Congestive heart failure (CHF) is a chronic condition characterized by the heart’s reduced ability to pump blood effectively. While many individuals with CHF can maintain relative stability through medication and lifestyle management, there are periods when symptoms worsen suddenly. This clinical worsening is referred to as an exacerbation of congestive heart failure, often mistakenly described as “exasperated CHF.”
- Fluid overload causes pulmonary congestion, peripheral edema, worsened breathlessness, fatigue, and increased cardiac workload during CHF exacerbations.
- Triggers include excess sodium or fluid intake, missed medications, infections, uncontrolled hypertension, arrhythmias, and other comorbidities, many are preventable.
- Early detection with daily weights, BNP, exams, and timely treatment with diuretics, ACE inhibitors, beta blockers, or hospital care reduces complications.
An exacerbation represents a critical phase in the disease trajectory. During this period, fluid accumulation increases, cardiac workload intensifies, and symptoms such as breathlessness and fatigue become more pronounced. In many cases, exacerbations require urgent medical attention or hospitalization. Therefore, understanding the mechanisms, triggers, warning signs, and management strategies is essential for improving outcomes and preventing complications.
What Is Congestive Heart Failure?
Congestive heart failure occurs when the heart cannot pump sufficient blood to meet the body’s metabolic demands. This inefficiency leads to a cascade of physiological changes that affect multiple organ systems.
Reduced Cardiac Output
The heart’s primary function is to circulate oxygenated blood throughout the body. In CHF, this function is compromised due to weakened or stiffened heart muscle. As a result, organs and tissues receive less oxygen and nutrients, which contributes to fatigue, weakness, and reduced physical capacity.
Fluid Retention (Edema)
Because the heart cannot pump effectively, blood tends to back up in the circulatory system. This increases pressure in blood vessels and causes fluid to leak into surrounding tissues. Fluid accumulation may occur in:
- The lungs, leading to pulmonary congestion
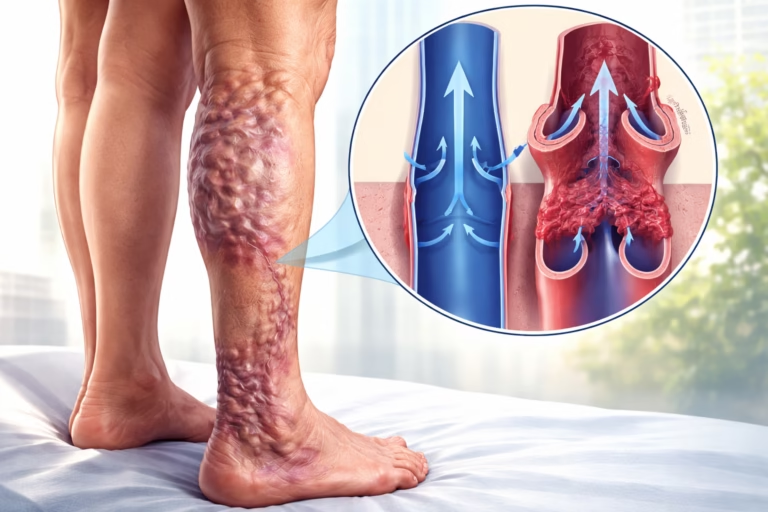
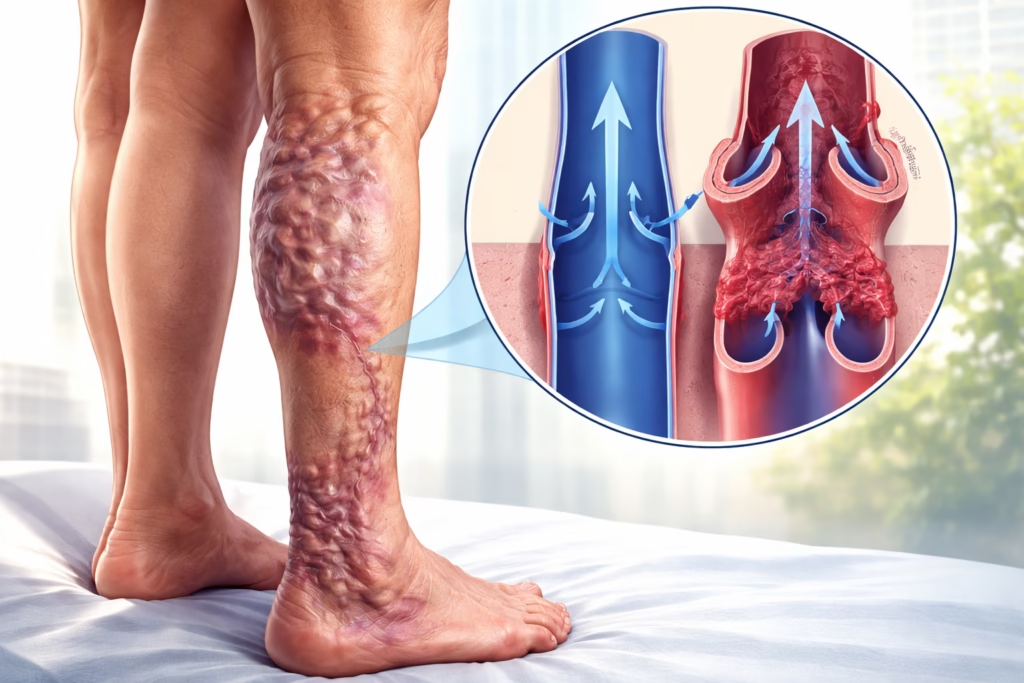
- The lower limbs, causing swelling in the ankles and legs
- The abdomen, resulting in ascites
This fluid buildup is a defining feature of CHF and a major contributor to symptom severity.
Shortness of Breath
When fluid accumulates in the lungs, it interferes with normal gas exchange. This leads to difficulty breathing, particularly during physical activity or when lying flat. In more severe cases, breathlessness may occur even at rest.
CHF often develops as a consequence of underlying conditions such as hypertension, coronary artery disease, or previous myocardial infarction. Over time, these conditions weaken the heart and impair its function.
Defining Exacerbated CHF
