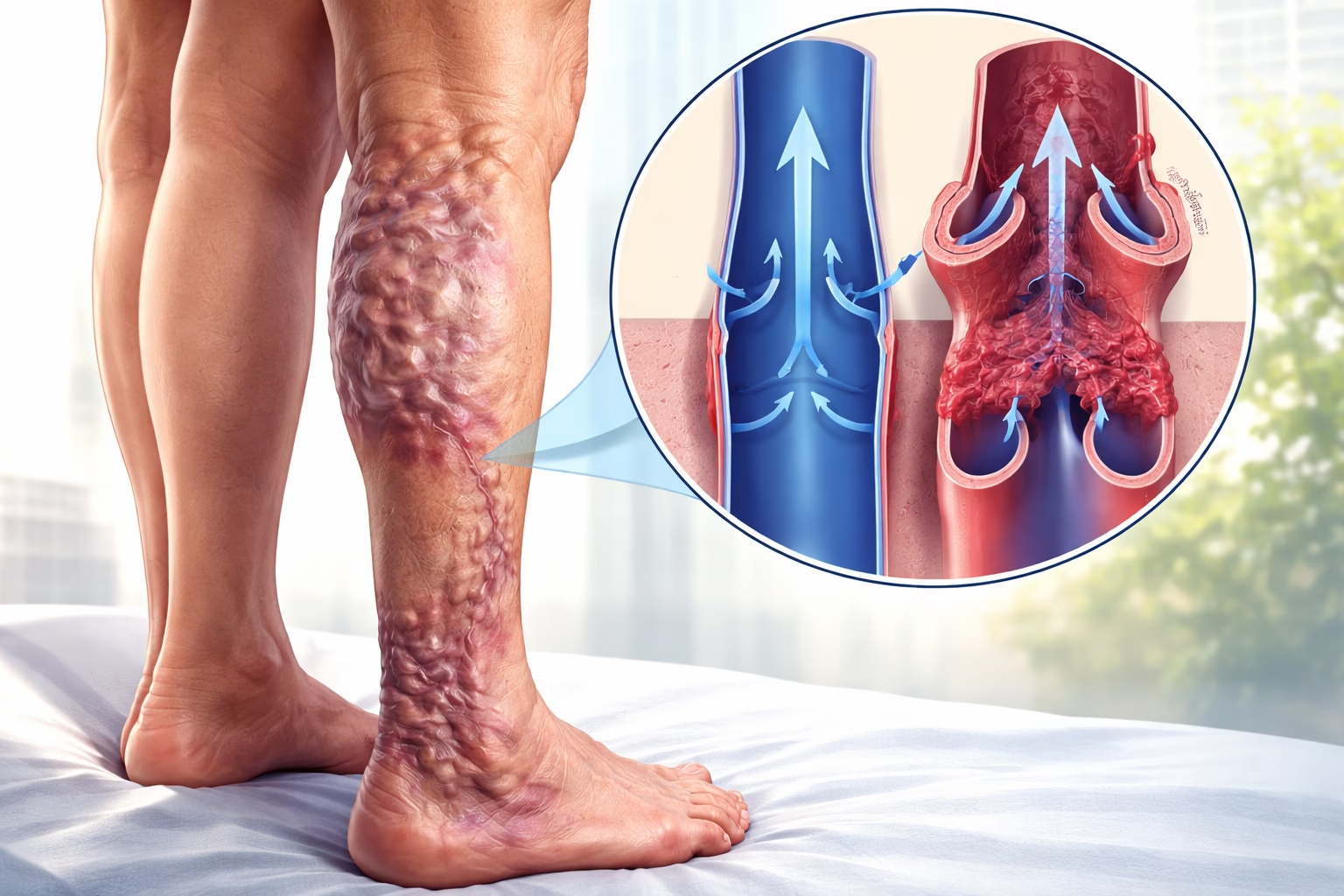
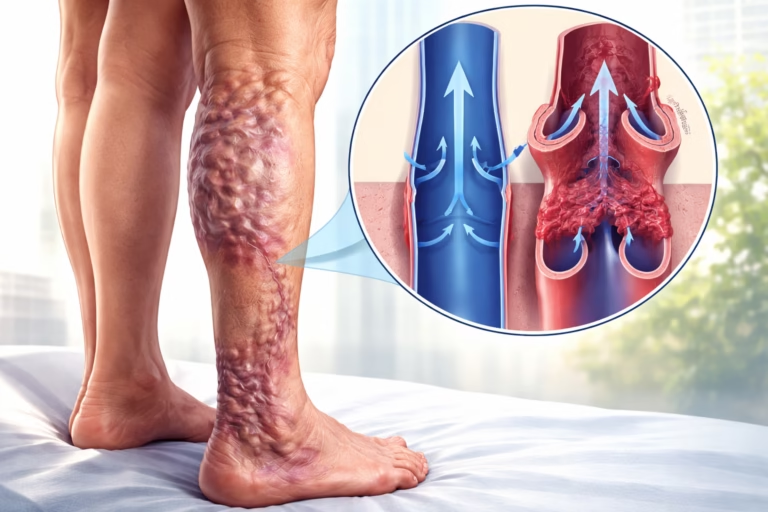
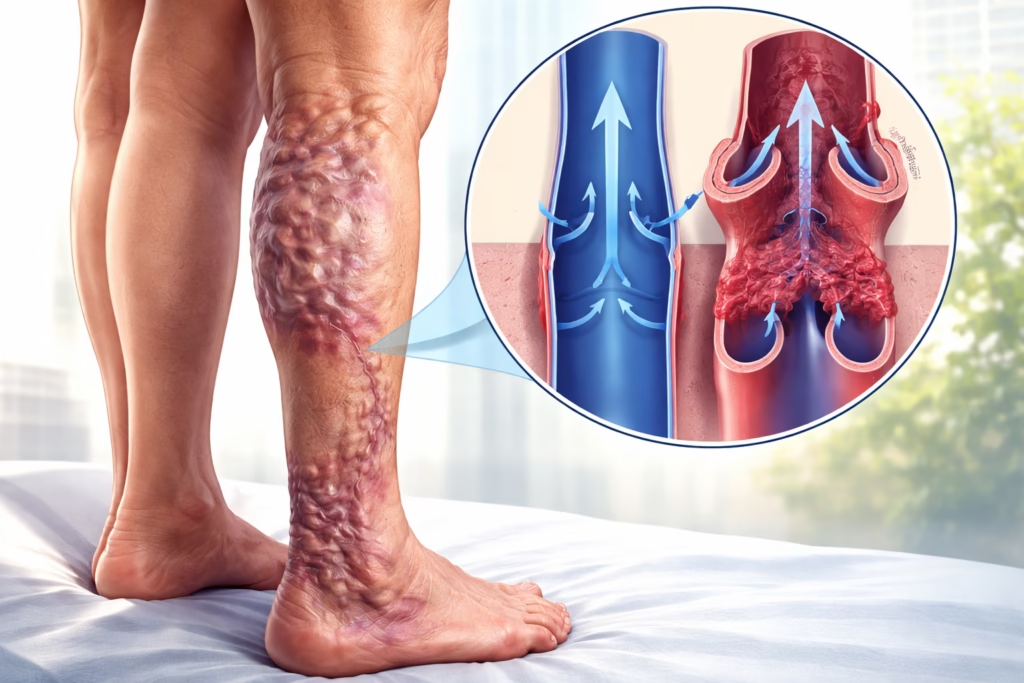
Venous hypertension is a chronic vascular condition that develops when pressure within the veins, particularly in the lower limbs, becomes abnormally elevated. Although less widely discussed than arterial hypertension, it is clinically significant because it can progressively damage veins, skin, and surrounding tissues if not identified early.
- Leg swelling, often pitting, increases through the day due to fluid accumulation in ankles, feet, and lower legs.
- Dull, heavy aching or nighttime muscle cramps improve with leg elevation and reflect increased venous pressure.
- Reddish brown or purplish discoloration, dry itchy skin, and shiny tight skin indicate stasis dermatitis and ongoing tissue damage.
- Enlarged twisted varicose veins and spider telangiectasia signal vein dysfunction and may cause aching, burning, or fullness.
- Chronic venous ulcers near the inner ankle heal poorly, show persistent drainage and surrounding discoloration, requiring long term care.
Individuals may initially notice subtle symptoms such as mild swelling or skin discoloration around the ankles. However, without intervention, these early signs can evolve into persistent pain, skin breakdown, and venous ulcers. Therefore, understanding each symptom in detail is essential for timely recognition and appropriate management.
This article provides a comprehensive explanation of venous hypertension, its causes, symptoms, diagnostic approaches, and treatment strategies, with each point fully elaborated to ensure clarity and practical understanding.
