Malaria: Causes, Symptoms, Treatment, and Prevention
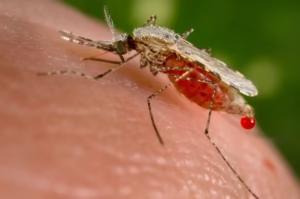
Malaria is a serious and potentially life-threatening infectious disease that continues to affect millions of people worldwide, particularly in tropical and subtropical regions. Despite major advances in prevention and treatment, malaria remains a significant global health concern. Understanding how it spreads, how it presents, and how it can be prevented or treated is essential for both travelers and individuals living in endemic areas.
In this article, we explore malaria in detail—from its causes and symptoms to diagnosis, treatment, and prevention strategies.
Overview / Definition
Malaria is a mosquito-borne infectious disease caused by Plasmodium parasites. These parasites are transmitted to humans through the bite of infected female Anopheles mosquitoes.
There are five species of Plasmodium known to infect humans:
- Plasmodium falciparum (most severe and potentially fatal)
- Plasmodium vivax
- Plasmodium ovale
- Plasmodium malariae
- Plasmodium knowlesi
Among these, P. falciparum causes the majority of severe disease and deaths globally.
Malaria is most prevalent in:
- Sub-Saharan Africa
- South and Southeast Asia
- Parts of Latin America
- Certain regions in the Middle East
Without prompt diagnosis and appropriate treatment, malaria—particularly falciparum malaria—can rapidly become life-threatening.
Causes and Risk Factors
Cause
Malaria is caused by infection with Plasmodium parasites. The transmission cycle includes:
- An infected mosquito bites a human, injecting parasites into the bloodstream.
- The parasites travel to the liver, where they multiply.
- They re-enter the bloodstream and infect red blood cells.
- This cycle leads to the clinical symptoms of malaria.
Risk Factors
Certain factors increase the risk of contracting malaria or developing severe illness:
- Living in or traveling to malaria-endemic areas
- Lack of use of preventive measures (e.g., insecticide-treated bed nets)
- Pregnancy (especially first pregnancies)
- Young children under 5 years
- Weakened immune systems (e.g., HIV infection)
- Delayed diagnosis or treatment
Travelers from non-endemic regions may be at higher risk for severe disease due to lack of partial immunity.
Symptoms or Clinical Presentation
Malaria symptoms typically appear 7–30 days after the infected mosquito bite, although some forms can remain dormant in the liver for months.
Common Symptoms
- Fever (often cyclic or recurring)
- Chills and shaking
- Sweating
- Headache
- Muscle aches
- Fatigue
- Nausea and vomiting
- Diarrhea
The classic pattern involves cycles of:
- Sudden chills
- High fever
- Profuse sweating
However, this pattern is not always present, especially early in the illness.
Severe Malaria
Severe malaria, most commonly caused by P. falciparum, can involve:
- Altered consciousness or confusion
- Seizures
- Severe anemia
- Respiratory distress
- Kidney failure
- Low blood sugar (hypoglycemia)
- Shock
Severe malaria is a medical emergency requiring immediate treatment.
Diagnosis or Screening
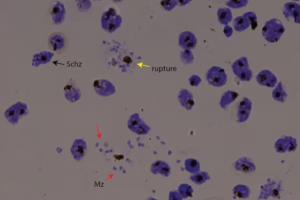
Prompt and accurate diagnosis is essential to prevent complications.
Diagnostic Methods
- Microscopic Blood Examination (Blood Smear)
- The gold standard for diagnosis
- Identifies the presence and species of Plasmodium
- Determines parasite density
- Rapid Diagnostic Tests (RDTs)
- Detect specific malaria antigens
- Provide results within 15–20 minutes
- Useful in areas with limited laboratory access
- Polymerase Chain Reaction (PCR)
- Highly sensitive
- Used primarily in research or complex cases
Anyone with fever who has traveled to or lives in a malaria-endemic area should seek testing promptly.
Treatment or Management Options
Malaria treatment depends on:
- The species of Plasmodium
- Severity of illness
- Geographic region (due to drug resistance patterns)
- Patient-specific factors (age, pregnancy status, other medical conditions)
Uncomplicated Malaria
Common treatment options may include:
- Artemisinin-based combination therapies (ACTs) – First-line treatment in many regions
- Chloroquine (where resistance is not present)
- Atovaquone-proguanil
- Doxycycline (in combination with other drugs)
- Mefloquine
Severe Malaria
Severe cases require hospitalization and intravenous (IV) therapy:
- Intravenous artesunate is the preferred treatment
- Supportive care may include:
- Fluid management
- Blood transfusion (for severe anemia)
- Treatment of low blood sugar
- Management of organ complications
Early treatment significantly reduces the risk of death.
Prevention and Lifestyle Considerations

Malaria is largely preventable with appropriate measures.
Personal Preventive Measures
- Use insecticide-treated bed nets
- Apply mosquito repellents containing DEET, picaridin, or similar agents
- Wear long-sleeved clothing and pants in mosquito-prone areas
- Use indoor residual spraying in high-risk regions
- Install window screens or use air conditioning
Preventive Medication (Chemoprophylaxis)
Travelers to endemic areas may be prescribed antimalarial medications before, during, and after travel. The choice of medication depends on:
- Destination
- Drug resistance patterns
- Duration of travel
- Individual health status
Consultation with a healthcare provider before travel is essential.
Public Health Strategies
- Vector control programs
- Community education
- Early diagnosis and treatment initiatives
- Malaria vaccines (e.g., RTS,S and R21 vaccines in certain regions)
Vaccines offer partial protection but do not replace other preventive measures.
Global Impact and Public Health Significance
Malaria remains a major health burden, particularly in low-resource settings. According to global health estimates:
- Hundreds of millions of cases occur annually
- Children under five are disproportionately affected
- Most deaths occur in Sub-Saharan Africa
Continued investment in prevention, treatment, vaccine development, and healthcare infrastructure is necessary to reduce transmission and mortality.
Conclusion
Malaria is a preventable and treatable infectious disease caused by Plasmodium parasites transmitted through mosquito bites. While symptoms may initially resemble other febrile illnesses, prompt testing and treatment are critical—especially in severe cases.
Key takeaways:
- Malaria is transmitted by infected Anopheles mosquitoes.
- Fever and chills are hallmark symptoms.
- Early diagnosis via blood testing is essential.
- Effective treatments are available, particularly when administered promptly.
- Preventive measures, including mosquito protection and prophylactic medication, significantly reduce risk.
If you live in or plan to travel to a malaria-endemic area, understanding prevention strategies can make a substantial difference in reducing your risk.
Disclaimer
This article is for educational purposes only and does not replace professional medical advice. If you suspect malaria or have concerns about symptoms or prevention, consult a qualified healthcare professional promptly for appropriate evaluation and care.