An exacerbation of CHF refers to a sudden and clinically significant worsening of symptoms. This deterioration may occur over hours or days and often requires changes in treatment or hospitalization.
During an exacerbation, the balance that had previously kept the condition stable is disrupted. The heart becomes less efficient, fluid retention increases, and symptoms intensify.
Common Triggers of Exacerbation
Exacerbations are often precipitated by identifiable factors.
- Dietary indiscretions: Excess sodium or fluid intake can overwhelm the body’s ability to regulate fluid balance
- Medication noncompliance: Missing doses of prescribed medications, particularly diuretics or heart failure drugs, can lead to rapid deterioration
- Acute illnesses: Infections or uncontrolled hypertension increase physiological stress on the القلب
- Irregular heart rhythms: Arrhythmias can reduce cardiac efficiency and trigger symptom worsening
Recognizing these triggers is essential because many exacerbations are preventable with proper management.
Causes and Triggers of Exacerbations
Dietary Factors
Excess sodium intake is one of the most common causes of fluid retention in CHF patients. Sodium causes the body to retain water, which increases blood volume and places additional strain on the heart.
Similarly, excessive fluid consumption beyond recommended limits can lead to fluid overload. This is particularly problematic in individuals whose kidneys are already struggling to maintain balance.
Medication Issues
Medications such as diuretics, ACE inhibitors, and beta blockers play a crucial role in managing CHF. Skipping doses or discontinuing medication can disrupt fluid regulation and cardiac function.
In addition, certain medications, particularly nonsteroidal anti inflammatory drugs (NSAIDs), can worsen fluid retention and reduce kidney function, thereby exacerbating heart failure symptoms.
Comorbid Conditions
Other medical conditions can significantly influence CHF stability.
- Respiratory infections: Conditions such as pneumonia or viral infections increase oxygen demand and stress the cardiovascular system
- Metabolic disorders: Poorly controlled diabetes or thyroid disease can alter metabolism and worsen cardiac function
These comorbidities often act as external stressors that destabilize an already compromised heart.
Lifestyle Stressors
Both physical and emotional stress can trigger exacerbations. Sudden increases in physical activity may overburden the heart, while emotional stress can lead to hormonal changes that elevate blood pressure and heart rate.
Understanding these lifestyle factors helps patients identify and manage risks proactively.
Recognizing Warning Signs
Early recognition of worsening CHF is critical for preventing severe complications.
Rapid Weight Gain
A sudden increase in body weight, typically 2 to 5 pounds within one to two days, often indicates fluid retention rather than fat accumulation. This is one of the earliest and most reliable signs of exacerbation.
