Joint Pain: Causes, Symptoms, and Effective Management Strategies
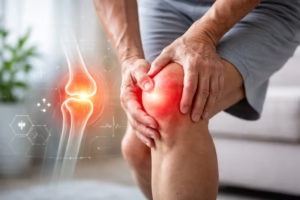
Joint pain is one of the most common health complaints across all age groups. It can affect a single joint, such as the knee or shoulder, or multiple joints throughout the body. While some cases are mild and temporary, others may signal underlying medical conditions requiring treatment. Understanding the causes, symptoms, and management options for joint pain can help individuals make informed decisions about their health.
Overview: What Is Joint Pain?
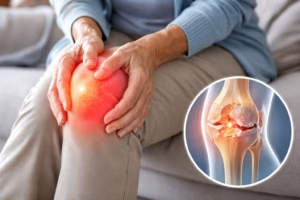
Joint pain refers to discomfort, stiffness, or soreness in one or more joints—the areas where two or more bones meet. Commonly affected joints include the knees, hips, shoulders, hands, and spine.
The pain may arise from the joint structures themselves (including cartilage, ligaments, or synovial lining) or from surrounding tissues such as muscles and tendons. Joint pain can be acute (short-term) or chronic (lasting more than three months).
Causes and Risk Factors
Joint pain has many potential causes ranging from temporary injuries to chronic systemic conditions.
Common Causes
- Osteoarthritis: Degenerative “wear-and-tear” arthritis caused by cartilage breakdown
- Rheumatoid arthritis: An autoimmune condition where the body attacks its own joints
- Gout: A form of inflammatory arthritis caused by uric acid crystal buildup
- Bursitis: Inflammation of the small fluid-filled sacs that cushion joints
- Tendinitis: Inflammation of tendons surrounding a joint
- Injury: Sprains, strains, fractures, or ligament tears
- Infections: Septic arthritis or viral infections can cause joint inflammation
Risk Factors
Certain factors increase the likelihood of developing joint pain:
- Advancing age
- Obesity (increased stress on weight-bearing joints)
- Previous joint injury
- Repetitive motion activities
- Family history of arthritis
- Autoimmune disorders
- Sedentary lifestyle
Symptoms and Clinical Presentation
Joint pain may present differently depending on the underlying cause.
Common Symptoms Include:
- Aching or throbbing pain
- Joint stiffness (especially in the morning or after inactivity)
- Swelling or warmth around the joint
- Redness
- Reduced range of motion
- Clicking or grinding sensation
When to Seek Medical Attention
Prompt evaluation is important if joint pain is accompanied by:
- Sudden, severe swelling
- Inability to bear weight
- Fever with joint redness and warmth
- Deformity after injury
- Persistent symptoms lasting more than a few weeks
Diagnosis and Evaluation
A healthcare provider evaluates joint pain using a combination of:
1. Medical History
- Onset and duration of pain
- Pattern (single vs. multiple joints)
- Triggers or relieving factors
- Family history of autoimmune disease
2. Physical Examination
- Assessment of swelling, tenderness, warmth
- Joint mobility testing
- Functional movement assessment
3. Diagnostic Tests (if needed)
- Blood tests: To detect inflammation markers or autoimmune conditions
- Imaging studies:
- X-rays (to assess bone damage or arthritis)
- MRI (to evaluate soft tissues)
- Ultrasound (to detect fluid or inflammation)
- Joint fluid analysis in cases of suspected infection or gout
Accurate diagnosis is essential to guide proper treatment.
Treatment and Management Options
Treatment varies depending on the cause, severity, and duration of joint pain.
Conservative (Non-Surgical) Management
Medications
- Acetaminophen for mild pain
- Nonsteroidal anti-inflammatory drugs (NSAIDs) for inflammation
- Topical analgesics
- Disease-modifying antirheumatic drugs (DMARDs) for autoimmune conditions
- Corticosteroid injections in selected cases
Physical Therapy
- Strengthening exercises
- Range-of-motion exercises
- Posture correction
- Activity modification techniques
Lifestyle Measures
- Rest during acute flare-ups
- Heat therapy (for stiffness)
- Cold therapy (for swelling)
- Assistive devices (braces, orthotics)
Surgical Options
In resistant or advanced cases:
- Arthroscopy (minimally invasive joint repair)
- Joint realignment procedures
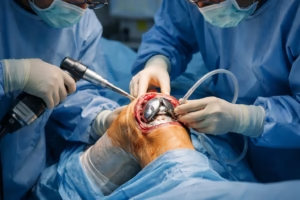
- Joint replacement (e.g., knee or hip replacement)
Surgical intervention is usually reserved for severe cases where conservative treatments fail.
Prevention and Lifestyle Considerations
Many forms of joint pain can be prevented or minimized with healthy habits.
Practical Strategies:
- Maintain a healthy weight to reduce stress on joints
- Engage in regular low-impact exercise, such as:
- Swimming
- Walking
- Cycling
- Yoga
- Strengthen muscles around joints to improve stability
- Use proper techniques during sports or repetitive tasks
- Avoid prolonged inactivity
- Follow an anti-inflammatory diet rich in:
- Fruits and vegetables
- Omega-3 fatty acids
- Whole grains
Early management of minor joint issues may prevent long-term complications.
Conclusion
Joint pain is a common yet complex symptom that can stem from injury, inflammation, autoimmune disorders, or degenerative conditions. Recognizing the underlying cause is essential for effective treatment. While many cases improve with conservative measures such as exercise, medication, and lifestyle modifications, persistent or severe symptoms warrant medical evaluation.
Early diagnosis and proactive management can significantly improve mobility, comfort, and overall quality of life.
Disclaimer:
This article is intended for educational purposes only and does not constitute medical advice. If you are experiencing persistent or severe joint pain, consult a qualified healthcare professional for proper evaluation and individualized treatment recommendations.