Psoriatic Arthritis: Understanding the Link Between Skin and Joint Health
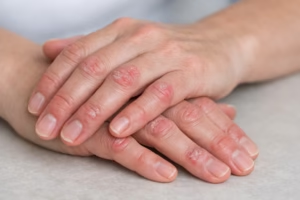
Psoriatic arthritis (PsA) is a chronic inflammatory condition that affects both the skin and joints. It commonly develops in people who have psoriasis—a long-term autoimmune skin disorder characterized by red, scaly patches. However, joint symptoms may sometimes appear before noticeable skin changes, making diagnosis more complex.
Psoriatic arthritis can range from mild to severe and, if left untreated, may lead to joint damage and reduced quality of life. The good news is that early recognition and appropriate treatment can significantly improve outcomes. This article explores the causes, symptoms, diagnosis, treatment options, and lifestyle considerations for managing psoriatic arthritis.
Overview / Definition
Psoriatic arthritis is a type of inflammatory arthritis associated with psoriasis. It belongs to a group of conditions known as spondyloarthropathies, which are characterized by inflammation of the joints, spine, and areas where tendons and ligaments attach to bone (entheses).
Key features of psoriatic arthritis include:
- Joint pain, stiffness, and swelling
- Skin and nail changes typical of psoriasis
- Inflammation that may affect fingers, toes, spine, and pelvis
- Fluctuating periods of flare-ups and remission
Psoriatic arthritis affects men and women equally and most commonly develops between ages 30 and 50, although it can occur at any age.
Causes and Risk Factors
Psoriatic arthritis is considered an autoimmune disease, meaning the immune system mistakenly attacks healthy tissues. While the exact cause is not fully understood, several factors are believed to contribute.
1. Genetic Factors
- Family history of psoriasis or psoriatic arthritis increases risk
- Certain genetic markers (such as HLA-B27) are associated with specific forms of the condition
2. Immune System Dysregulation
- Overactive immune response leads to inflammation in skin and joints
3. Environmental Triggers
- Infections
- Physical trauma (sometimes referred to as the “Koebner phenomenon”)
- Emotional stress
Not everyone with psoriasis develops psoriatic arthritis. However, approximately 20–30% of people with psoriasis may eventually develop joint involvement.
Symptoms and Clinical Presentation
Symptoms can vary widely in severity and pattern. Some individuals experience mild intermittent symptoms, while others develop progressive joint damage.
Common Joint Symptoms
- Joint pain and tenderness
- Morning stiffness lasting longer than 30 minutes
- Swelling of entire fingers or toes (dactylitis), sometimes called “sausage digits”
- Reduced range of motion
- Lower back pain due to spinal involvement
Skin and Nail Changes
- Red, scaly plaques on elbows, knees, scalp, or trunk
- Pitting or ridging of the nails
- Nail separation from the nail bed (onycholysis)
Other Features
- Enthesitis (pain at tendon and ligament attachment sites, such as the Achilles tendon)
- Fatigue
- Eye inflammation (uveitis), which may cause redness and visual changes
Because symptoms can overlap with other forms of arthritis, proper evaluation is essential.
Diagnosis and Screening
There is no single definitive test for psoriatic arthritis. Diagnosis typically involves a combination of clinical evaluation, imaging, and laboratory testing.
Clinical Assessment
A healthcare provider will evaluate:
- Personal and family history of psoriasis
- Pattern of joint involvement
- Nail changes
- Presence of dactylitis or enthesitis
Imaging Studies
- X-rays to assess joint damage
- MRI or ultrasound to detect early inflammatory changes
Laboratory Tests
- Blood tests to rule out rheumatoid arthritis (e.g., rheumatoid factor, anti-CCP antibodies)
- Inflammatory markers (ESR, CRP)
- Genetic markers such as HLA-B27 in some cases
Early diagnosis is crucial to prevent irreversible joint damage.
Treatment and Management Options
While there is currently no cure for psoriatic arthritis, effective treatment can control inflammation, relieve symptoms, and prevent long-term complications.
Treatment is often tailored to the severity and pattern of disease.
1. Medications
Nonsteroidal Anti-Inflammatory Drugs (NSAIDs)
- Help relieve pain and inflammation
- Typically used for mild cases
Disease-Modifying Antirheumatic Drugs (DMARDs)
- Examples: methotrexate, sulfasalazine, leflunomide
- Slow disease progression
Biologic Therapies
- Target specific immune pathways (e.g., TNF inhibitors, IL-17 inhibitors, IL-23 inhibitors)
- Often used in moderate to severe disease
Targeted Synthetic DMARDs
- Such as JAK inhibitors
- Used when other therapies are ineffective
Corticosteroids
- May be used short term to control flares
2. Physical and Occupational Therapy
- Improve joint mobility
- Strengthen supporting muscles
- Protect joints during daily activities
3. Surgery (Rare Cases)
- Joint replacement may be considered when severe damage occurs
Early, aggressive treatment is associated with better long-term outcomes.
Prevention and Lifestyle Considerations
Although psoriatic arthritis cannot be fully prevented, certain lifestyle strategies can help reduce flare-ups and improve overall well-being.
Maintain a Healthy Weight
- Reduces stress on joints
- May improve response to treatment
Engage in Regular, Low-Impact Exercise
- Swimming
- Walking
- Yoga or stretching
Manage Stress
- Mindfulness techniques
- Adequate sleep
- Counseling if needed
Avoid Smoking
- Smoking may worsen autoimmune inflammation
Follow Treatment Plans Closely
- Consistent medication use
- Regular follow-up appointments
A comprehensive approach combining medical treatment and healthy lifestyle habits can significantly improve quality of life.
Conclusion
Psoriatic arthritis is a chronic autoimmune condition that affects both skin and joints. It can range from mild discomfort to progressive joint damage if untreated. Recognizing early symptoms—such as joint pain, stiffness, nail changes, or dactylitis—is critical for timely diagnosis.
Modern treatment options, including DMARDs and biologic therapies, have significantly improved the outlook for individuals with this condition. With proper medical care, physical activity, and lifestyle modifications, many people with psoriatic arthritis can lead active, fulfilling lives.
Disclaimer: This article is intended for educational purposes only and does not constitute medical advice. If you are experiencing symptoms or have concerns about psoriatic arthritis, please consult a qualified healthcare professional for proper evaluation and personalized care.






