue.
- D – Diameter: Larger than 6 mm (about the size of a pencil eraser), though melanomas can be smaller.
- E – Evolving: Changes in size, shape, color, or symptoms (itching, bleeding).
Additional warning signs may include:
- A sore that does not heal
- Spread of pigment into surrounding skin
- Redness or swelling beyond the mole’s border
- Changes in sensation (itching, tenderness, pain)
Diagnosis and Screening
Early detection dramatically improves survival rates.
Clinical Evaluation
A healthcare professional may perform:
- Visual skin examination
- Dermatoscopy (a specialized magnifying tool)
- Total body photography (for high-risk individuals)
If melanoma is suspected, a biopsy is necessary. This involves removing part or all of the suspicious lesion for microscopic examination.
Staging
If melanoma is confirmed, additional tests may be used to determine whether it has spread. Staging depends on:
- Tumor thickness (Breslow depth)
- Ulceration
- Lymph node involvement
- Presence of distant metastasis
Staging ranges from Stage 0 (in situ) to Stage IV (advanced metastatic melanoma).
Routine population-wide screening for melanoma is not universally recommended, but individuals at high risk may benefit from regular professional skin examinations.
Treatment and Management Options
Treatment depends on the stage, location, and overall health of the patient.
1. Surgical Treatment
- Wide local excision (removal of the tumor and surrounding tissue) is the primary treatment for early-stage melanoma.
- Sentinel lymph node biopsy may be performed to assess spread.
2. Immunotherapy
For advanced melanoma, immunotherapy has significantly improved outcomes. These medications help the immune system recognize and attack cancer cells.
Common approaches include:
- Checkpoint inhibitors (e.g., anti–PD-1, anti–CTLA-4 therapies)
3. Targeted Therapy
For melanomas with specific genetic mutations (such as BRAF mutations), targeted drugs may block cancer growth signals.
4. Radiation Therapy
Used in certain cases, such as:
- When surgery is not possible
- To treat brain metastases
- To reduce recurrence risk
5. Chemotherapy
Less commonly used today due to the effectiveness of newer therapies, but may still be an option in selected cases.
Prevention and Lifestyle Considerations
While not all melanomas can be prevented, risk can be significantly reduced.
Sun Protection Strategies
- Use broad-spectrum sunscreen (SPF 30 or higher) daily
- Reapply sunscreen every two hours when outdoors
- Wear protective clothing (long sleeves, wide-brimmed hats, sunglasses)
- Seek shade during peak sun hours (10 a.m. to 4 p.m.)
- Avoid tanning beds
Skin Self-Examinations
Conduct monthly self-exams to monitor for changes in moles or new skin lesions. Individuals at higher risk should consider regular dermatologist visits.
Conclusion
Melanoma is the most serious type of skin cancer due to its potential to spread rapidly. However, early detection and advances in treatment—particularly immunotherapy and targeted therapy—have substantially improved survival rates.
Key takeaways include:
- Protect your skin from UV exposure.
- Monitor moles using the ABCDE rule.
- Seek medical evaluation for any concerning changes.
- Early diagnosis greatly improves outcomes.
If you notice suspicious skin changes or have concerns about melanoma risk, consult a qualified healthcare professional for proper evaluation and management.
Disclaimer:
This article is intended for educational purposes only and does not replace professional medical advice. If you have specific concerns about your health or skin changes, please consult a qualified healthcare provider for personalized evaluation and treatment.