Invasive Ductal Carcinoma: Understanding the Most Common Type of Breast Cancer
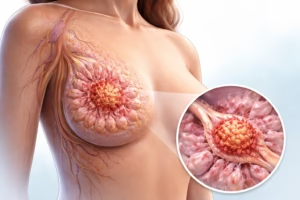
Breast cancer is one of the most widely diagnosed cancers worldwide, affecting millions of individuals each year. Among its various forms, Invasive Ductal Carcinoma (IDC) is the most common type, accounting for approximately 70–80% of all breast cancer cases.
Understanding invasive ductal carcinoma — what it is, how it develops, how it’s diagnosed, and what treatment options are available — can empower individuals to recognize symptoms early and make informed healthcare decisions.
Overview: What Is Invasive Ductal Carcinoma?
Invasive ductal carcinoma begins in the milk ducts of the breast. The term can be broken down as follows:
- Invasive: The cancer has spread beyond the ducts into surrounding breast tissue.
- Ductal: It originated in the milk ducts.
- Carcinoma: A cancer that starts in epithelial (lining) cells.
IDC differs from ductal carcinoma in situ (DCIS), which remains confined to the ducts and has not spread into nearby tissue. Once the cancer becomes invasive, it has the potential to spread to lymph nodes or other parts of the body if left untreated.
IDC can affect both women and men, although it is significantly more common in women.
Causes and Risk Factors
There is no single cause of invasive ductal carcinoma. Instead, it develops through a combination of genetic changes and environmental or lifestyle influences.
Key Risk Factors
- Age (risk increases after age 50)
- Female sex
- Family history of breast cancer
- Inherited genetic mutations (e.g., BRCA1 and BRCA2)
- Personal history of breast conditions or cancer
- Hormonal factors, such as:
- Early menstruation (before age 12)
- Late menopause (after age 55)
- Hormone replacement therapy
- Radiation exposure to the chest
- Obesity, particularly after menopause
- Alcohol consumption
- Sedentary lifestyle
It’s important to note that many people diagnosed with IDC may not have clear risk factors. Conversely, having risk factors does not guarantee cancer development.
Symptoms and Clinical Presentation
In its early stages, invasive ductal carcinoma may not cause noticeable symptoms. This is why routine breast cancer screening is critical.
As IDC progresses, common symptoms may include:
- A new lump or mass in the breast
- Changes in breast shape or size
- Skin changes, such as dimpling or puckering (often described as “peau d’orange”)
- Nipple discharge, especially if bloody
- Nipple inversion or retraction
- Redness or thickening of breast skin
- Swelling in part or all of the breast
- Enlarged lymph nodes in the armpit
Not all breast lumps are cancerous. However, any new or unusual breast change should be evaluated promptly by a healthcare professional.
Diagnosis and Screening
Routine Screening
Early detection greatly improves outcomes. Standard screening tools include:
- Mammography (recommended starting age varies by guideline, typically 40–50 years)
- Breast MRI (for high-risk individuals)
- Clinical breast examinations
Mammograms can identify abnormalities even before symptoms arise.
Diagnostic Testing
If an abnormality is detected, further testing may include:
- Diagnostic mammogram
- Breast ultrasound
- MRI of the breast
- Core needle biopsy (the definitive method for diagnosis)
A biopsy allows pathologists to confirm:
- Whether cancer is present
- Tumor grade (how abnormal the cells appear)
- Hormone receptor status:
- Estrogen receptor (ER)
- Progesterone receptor (PR)
- HER2 status (a protein that may promote aggressive growth)
These characteristics help determine the most effective treatment plan.
Staging and Prognosis
After diagnosis, the cancer is staged based on:
- Tumor size (T)
- Lymph node involvement (N)
- Metastasis (M)
Stages range from Stage I (early, localized cancer) to Stage IV (metastatic cancer).
Prognosis depends on several factors, including:
- Stage at diagnosis
- Tumor grade
- Receptor status
- Overall health of the patient
With modern treatments and early detection, survival rates for localized IDC are high.
Treatment and Management Options
Treatment for invasive ductal carcinoma is individualized and often involves multiple approaches.
1. Surgery
Surgery is typically the first-line treatment:
- Lumpectomy (removal of tumor and small margin of surrounding tissue)
- Mastectomy (removal of entire breast)
- Sentinel lymph node biopsy or axillary lymph node dissection
The choice depends on tumor size, location, genetic factors, and patient preference.
2. Radiation Therapy
Radiation is often used:
- After lumpectomy to reduce recurrence risk
- After mastectomy in certain cases
- To treat metastatic sites when necessary
3. Chemotherapy
Chemotherapy may be recommended:
- Before surgery (neoadjuvant therapy) to shrink the tumor
- After surgery (adjuvant therapy) to reduce recurrence risk
- For advanced or metastatic disease
4. Hormone Therapy
If the tumor is hormone receptor–positive, medications may block estrogen’s effects:
- Tamoxifen
- Aromatase inhibitors (e.g., anastrozole, letrozole)
These therapies may continue for 5–10 years to reduce recurrence risk.
5. Targeted Therapy
For HER2-positive cancers, targeted drugs such as:
- Trastuzumab
- Pertuzumab
Specifically attack cancer cells with minimal damage to normal cells.
6. Immunotherapy
In selected cases (e.g., triple-negative breast cancer), immunotherapy may be incorporated into treatment.
Prevention and Lifestyle Considerations
While invasive ductal carcinoma cannot always be prevented, certain lifestyle choices may reduce risk.
Healthy Lifestyle Strategies
- Maintain a healthy body weight
- Engage in regular physical activity
- Limit alcohol consumption
- Avoid smoking
- Eat a balanced diet rich in fruits, vegetables, and whole grains
- Breastfeed when possible (may offer modest protective effects)
For individuals at very high genetic risk (such as BRCA mutation carriers), preventive options may include enhanced screening, medications, or prophylactic surgery under specialist guidance.
Emotional and Psychological Considerations
A diagnosis of invasive ductal carcinoma can be emotionally overwhelming. Support systems are essential and may include:
- Counseling or mental health professionals
- Support groups
- Patient advocacy organizations
- Oncology social workers
Comprehensive care addresses both physical and emotional well-being.
Conclusion
Invasive ductal carcinoma is the most common form of breast cancer, originating in the milk ducts and spreading into surrounding breast tissue. Early detection through regular screening significantly improves outcomes. Diagnosis typically involves imaging and biopsy, and treatment may include surgery, radiation, chemotherapy, hormone therapy, targeted therapy, or a combination of these approaches.
Although risk factors such as age, genetics, and hormonal influences contribute to its development, lifestyle modifications and regular medical screenings can play a key role in early detection and risk reduction.
If you notice any unusual breast changes or have concerns about your risk, consult a qualified healthcare provider for appropriate evaluation.
Disclaimer
This article is intended for educational purposes only and does not constitute medical advice. For personalized assessment, diagnosis, or treatment, please consult a licensed healthcare professional or medical specialist.