Swelling (Edema)
Fluid buildup may manifest as swelling in the ankles, legs, or abdomen. Shoes may feel tighter, and clothing may become uncomfortable. This reflects increased pressure in the venous system.
Increased Shortness of Breath
Breathlessness may worsen during routine activities or even at rest. Difficulty breathing when lying flat, known as orthopnea, is particularly concerning and suggests pulmonary congestion.
Persistent Cough
A cough producing frothy or pink tinged sputum may indicate fluid in the lungs. This symptom requires urgent evaluation.
Fatigue and Dizziness
Reduced cardiac output leads to decreased oxygen delivery to the brain and muscles. This can cause fatigue, lightheadedness, or fainting episodes.
These warning signs should prompt immediate medical consultation, as early intervention can prevent hospitalization.
Diagnosis and Monitoring
Accurate diagnosis and continuous monitoring are essential for managing exacerbated CHF.
Physical Examination
Healthcare providers assess for signs such as lung crackles, elevated jugular venous pressure, and peripheral edema. These findings indicate fluid overload and cardiac dysfunction.
Imaging
A chest X ray is commonly used to detect fluid accumulation in the lungs and assess heart size.
Blood Tests
Markers such as BNP (B type natriuretic peptide) or NT proBNP are released when the heart is under stress. Elevated levels support the diagnosis of heart failure exacerbation.
Echocardiogram
This imaging test evaluates heart structure and function, including ejection fraction, which measures how effectively the heart pumps blood.
Daily Self Monitoring
Patients play a crucial role in monitoring their condition.
- Daily weight measurement helps detect fluid retention early
- Blood pressure and heart rate tracking provide insight into cardiovascular stability
- Symptom logs allow for pattern recognition and timely intervention
Consistent monitoring empowers patients to identify changes before they become severe.
Treatment and Management Strategies
Diuretics
Diuretics such as furosemide help remove excess fluid from the body. By increasing urine production, they reduce swelling and improve breathing.
Vasodilators and ACE Inhibitors
These medications lower blood pressure and reduce the workload on the heart. By relaxing blood vessels, they improve blood flow and decrease strain on the القلب.
Beta Blockers
Beta blockers slow the heart rate and improve long term cardiac function. They also help reduce the risk of arrhythmias.
Advanced Therapies
In severe cases, additional interventions may be required.
- Inotropes: Medications that increase the strength of heart contractions
- Mechanical devices: Such as left ventricular assist devices (LVAD), which support heart function
Hospital Based Care
Hospitalization may be necessary for close monitoring and intensive treatment.
- Intravenous diuretics provide rapid fluid removal
- Oxygen therapy supports breathing
- Non invasive ventilation may be used in cases of severe respiratory distress
Prevention and Lifestyle Modifications
Dietary Discipline
Limiting sodium intake to less than 2,000 mg per day helps prevent fluid retention. Fluid intake may also need to be restricted, typically to 1.5 to 2 liters per day, depending on medical advice.
Medication Adherence
Taking medications consistently is essential for maintaining stability. Tools such as pill organizers or digital reminders can improve adherence.
Physical Activity
Regular, moderate exercise improves cardiovascular efficiency and overall health. Activities such as walking or cycling should be performed within individual tolerance levels.
Stress Management
Managing stress through techniques such as mindfulness, meditation, or counseling can reduce physiological strain on the heart.
Living Well with CHF
Despite the challenges associated with CHF, many individuals lead active and fulfilling lives through effective management.
- Developing an emergency action plan ensures preparedness during exacerbations
- Educating caregivers improves support and response during critical situations
- Utilizing home health services can provide additional monitoring and assistance
- Staying current with vaccinations reduces the risk of infections that may trigger exacerbations
These strategies enhance both quality of life and long term outcomes.
Conclusion
Exacerbated congestive heart failure represents a serious clinical event that requires immediate attention and careful management. By understanding the underlying mechanisms, recognizing early warning signs, and adhering to treatment and lifestyle recommendations, individuals can significantly reduce the frequency and severity of exacerbations.
Proactive monitoring, consistent communication with healthcare providers, and informed self care are essential components of effective CHF management. With the right approach, it is possible to maintain stability and improve overall well being despite the challenges of this condition.
Call to Action
If you or a loved one experiences symptoms of worsening heart failure, seek medical attention promptly. Early intervention can prevent complications and improve outcomes. For ongoing support and updates on heart health management, consider engaging with trusted healthcare resources and professional guidance.