Heart Valve Disease: Understanding Causes, Symptoms, and Treatment Options
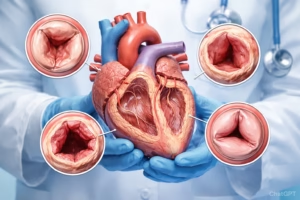
Heart valve disease is a common yet often misunderstood condition that affects how blood flows through the heart. While the heart is a powerful and resilient organ, problems with its valves can disrupt normal circulation and lead to serious complications if left untreated. The good news is that early detection and modern treatment options have significantly improved outcomes for many individuals.
In this article, we’ll explore what heart valve disease is, what causes it, how it presents, and the current approaches to diagnosis and management.
Overview: What Is Heart Valve Disease?
The heart has four valves that ensure blood flows in the right direction:
- Aortic valve
- Mitral valve
- Tricuspid valve
- Pulmonary valve
These valves open and close with each heartbeat, preventing blood from flowing backward.
Heart valve disease occurs when one or more of these valves does not function properly. The main types include:
- Stenosis – Narrowing of a valve, restricting blood flow
- Regurgitation (or insufficiency) – Leakage of blood backward through a valve
- Prolapse – Valve flaps bulge backward (commonly seen in mitral valve prolapse)
Depending on the severity and which valve is affected, heart valve disease can range from mild and asymptomatic to life-threatening.
Causes and Risk Factors
Heart valve disease can be congenital (present at birth) or acquired later in life.
Common Causes
- Age-related degeneration
- Calcium buildup can stiffen valves, especially the aortic valve.
- Rheumatic heart disease
- A complication of untreated streptococcal infections (e.g., strep throat).
- Congenital heart defects
- Abnormal valve formation from birth.
- Infective endocarditis
- Infection of the heart valves, often due to bacteria entering the bloodstream.
- Heart attack or cardiomyopathy
- Damage to heart muscle can affect valve function.
- Connective tissue disorders
- Conditions such as Marfan syndrome can alter valve structure.
Risk Factors
- Older age
- History of rheumatic fever
- High blood pressure
- Coronary artery disease
- Diabetes
- Smoking
- Prior heart surgery
- Family history of valve disorders
Symptoms and Clinical Presentation
Symptoms vary depending on:
- Which valve is affected
- Severity of the disease
- Speed of progression
Some individuals remain symptom-free for years.
Common Symptoms
- Shortness of breath (especially during exertion or when lying flat)
- Fatigue
- Chest pain or pressure
- Heart palpitations
- Lightheadedness or fainting
- Swelling of legs, ankles, or abdomen
- Persistent cough (especially at night)
In severe cases, heart valve disease can lead to:
- Heart failure
- Irregular heart rhythms (arrhythmias)
- Stroke
- Sudden cardiac events
Because symptoms may develop gradually, they are sometimes mistaken for normal aging or reduced fitness.
Diagnosis and Screening
Early detection is crucial for preventing complications.
Physical Examination
A healthcare provider may hear a heart murmur—an abnormal heart sound—using a stethoscope. While not all murmurs indicate disease, further evaluation is often necessary.
Diagnostic Tests
Common tests include:
- Echocardiogram (ultrasound of the heart)
The primary diagnostic tool. It shows valve structure and blood flow. - Electrocardiogram (ECG)
Records electrical activity of the heart. - Chest X-ray
May reveal enlargement of the heart. - Cardiac MRI or CT scan
Offers more detailed imaging. - Cardiac catheterization
Used in complex cases to measure pressure and blood flow directly.
Screening is typically recommended for individuals with known heart murmurs, congenital defects, or risk factors.
Treatment and Management Options
Treatment depends on:
- Type of valve disorder
- Severity
- Presence of symptoms
- Overall health of the patient
1. Monitoring (“Watchful Waiting”)
Mild cases may only require:
- Regular follow-up visits
- Periodic echocardiograms
- Symptom monitoring
2. Medications
While medications cannot fix a damaged valve, they can reduce symptoms and complications.
Common medications include:
- Diuretics (to reduce fluid buildup)
- Blood pressure medications
- Anticoagulants (to prevent clots in certain conditions)
- Beta-blockers
- Medications to control heart rhythm
3. Interventional Procedures
Certain valve conditions can be treated without open-heart surgery:
- Balloon valvuloplasty – A catheter with a balloon widens a narrowed valve.
- Transcatheter Aortic Valve Replacement (TAVR) – A minimally invasive valve replacement option for select patients.
4. Surgery
For severe disease, valve repair or replacement may be necessary.
- Valve repair
- Preferred when feasible
- Preserves natural valve tissue
- Valve replacement
- Mechanical valves (require lifelong blood thinners)
- Biological (tissue) valves (may eventually require replacement)
Advances in cardiac surgery have significantly improved safety and recovery times.
Prevention and Lifestyle Considerations
Not all cases are preventable, especially congenital forms. However, certain steps may reduce risk or slow progression.
Heart-Healthy Habits
- Maintain healthy blood pressure
- Manage cholesterol levels
- Eat a balanced diet rich in fruits, vegetables, and whole grains
- Exercise regularly (as recommended by a healthcare provider)
- Avoid smoking
- Limit alcohol intake
Preventing Infective Endocarditis
In some high-risk individuals, doctors may recommend antibiotics before specific dental or surgical procedures. This approach depends on individual risk factors.
Prompt treatment of strep throat can help prevent rheumatic heart disease.
When to Seek Medical Evaluation
Individuals should seek medical evaluation if they experience:
- Unexplained shortness of breath
- Chest discomfort
- Fainting episodes
- Persistent swelling
- A known heart murmur with new symptoms
Early assessment can prevent disease progression and serious complications.
Conclusion
Heart valve disease affects the normal flow of blood through the heart and can range from mild to life-threatening. Causes include aging, infection, congenital defects, and underlying cardiovascular disease. Symptoms such as shortness of breath, fatigue, and chest pain may develop gradually, making early evaluation essential.
With modern imaging techniques, medications, and advanced surgical options—including minimally invasive procedures—many individuals with valve disorders lead long, active lives. Early detection and appropriate management remain the cornerstone of successful outcomes.
Disclaimer:
This article is intended for informational and educational purposes only. It does not replace professional medical advice, diagnosis, or treatment. If you have symptoms or concerns about heart valve disease, please consult a qualified healthcare professional for personalized evaluation and care.