Understanding Venous Hypertension
Definition
Venous hypertension occurs when the normal return of blood from the legs to the heart is impaired. Under healthy conditions, veins contain one way valves that prevent blood from flowing backward. When these valves become damaged or weakened, blood begins to pool in the lower limbs. This pooling increases pressure within the veins, leading to venous hypertension.
Causes
Several underlying conditions contribute to this dysfunction.
Chronic venous insufficiency (CVI):
This is the most common cause. It develops when vein valves fail to close properly, allowing blood to flow backward and accumulate in the legs.
Deep vein thrombosis (DVT):
A previous blood clot in the deep veins can damage the vein walls and valves. Even after the clot resolves, the residual damage may impair blood flow and lead to long term pressure elevation.
Prolonged inactivity:
Extended periods of sitting or standing reduce the effectiveness of the calf muscle pump, which normally helps push blood upward toward the heart. Without this movement, blood tends to pool in the lower extremities.
Risk Factors
Certain factors increase the likelihood of developing venous hypertension.
- Age: Vein elasticity and valve function decline over time
- Obesity: Excess body weight increases pressure on leg veins
- Family history: Genetic predisposition may affect vein structure and function
- Pregnancy: Increased blood volume and hormonal changes can weaken vein walls
- Occupational factors: Jobs requiring prolonged standing or sitting contribute to poor venous return
Early recognition of symptoms in individuals with these risk factors is particularly important to prevent progression.
Common Symptoms of Venous Hypertension
Leg Swelling (Edema)
Leg swelling is one of the earliest and most noticeable signs of venous hypertension.
This swelling usually appears in the ankles, feet, and lower legs and tends to worsen as the day progresses. The reason for this pattern is that gravity causes blood and fluid to accumulate in the lower extremities when a person is standing or sitting for long periods.
In many cases, pressing a finger into the swollen area leaves a temporary indentation, a condition known as pitting edema. This occurs because excess fluid has leaked from the veins into surrounding tissues.
Over time, persistent swelling can stretch the skin, reduce circulation, and increase the risk of skin damage.
Pain, Aching, or Muscle Cramps
Individuals with venous hypertension often report a dull, heavy, or throbbing pain in the legs. This discomfort is caused by increased pressure within the veins and reduced oxygen delivery to tissues.
Muscle cramps, particularly at night, are also common. These cramps occur due to impaired circulation and accumulation of metabolic waste in the muscles.
A key feature of venous related pain is that it typically improves when the legs are elevated. Elevation reduces venous pressure by allowing blood to flow more easily back toward the heart.
Skin Changes and Discoloration
As venous hypertension progresses, it begins to affect the skin.
One of the most characteristic changes is the development of reddish brown or purplish discoloration, especially around the ankles. This occurs due to leakage of red blood cells from damaged veins, which then break down and deposit pigments in the skin.
Other changes include:
- Dry and itchy skin: Reduced circulation leads to poor skin hydration
- Flaking or cracking: The skin becomes fragile and prone to irritation
- Shiny, tight appearance: Chronic swelling stretches the skin, making it appear smooth and taut
These changes are collectively referred to as stasis dermatitis, and they indicate ongoing tissue damage.
Varicose Veins and Telangiectasia
Venous hypertension often leads to visible changes in the veins.
Varicose veins appear as enlarged, twisted, and bulging veins just beneath the skin. They form because increased pressure causes veins to stretch and lose their normal shape.
Telangiectasia, also known as spider veins, are smaller, thin, red or blue lines that appear near the surface of the skin. While often considered cosmetic, they may indicate underlying venous dysfunction.
Both conditions can be associated with discomfort, including aching, burning, or a sensation of fullness in the legs.
Leg Ulcers
One of the most severe complications of venous hypertension is the development of venous ulcers.
These ulcers typically form near the inner ankle, where pressure and fluid accumulation are greatest. They may begin as minor skin injuries or areas of irritation but gradually deepen and fail to heal due to poor circulation.
Venous ulcers are often characterized by:
- Persistent drainage
- Surrounding skin discoloration
- Foul odor in advanced cases
These wounds can significantly affect quality of life and require long term medical care.
Heaviness and Fatigue in the Legs
A common but often overlooked symptom is a sensation of heaviness or fatigue in the legs.
Individuals may feel that their legs are unusually tired even after minimal activity. This occurs because inefficient blood flow reduces oxygen delivery and increases pressure within the veins.
As a result, daily activities such as walking, standing, or exercising may become more difficult, leading to reduced physical activity and further worsening of symptoms.
Additional Symptoms (Less Common)
Some individuals may experience less frequent but still important symptoms.
