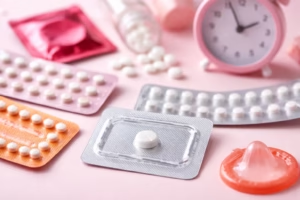
IUDs: A Comprehensive Guide to Intrauterine Devices
Intrauterine devices (IUDs) are among the most effective and widely used forms of reversible contraception worldwide. Safe, long-lasting, and low-maintenance, IUDs offer reliable pregnancy prevention for people seeking either short-term or extended birth control solutions. Despite their growing popularity, many individuals still have questions about how they work, their safety, and what to expect.
This article provides a medically accurate, easy-to-understand overview of IUDs, including how they function, potential risks, side effects, and what to consider before choosing one.
Overview / Definition
An intrauterine device (IUD) is a small, T-shaped device inserted into the uterus by a trained healthcare professional to prevent pregnancy. Depending on the type, IUDs can work for 3 to 10 years.
There are two main types of IUDs:
1. Hormonal IUDs
These release a small amount of progestin (levonorgestrel) into the uterus. Brand names may include Mirena®, Kyleena®, Liletta®, and Skyla®.
They prevent pregnancy by:
- Thickening cervical mucus (blocking sperm)
- Thinning the uterine lining
- Sometimes suppressing ovulation
2. Copper IUDs
The most common brand is ParaGard®. These devices:
- Contain copper, which is toxic to sperm
- Create an inflammatory reaction in the uterus that prevents fertilization
- Can remain effective for up to 10–12 years
Both types are over 99% effective, making them among the most reliable contraceptive methods available.
Causes or Risk Factors (Why Consider an IUD?)
People choose IUDs for a variety of reasons, including:
- Desire for long-term, low-maintenance contraception
- Difficulty remembering daily birth control pills
- Contraindications to estrogen-containing contraceptives
- Preference for non-hormonal birth control (copper IUD)
- Management of heavy menstrual bleeding (hormonal IUDs)
While IUDs are safe for most individuals—including adolescents and those who have not been pregnant—certain medical conditions may affect eligibility.
Relative Contraindications May Include:
- Current pelvic infection
- Unexplained vaginal bleeding
- Certain uterine abnormalities
- Active cervical or endometrial cancer
A healthcare provider evaluates individual risk factors before insertion.
Symptoms or Clinical Presentation
IUDs themselves do not cause pregnancy symptoms but may produce temporary side effects after insertion.
Common Initial Side Effects:
- Cramping
- Light bleeding or spotting
- Back discomfort
- Dizziness immediately after insertion
These symptoms typically improve within days to weeks.
Hormonal IUD Side Effects May Include:
- Lighter periods
- Irregular spotting (especially in first 3–6 months)
- Amenorrhea (absence of periods) over time
- Breast tenderness or mild acne (less common)
Copper IUD Side Effects May Include:
- Heavier menstrual bleeding
- Stronger menstrual cramps
- Longer periods
Serious complications are rare but may include:
- Expulsion (IUD partially or fully falling out)
- Perforation (very rare uterine injury during insertion)
- Pelvic inflammatory disease (most common in first 20 days if infection is present)
Diagnosis or Screening
Before inserting an IUD, healthcare providers typically perform:
- A medical history review
- Pregnancy exclusion
- Screening for sexually transmitted infections (STIs) if indicated
- A pelvic exam
Once inserted, IUD placement is usually confirmed by:
- Visualization of the IUD strings
- Ultrasound (if placement is uncertain)
Routine follow-up may be scheduled a few weeks after insertion, although many guidelines now indicate that follow-up is only necessary if symptoms occur.
Treatment or Management Options
IUD care is generally straightforward.
After Insertion:
- Mild cramping can be managed with over-the-counter pain relief (as directed by a healthcare provider).
- Patients are advised to check IUD strings periodically.
If Side Effects Occur:
- Irregular bleeding often improves within several months.
- Persistent pain, unusual discharge, or fever requires medical evaluation.
Removal
IUD removal:
- Is quick and typically uncomplicated
- Can be done at any time by a healthcare provider
- Allows for rapid return to fertility (often within weeks)
Prevention or Lifestyle Considerations
Although IUDs are excellent at preventing pregnancy, they do not protect against sexually transmitted infections (STIs). Barrier methods like condoms are recommended for STI prevention.
Additional considerations:
- IUDs can also be used as emergency contraception (copper IUD within 5 days of unprotected intercourse).
- Hormonal IUDs are commonly used to treat:
- Heavy menstrual bleeding
- Endometriosis pain
- Adenomyosis
- Regular gynecological care remains important even with an IUD in place.
Benefits of IUDs
- Over 99% effective
- Long-lasting
- Reversible
- Minimal maintenance
- No daily action required
- Safe for most individuals
Potential Drawbacks
- Requires in-office insertion
- Possible irregular bleeding
- Does not protect against STIs
- Rare procedural complications
Conclusion
IUDs are a highly effective, reversible form of long-term contraception suitable for many individuals. Available in hormonal and non-hormonal options, they offer flexibility for different health needs and lifestyle preferences. While side effects such as temporary cramping or changes in menstrual patterns may occur, serious complications are uncommon when inserted by trained professionals.
Choosing a contraceptive method is a personal decision best made with accurate information and guidance from a qualified healthcare provider.
Disclaimer: This article is for educational purposes only and does not replace professional medical advice. Always consult a qualified healthcare professional to discuss your individual health needs and determine the most appropriate contraceptive option for you.