Macular Degeneration: Understanding a Leading Cause of Vision Loss
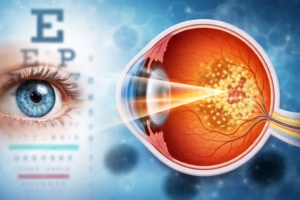
Vision changes can be part of normal aging, but some changes signal more serious eye conditions. Macular degeneration, also known as age-related macular degeneration (AMD), is one of the most common causes of vision loss in adults over 50. It affects central vision—the part we rely on for reading, recognizing faces, and driving—while typically leaving peripheral vision intact.
This article provides a detailed, evidence-based overview of macular degeneration, including its causes, symptoms, diagnosis, and management options.
Overview / Definition
Macular degeneration is a progressive eye disease that affects the macula, a small but vital area near the center of the retina. The retina is the light-sensitive tissue at the back of the eye that sends visual signals to the brain. The macula is responsible for sharp, detailed central vision.
There are two main types:
1. Dry (Atrophic) Age-Related Macular Degeneration
- Most common form (about 80–90% of cases)
- Characterized by thinning of the macula and accumulation of yellow deposits called drusen
- Progresses gradually
2. Wet (Neovascular or Exudative) Age-Related Macular Degeneration
- Less common but more severe
- Caused by abnormal blood vessels growing beneath the retina
- These vessels can leak blood or fluid, leading to rapid vision loss
Both forms can significantly affect quality of life, particularly when reading or performing tasks requiring fine vision.
Causes and Risk Factors
The exact cause of age-related macular degeneration is complex and involves a combination of genetic, environmental, and lifestyle factors.
Key Risk Factors Include:
- Age (greatest risk after age 50)
- Family history of macular degeneration
- Smoking (one of the strongest modifiable risk factors)
- White race
- Obesity
- Cardiovascular disease
- High cholesterol
- Prolonged sun exposure
Genetic variations in certain immune and inflammatory pathways are also linked to increased susceptibility.
Symptoms and Clinical Presentation
Symptoms vary depending on whether the condition is dry or wet and how advanced it is.
Early Symptoms:
- Blurred or fuzzy central vision
- Difficulty reading small print
- Increased need for brighter light
- Trouble recognizing faces
Advanced Symptoms:
- Distorted vision (straight lines appear wavy—known as metamorphopsia)
- Dark or blind spots in central vision
- Reduced color perception
- Sudden central vision loss (more common in wet AMD)
Importantly, macular degeneration does not usually cause complete blindness because peripheral vision remains intact.
Diagnosis and Screening
Early detection is critical, particularly for preventing progression from dry to wet AMD.
Common Diagnostic Methods:
- Comprehensive dilated eye exam
- Amsler grid test (detects central distortion)
- Optical coherence tomography (OCT) – high-resolution imaging of the retina
- Fluorescein angiography – identifies abnormal blood vessels in wet AMD
Routine eye exams are especially important for individuals over age 50 or those at higher risk.
Treatment and Management Options
Treatment depends on the type and severity of macular degeneration.
Dry Macular Degeneration
Currently, there is no cure for dry AMD, but progression may be slowed with:
- AREDS2 nutritional supplements, containing:
- Vitamin C
- Vitamin E
- Zinc
- Copper
- Lutein and zeaxanthin
These supplements are recommended for certain stages of AMD but should only be taken under medical supervision.
Wet Macular Degeneration
Wet AMD is treated more aggressively due to its rapid progression.
Common treatments include:
- Anti-VEGF injections (e.g., ranibizumab, aflibercept, bevacizumab)
- These medications block abnormal blood vessel growth
- Often require repeated injections
- Photodynamic therapy (less common today)
- Laser therapy (selected cases)
These treatments often stabilize vision and may improve it if started early.
Low Vision Rehabilitation
For advanced disease:
- Magnifying devices
- Special reading glasses
- Electronic visual aids
- Occupational therapy for vision adaptation
These strategies can significantly improve independence and quality of life.
Prevention and Lifestyle Considerations
While macular degeneration cannot always be prevented, certain measures can reduce risk or slow progression:
Protective Steps:
- Quit smoking
- Maintain a healthy weight
- Manage blood pressure and cholesterol
- Consume a diet rich in:
- Leafy green vegetables (spinach, kale)
- Fish high in omega-3 fatty acids
- Fruits and colorful vegetables
- Wear sunglasses with UV protection
- Engage in regular physical activity
A heart-healthy lifestyle also supports retinal health.
Conclusion
Macular degeneration is a common, age-related condition that affects central vision and can significantly impact daily life. While there is currently no cure, early detection, appropriate treatment, and healthy lifestyle choices can slow progression and preserve vision for many individuals.
Regular eye examinations are essential, especially for adults over 50 or those with risk factors. Advances in treatment—particularly for wet macular degeneration—have markedly improved outcomes in recent years.
Disclaimer:
This article is intended for educational purposes only and does not replace professional medical advice. If you are experiencing changes in vision or have concerns about your eye health, please consult a qualified healthcare professional or ophthalmologist for evaluation and guidance.