- Itching or burning sensations: Caused by skin inflammation and irritation
- Restless legs: An uncomfortable urge to move the legs, often accompanied by tingling
- Numbness or tingling: Resulting from impaired circulation affecting nerve function
Although these symptoms may appear mild, they can indicate progressing venous dysfunction and should not be ignored.
How Venous Hypertension Differs from Arterial Hypertension
It is important to distinguish venous hypertension from arterial hypertension.
Arterial hypertension refers to high pressure within the arteries, which carry oxygen rich blood from the heart to the body. It is commonly associated with cardiovascular risk factors such as heart disease and stroke.
Venous hypertension, in contrast, involves elevated pressure within the veins, particularly in the legs. It is primarily related to impaired blood return and valve dysfunction rather than systemic blood pressure.
Because the underlying mechanisms differ, the treatment approaches are also different. Confusing the two conditions may delay appropriate management.
When to See a Doctor
Medical evaluation is essential when symptoms persist or worsen.
Seek medical attention if you experience:
- Ongoing or increasing leg swelling
- Skin changes that do not improve
- Open wounds that fail to heal within two weeks
- Sudden pain, redness, or warmth in one leg, which may indicate a blood clot
- Symptoms appearing after surgery or prolonged immobility
Early consultation allows for proper diagnosis and prevents complications.
Diagnosis and Tests
Physical Examination and History
A healthcare provider will begin by evaluating symptoms, medical history, and risk factors. Observation of swelling, skin changes, and visible veins provides important initial clues.
Doppler Ultrasound
This is the most commonly used diagnostic test. It uses sound waves to assess blood flow and evaluate the function of vein valves. It helps identify areas of reflux or obstruction.
Venography
In more complex cases, a contrast dye is injected into the veins and X ray imaging is used to visualize blood flow. This provides detailed information about vein structure.
Ankle Brachial Index (ABI)
This test compares blood pressure in the ankle and arm to rule out arterial disease. It is important because treatment approaches differ between arterial and venous conditions.
Management and Treatment Options
Lifestyle Modifications
Lifestyle changes play a central role in managing venous hypertension.
Leg elevation:
Elevating the legs above heart level for 15 to 20 minutes several times a day reduces venous pressure and improves circulation.
Regular movement:
Taking breaks to walk activates the calf muscles, which help pump blood upward.
Weight management:
Maintaining a healthy weight reduces pressure on the veins.
Exercise:
Activities such as walking, cycling, or calf strengthening exercises improve circulation and muscle function.
Compression Therapy
Compression stockings apply graduated pressure to the legs, with the highest pressure at the ankle.
This helps:
- Improve blood flow toward the heart
- Reduce swelling
- Prevent progression of symptoms
Regular use during the day is often recommended for long term management.
Medications
Certain medications may be used to manage symptoms.
- Venoactive drugs: Strengthen vein walls and improve circulation
- Diuretics: Reduce fluid buildup, typically for short term use
- Topical treatments: Relieve itching and inflammation associated with skin changes
Medication use depends on individual patient needs and clinical evaluation.
Minimally Invasive Procedures
Modern treatments can address damaged veins without major surgery.
- Endovenous laser therapy (EVLT): Uses heat to close affected veins
- Radiofrequency ablation (RFA): Similar to EVLT but uses radiofrequency energy
- Sclerotherapy: Injects a solution that collapses and seals small veins
These procedures redirect blood flow to healthier veins and reduce symptoms.
Surgical Options
In advanced cases, surgical intervention may be necessary.
- Vein stripping or phlebectomy: Removal of damaged veins
- Vein bypass surgery: Used in rare and severe cases
Surgery is typically considered when other treatments are ineffective.
Prevention Tips
Preventive measures can reduce the risk of developing or worsening venous hypertension.
- Engage in regular physical activity to promote circulation
- Avoid sitting or standing for prolonged periods without movement
- Wear supportive footwear to reduce strain on the legs
- Avoid crossing legs for extended periods
- Schedule regular medical checkups if risk factors are present
These strategies help maintain healthy blood flow and prevent pressure buildup in the veins.
Conclusion
Venous hypertension is a progressive condition that can lead to significant complications if left untreated. Symptoms such as swelling, pain, skin changes, and ulcers should be recognized early and addressed promptly.
Through a combination of lifestyle modifications, medical management, and appropriate interventions, individuals can effectively control symptoms and improve quality of life. Early detection and proactive care remain the most effective strategies for preventing long term damage and maintaining vascular health.