Yellow Fever: Causes, Symptoms, Prevention, and Treatment

Yellow fever is a serious viral disease that continues to pose a public health threat in certain parts of the world, particularly in tropical regions of Africa and South America. Although it is preventable through vaccination, outbreaks still occur, affecting thousands of people each year.
Understanding how yellow fever spreads, its symptoms, and how it can be prevented is essential—especially for travelers and those living in endemic areas. In this article, we’ll explore the disease in clear, accessible terms while maintaining accurate, evidence-based information.
Overview: What Is Yellow Fever?
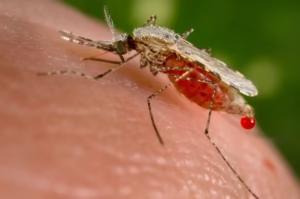
Yellow fever is a viral hemorrhagic disease caused by the yellow fever virus, a member of the Flavivirus family. It is primarily transmitted to humans through the bite of infected mosquitoes, particularly Aedes aegypti.
The disease gets its name from one of its hallmark symptoms: jaundice, which is the yellowing of the skin and eyes caused by liver involvement.
Where Is Yellow Fever Found?
Yellow fever occurs in:
- Sub-Saharan Africa
- Tropical regions of South America
- Certain forested or urban areas where infected mosquitoes are present
Some countries require proof of yellow fever vaccination for entry.
Causes and Risk Factors
What Causes Yellow Fever?
Yellow fever is caused by infection with the yellow fever virus. The virus is transmitted by infected mosquitoes in three cycles:
- Sylvatic (jungle) cycle – Transmission between monkeys and forest mosquitoes; humans become infected when they enter forested areas.
- Intermediate (savannah) cycle – Transmission from mosquitoes to both monkeys and humans in rural areas.
- Urban cycle – Human-to-human transmission via urban mosquitoes (especially Aedes aegypti).
Risk Factors
You may be at increased risk if you:
- Live in or travel to endemic tropical regions
- Are unvaccinated
- Spend time outdoors in mosquito-prone areas
- Work in forested or rural environments
- Travel without proper mosquito protective measures
Symptoms and Clinical Presentation
Yellow fever symptoms typically appear 3 to 6 days after infection. The illness can range from mild to severe, and in some cases, can be fatal.
Stage 1: Acute Phase
Most infected individuals develop:
- Sudden fever
- Chills
- Severe headache
- Back and muscle pain
- Fatigue
- Nausea and vomiting
- Loss of appetite
Many patients improve after this stage.
Stage 2: Toxic Phase (Severe Cases)
Approximately 15% of patients enter a more severe phase within 24 hours of remission. This stage can involve:
- High fever
- Jaundice (yellowing of skin and eyes)
- Abdominal pain
- Persistent vomiting (sometimes with blood)
- Bleeding from nose, mouth, or stomach
- Kidney dysfunction
- Liver failure
- Shock
The toxic phase can be life-threatening. Mortality rates among severe cases range from 20% to 50%.
Diagnosis and Screening
Early symptoms of yellow fever resemble other tropical infections such as:
- Malaria
- Dengue fever
- Zika virus
- Viral hepatitis
Because of this similarity, laboratory testing is essential.
Diagnostic Methods
- Blood tests to detect antibodies or viral RNA
- Liver function tests to assess organ involvement
- Polymerase chain reaction (PCR) testing in early stages
Diagnosis can be challenging in areas with limited healthcare resources.
Individuals with recent travel to endemic regions and compatible symptoms should seek medical evaluation promptly.
Treatment and Management Options
There is no specific antiviral treatment for yellow fever. Care is primarily supportive.
Supportive Management May Include:
- Intravenous fluids to prevent dehydration
- Medication to reduce fever and pain (avoiding drugs that increase bleeding risk, such as aspirin)
- Monitoring and support for liver and kidney function
- Blood transfusions if necessary
- Hospitalization in severe cases
Early supportive care improves survival rates significantly.
Because no cure exists, prevention remains the most effective strategy against yellow fever.
Prevention and Lifestyle Considerations
1. Vaccination
The yellow fever vaccine is:
- Highly effective (more than 95% protection)
- Given as a single dose
- Usually provides lifelong immunity
The vaccine is made from a live, weakened virus and is generally safe for most individuals over 9 months of age. However, certain people—such as those with severe immune system compromise—should consult a healthcare provider before vaccination.
Many countries require proof of vaccination (International Certificate of Vaccination or Prophylaxis) for travelers entering or leaving endemic areas.
2. Mosquito Control and Personal Protection
Even if vaccinated, mosquito bite prevention is essential:
- Use insect repellent containing DEET, picaridin, IR3535, or oil of lemon eucalyptus
- Wear long-sleeved clothing and long pants
- Use mosquito nets treated with insecticide
- Stay in accommodations with screened windows or air conditioning
- Eliminate standing water around living areas
3. Community-Level Prevention
Public health measures include:
- Mosquito control programs
- Vaccination campaigns during outbreaks
- Surveillance and rapid outbreak response
When to Seek Medical Care
Anyone who experiences:
- Fever after travel to endemic areas
- Jaundice
- Bleeding symptoms
- Severe abdominal pain
should seek immediate medical evaluation.
Early medical attention can significantly improve outcomes.
Conclusion
Yellow fever is a potentially severe but preventable viral disease transmitted by infected mosquitoes. While many infections are mild, some cases progress to liver and kidney failure, bleeding, and death. Because no specific antiviral treatment exists, prevention—especially vaccination and mosquito control—is critical.
With proper public health strategies, increased vaccination coverage, and informed travelers, the global burden of yellow fever can be significantly reduced.
Disclaimer:
This article is for educational purposes only and is not a substitute for professional medical advice. If you have concerns about yellow fever, vaccination, or symptoms after travel, please consult a qualified healthcare provider or public health authority.