PMS: Understanding Premenstrual Syndrome

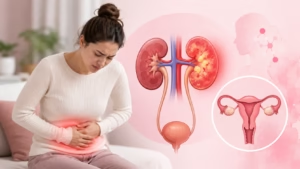
Premenstrual Syndrome (PMS) is a common condition that affects many individuals who menstruate, typically occurring in the days or weeks before a menstrual period. While often discussed casually, PMS can involve a wide range of physical, emotional, and behavioral symptoms that meaningfully impact daily life.
Although mild symptoms are common, for some individuals PMS can be disruptive and require medical evaluation. Understanding what PMS is, why it happens, and how it can be managed is an important step toward improving overall menstrual health.
Overview / Definition
Premenstrual Syndrome (PMS) refers to a group of recurring physical, emotional, and behavioral symptoms that occur during the luteal phase of the menstrual cycle — usually 1–2 weeks before menstruation begins — and resolve shortly after the period starts.
PMS is extremely common. Studies suggest that:
- Up to 75% of menstruating individuals experience at least one PMS symptom.
- About 20–30% have symptoms significant enough to interfere with work, school, or relationships.
- Approximately 3–8% experience a more severe form known as Premenstrual Dysphoric Disorder (PMDD).
PMS can occur at any reproductive age but is often reported more frequently in individuals in their late 20s to early 40s.
Causes and Risk Factors
The exact cause of PMS is not fully understood, but it is strongly associated with cyclical hormonal changes during the menstrual cycle.
Hormonal Fluctuations
After ovulation, levels of estrogen and progesterone rise and then decline if pregnancy does not occur. These hormonal shifts may affect:
- Neurotransmitters, particularly serotonin (which influences mood)
- Fluid balance
- Pain sensitivity
Notably, individuals with PMS usually have normal hormone levels, but may be more sensitive to hormonal changes.
Other Contributing Factors
- Serotonin fluctuations (linked to mood changes and food cravings)
- Genetic predisposition
- High stress levels
- Poor sleep habits
- Lack of regular exercise
Risk Factors
Certain factors may increase the likelihood or severity of PMS:
- History of depression or anxiety
- Family history of PMS or mood disorders
- Smoking
- High caffeine intake
- High levels of chronic stress
Symptoms and Clinical Presentation
PMS symptoms typically occur in a predictable pattern during the luteal phase and resolve with the onset of menstruation. They can vary widely in type and severity.
Physical Symptoms
- Bloating or abdominal discomfort
- Breast tenderness
- Headaches
- Joint or muscle pain
- Fatigue
- Acne
- Changes in appetite or food cravings
- Constipation or diarrhea
Emotional and Behavioral Symptoms
- Irritability
- Mood swings
- Anxiety
- Depressive feelings
- Crying spells
- Difficulty concentrating
- Sleep disturbances
- Social withdrawal
For a diagnosis of PMS, symptoms must:
- Occur repeatedly in the luteal phase
- Improve within a few days after menstruation begins
- Interfere with daily functioning to some degree
When symptoms are severe — especially mood-related symptoms such as intense depression, anger, or hopelessness — a healthcare professional may evaluate for Premenstrual Dysphoric Disorder (PMDD), a more serious condition.
Diagnosis or Screening
There is no single laboratory test for PMS. Diagnosis is primarily based on:
- A detailed medical history
- Symptom tracking over at least two menstrual cycles
- Exclusion of other conditions
Healthcare providers may recommend keeping a daily symptom diary, noting:
- Mood changes
- Physical symptoms
- Menstrual cycle timing
- Severity and duration
Other conditions that can mimic or worsen PMS include:
- Thyroid disorders
- Depression or anxiety disorders
- Chronic fatigue syndrome
- Irritable bowel syndrome (IBS)
In some cases, blood tests may be performed to rule out these underlying conditions.
Treatment and Management Options
Treatment depends on symptom severity and individual health factors. Management often involves a combination of lifestyle adjustments and medical therapies.
1. Lifestyle Modifications
For mild to moderate PMS, lifestyle changes may significantly reduce symptoms:
- Regular exercise: At least 30 minutes of moderate activity most days
- Balanced diet: Emphasizing whole grains, fruits, vegetables, and lean protein
- Reducing salt to decrease bloating
- Limiting caffeine and alcohol
- Adequate sleep (7–9 hours per night)
- Stress reduction techniques (yoga, meditation, mindfulness)
2. Nutritional Supplements
Some individuals may benefit from:
- Calcium supplements
- Vitamin B6 (within safe dosing limits)
- Magnesium
Supplement use should be discussed with a healthcare professional to ensure safety and appropriate dosing.
3. Medications
If symptoms are moderate to severe, medical treatment may include:
- Nonsteroidal anti-inflammatory drugs (NSAIDs): For pain and cramping
- Hormonal contraceptives: To regulate or suppress ovulation
- Selective Serotonin Reuptake Inhibitors (SSRIs): Especially effective for mood-related PMS or PMDD
- Diuretics: In select cases for significant fluid retention
Treatment plans are individualized based on symptom profile and overall health.
Prevention and Lifestyle Considerations
While PMS cannot always be prevented, symptom severity may be reduced through healthy habits:
- Maintain a consistent exercise routine
- Eat smaller, more frequent meals
- Avoid smoking
- Manage stress proactively
- Track symptoms to identify patterns
Awareness of one’s cycle can be empowering and helps in anticipating and managing recurring symptoms more effectively.
When to Seek Medical Attention
Consult a healthcare professional if:
- Symptoms interfere with work, school, or relationships
- Mood symptoms include persistent depression or thoughts of self-harm
- PMS suddenly worsens
- There is irregular bleeding or unusual cycle changes
Severe mood symptoms require prompt medical evaluation.
Conclusion
Premenstrual Syndrome (PMS) is a common condition characterized by recurring physical and emotional symptoms in the days before menstruation. While many individuals experience mild discomfort, others may face symptoms that significantly affect daily life.
Understanding hormonal influences, tracking symptoms, and implementing lifestyle adjustments are often effective first steps. When needed, medical therapies, including hormonal treatments or antidepressants, can provide meaningful relief. With proper evaluation and management, most individuals can successfully reduce the impact of PMS on their health and well-being.
Disclaimer:
This article is intended for educational purposes only and does not replace professional medical advice. If you experience persistent, severe, or concerning symptoms, consult a qualified healthcare professional for personalized evaluation and treatment.